In keeping with many other countries in sub-Saharan Africa, Ethiopia has a chronic lack of hospitals and doctors. Nadia Ashraf and Tim Crocker-Buqué tell us about a project which aims to improve training in ENT, in a hospital that has never had an otolaryngologist.

Aksum University Referral Hospital.
Ethiopia has a severe shortage of doctors and, particularly, hospital-based specialists. In 2010, there were only 5000 doctors in the country serving a population of over 90 million. This is compared to 150,000 doctors in the UK for a population of 64 million.
More than half of the physicians in Ethiopia are based in the capital, Addis Ababa, and there is little provision for those in less developed areas like Aksum. There are very few ENT surgeons practising in the country and fewer still involved in teaching and training.
In order to try and combat the shortage of doctors, particularly in rural areas, in 2011 the Ethiopian Government opened 13 new medical schools. This included the University of Aksum Medical School in the Tigray region in the northeastern part of the country. The Aksum Medical School has 60 medical students per year, and the first cohort graduated in 2016.
“Since Aksum had never seen an ENT specialist, our objectives were broad-ranging.”
The partnership between Barts and the London School of Medicine and the University of Aksum Medical School was established in 2013, with the aim of supporting undergraduate teaching and later developing into postgraduate training and clinical support of specialist services. The partnership is funded by The Tropical Health Education Trust (THET) through the Department for International Development (DFID) Health Partnerships Scheme.

The ENT Team at Aksum. (L-R): Bereket (Medical student), Ebrahim (GP),
KimberleyLau (ENT SpR) and Nadia Ashraf (Post-CCT ENT Fellow).
The Aksum University Referral Hospital was opened in May 2016 to provide tertiary services to the surrounding rural population of more than 1.2 million, but currently lacks many specialist services that we take for granted in the UK. The hospital currently provides basic services in internal medicine, surgery, paediatrics, obstetrics and gynaecology.
Since Aksum had never seen an ENT specialist, our objectives were broad-ranging: to set up a fledgling ENT outpatient service, train local GPs to deliver basic ENT care, develop an undergraduate ENT training programme and generate some surgical cases for future visits. Our two-surgeon ENT team travelled with a group of two ICU specialists, one ICU nurse and two general surgeons, along with our team leader, a public health specialist. The ICU team were faced with setting up a brand new ICU service, and the general surgical team with providing sub-specialist training to the existing local surgeons.
As fate would have it, we were presented with the perfect emergency ENT case to bring together many of our team’s joint objectives. Our patient was a 22-year old presenting with a two-week history of a sore throat and fever, developing into widespread neck swelling and airway obstruction. He was transferred from the local government hospital, having been heroically intubated by one of the medical officers there, despite his severe trismus. Clinical examination revealed a septic patient with a fluctuant abscess in the right side of the neck. A previous drainage site on the left side of the neck was visible, reportedly having produced 50ml of pus. The only imaging available to us was a bedside ultrasound scan, which duly confirmed the collection and patent neck vessels.
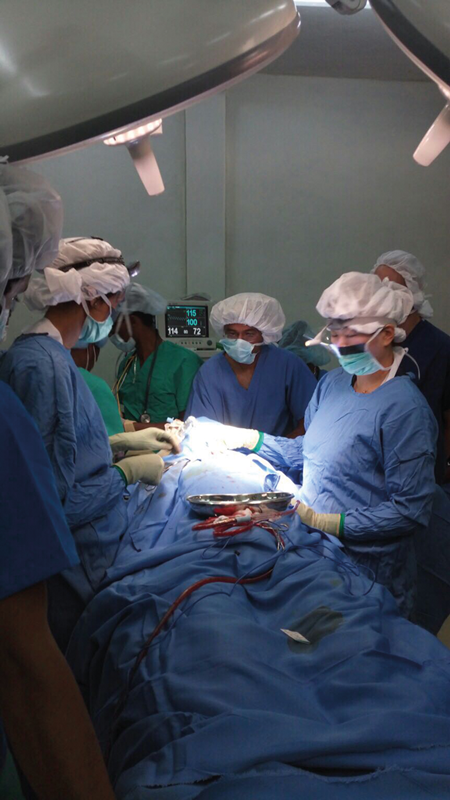
Operating on a young patient with deep neck space collection.

Teaching medical students anatomy of the ear.
We proceeded with the patient to the operating theatre, using the opportunity to train the local surgeons on deep neck space infection and the surgical approach to treat this life-threatening condition. We found an extensive para- and retro-pharyngeal collection and resultant fistula into the hypopharynx. Along with drainage of the collection, we performed a tracheostomy; another ideal teaching opportunity for the local surgeons, who had not performed a surgical airway before.
The postoperative care of our patient on ICU was the ideal case for our ICU colleagues to develop protocols for ventilation, fluid / electrolyte balance and sepsis control. The local nursing staff and doctors enthusiastically took up the opportunity to develop skills and knowledge in ICU care.
Throughout our two-week visit, we ran twice-daily outpatient clinics, following a local advert for any patients with ENT complaints to visit the hospital. We found a large burden of chronic otitis media and developed a sizeable database of patients that could potentially benefit from future tympanoplasty. We saw some interesting pathology, including HIV-related oropharyngeal malignancy, a case of nasal osteoma, multiple thyroid goitres and cutaneous leishmaniasis.
We had an extremely competent and enthusiastic nurse assisting us in the clinic. He diligently translated our English into Amharic or Tigrinya, depending on the patient’s background. He also patiently explained the unique Ethiopian time and calendar system to us. Ethiopia use a unique calendar, similar to the Julian calendar, which we discovered when we saw all the notes dated as May 2009, despite being in January 2017 (Gregorian calendar)! This caused no end of confusion and hilarity to begin with, but by the end of our stay, we were fluently writing the Ethiopian date in the notes and had no idea what the Gregorian date was! To add to the confusion, Ethiopian time is generally six hours behind universal time, so it was always wise to double-check when booking a case for theatre!
During our two-week stay, we developed and delivered an undergraduate ENT teaching programme to a group of 26 final-year medical students. This included lecture-based teaching on ENT anatomy and pathology and, most importantly, clinical examination skills training. Together with our ICU colleagues, we ran an airway simulation workshop covering basic and advanced airway management, intubation skills and emergency surgical airway, which was very enthusiastically received.
Aksum is one of the oldest continuously-inhabited places in Africa, having been the seat of the Akumsite Empire and, accordingly, has a number of historic sites. At weekends, we managed to see a number of historic churches, including: the Church of Our Lady Mary, said to hold the Ark of the Covenant; stelae from the Akumsite Kingdom; and the Queen of Sheba’s Bath.
“As fate would have it, we were presented with the perfect emergency ENT case to bring together many of our team’s joint objectives.”
We also made a trip to Lalibela; a world heritage site of stunning rock-hewn churches. From there, we headed into the Ethiopian Highlands to stay in a remote mountain lodge without running water or electricity, which required a two-hour uphill hike to reach. We also did a number of day hikes and visited a mountain village for delicious freshly-brewed Ethiopian coffee and the local delicacy, injera.
By the time of going to press, the next visit in April 2017 would already have gone ahead, with further outpatient work and teaching, as well as expansion of the ENT surgical service. If anyone is able to help, particularly in providing surgical kit for future visits, we would be very grateful. We are particularly looking to start an audiology service and therefore audiologists who can help, particularly if you have a stock of old hearing aids or an audiometer going spare, please do get in touch!
Our ongoing overriding objective remains to increase the number of ENT surgeons and ENT-trained GPs in Ethiopia through ongoing teaching and training, which will no doubt be a slow but hopefully rewarding process.
Acknowledgements: Sincere thanks to SheffMed© for providing ENT equipment to support our work in Aksum.





