Drooling can be a challenging problem to manage in paediatric ENT. The variety of medical and surgical treatments suggests that there is no gold standard treatment. Nicola Stobbs and Ravi Thevasagayam describe an approach to ligating the salivary ducts.
Drooling is a common and complex issue seen in paediatric ENT clinics. Children who are developmentally normal may drool and this can be expected to resolve spontaneously as the child gets older. Typically, abnormal drooling is a manifestation of impaired salivary control, usually caused by impaired neurological function. Almost two thirds of children with cerebral palsy drool [1].
True hypersalivation is much less common and may be seen in reflux, dental disease and certain drugs, such as anticonvulsants. All medical and surgical treatments are aimed at reducing saliva flow rather than addressing the primary pathology and, as such, will always be limited in their effectiveness. The difficulty in accurately measuring saliva production and the complexity of the patient group has led to challenges objectively assessing responsiveness to treatment modalities. That said, reducing the salivary load can be seen to improve the ability of the patient to manage the residual saliva.
Why treat drooling?
Drooling can be unhygienic causing soiling of clothes, toys and electronic devices. Perioral soreness and maceration, both from the wetness and the constant wiping, can be very uncomfortable which can also be unappealing to other children and lead to social isolation. Aspiration of retained secretions may result in recurrent chest infections. It is generally acknowledged that drooling can have a significant adverse impact on the child’s quality of life and increase the burden on their caregiver.
“Salivary duct clipping has no risk of potential aspiration when compared to duct relocation and appears to be associated with less postoperative morbidity.”
Assessment
A full history looking particularly at drug history, nasal congestion (which may promote a mouth open posture) and reflux symptoms should be taken. Previous failures to other modalities of treatment will guide treatment. Examination is particularly focused on dental and periodontal disease. If a child’s diagnosis is unknown but they are making gains in development, it may be wise not to embark on irreversible procedures.
Treatment options
In an otherwise normally developing child, drooling should not be treated and the parents should be reassured that the expectation is towards resolution with time.
Speech and language therapy input with oro-motor physical therapy, behavioural techniques or intra-oral appliances may be helpful [2]. These may be limited by the child’s level of function, but simple measures such as avoiding a head down posture and barrier emollients to the lips and chin can help.
Anticholinergic medications are in widespread use. These medications are not selective and can lead to unwanted neurological side-effects [3]. When delivered by a patch, skin reactions are common. It is also a widely-held belief that these drugs sometimes thicken secretions, making them harder to cough up and exacerbating chest disease.
Intra-glandular injection of botulinum toxin is rising in popularity. This inhibits acetylcholine release at the neuro-glandular junction and reduces gland salivary production but this effect is transient. Results are generally good [4] but the requirement for repeated injections and the risk of post-Botox dysphagia makes this unattractive for some patients.
The mainstays of surgical interventions have been submandibular duct relocation and bilateral submandibular excision. Both of these procedures come with significant morbidities and in-patient stay. In 1999 Klem and Mair described submandibular and parotid duct ligation [5]. This approach involved intra-oral identification and ligation of the ducts of the major salivary glands. Subsequent series have suggested good outcomes [6,7]. The technique is attractive as it has low morbidity and can be done as a day case procedure in about 45 minutes. The technique is simple and well within the capacity of any ENT surgeon.
Technique
The operation is performed under general anaesthetic, in the supine position with neck extension and intubated ideally with a naso-tracheal tube. Surgical loupes are used (magnification x2.5) and the oral cavity is kept open with dental blocks or a Doyen mouth gag. All four ducts are ligated in one sitting, preventing the need for multiple attendances and anaesthetics. Antibiotics are not routinely administrated and patients have no oral intake restrictions postoperatively.
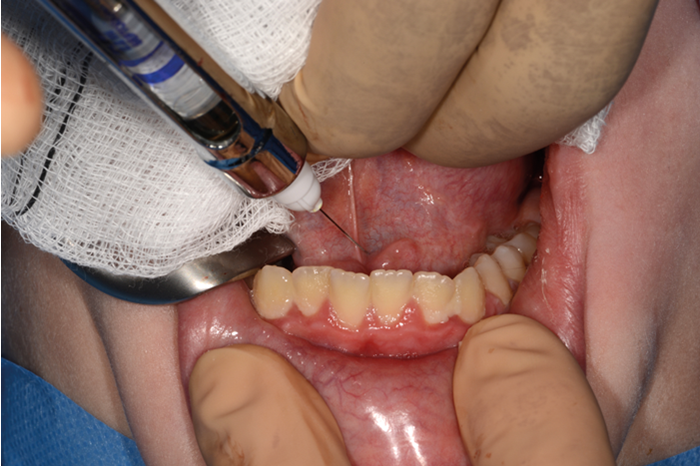
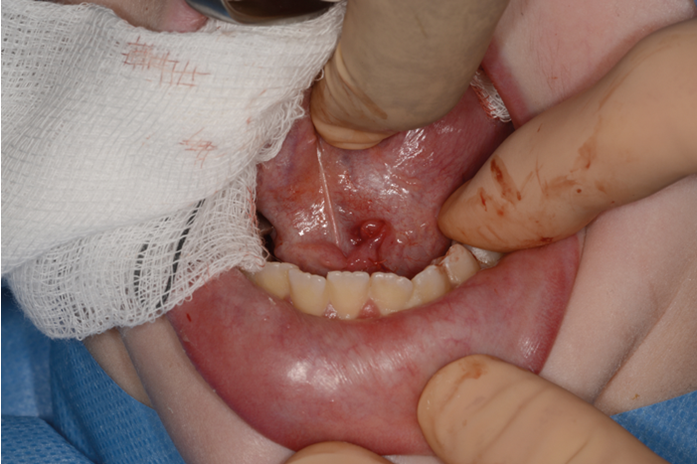
Figure 1. Floor of mouth local anaesthetic infiltration.
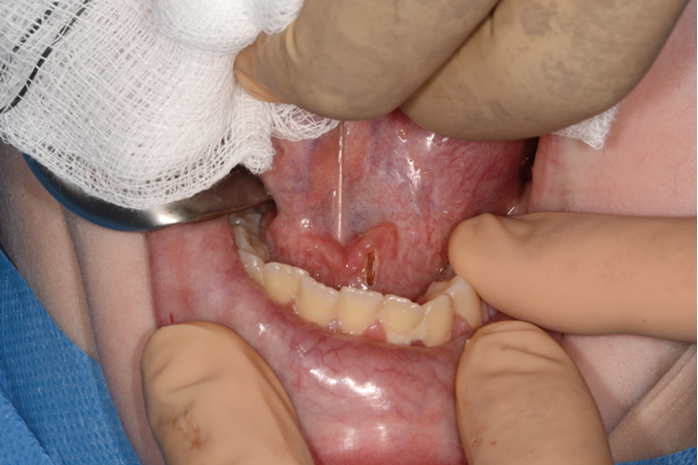
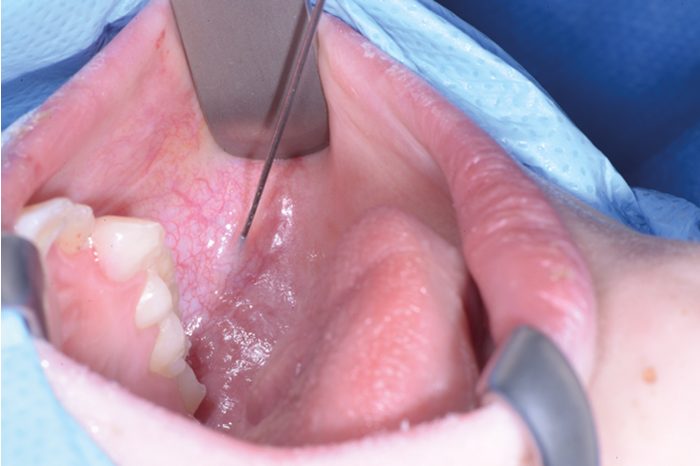
Figure 2. Mucosal incision.
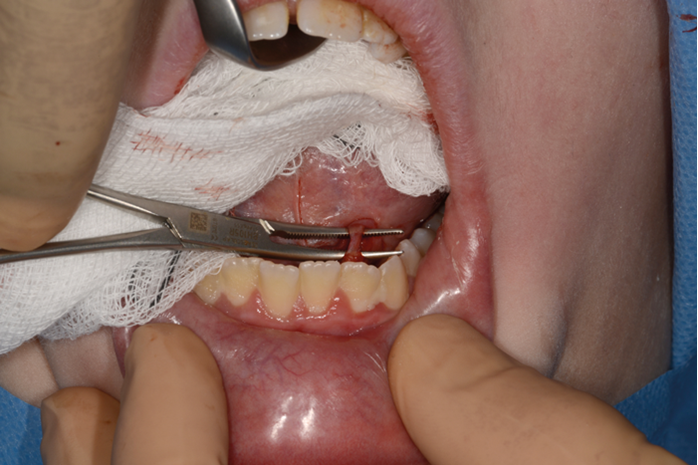
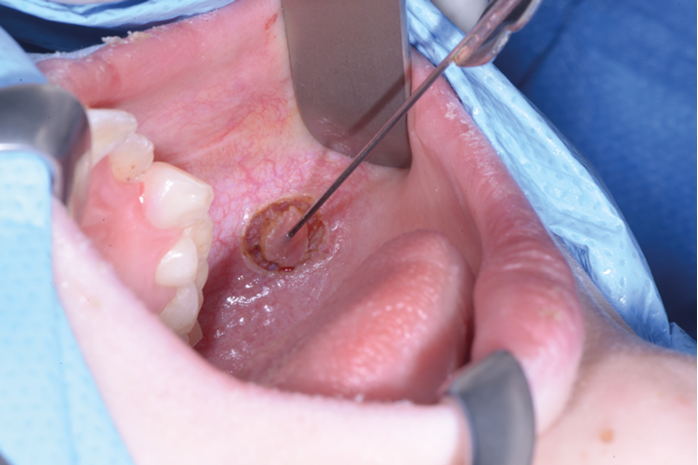
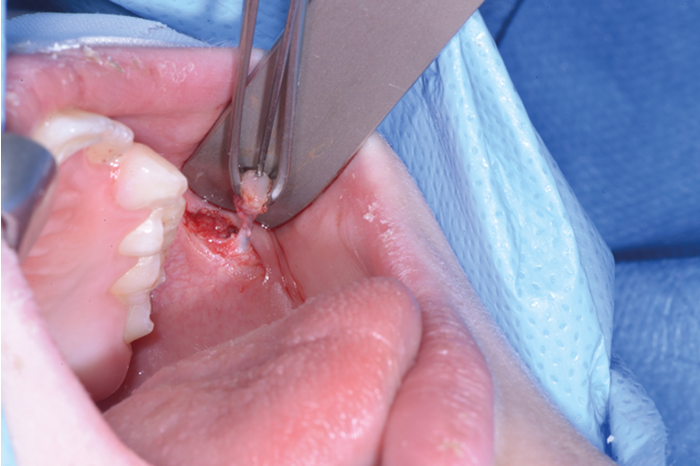
Figure 3. Skeletonisation of duct.
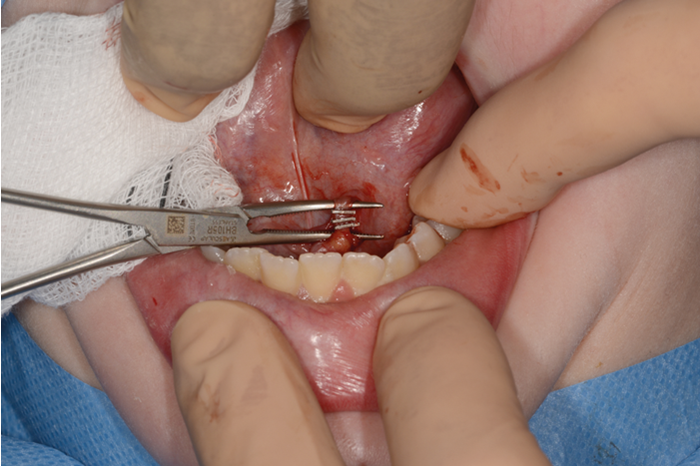
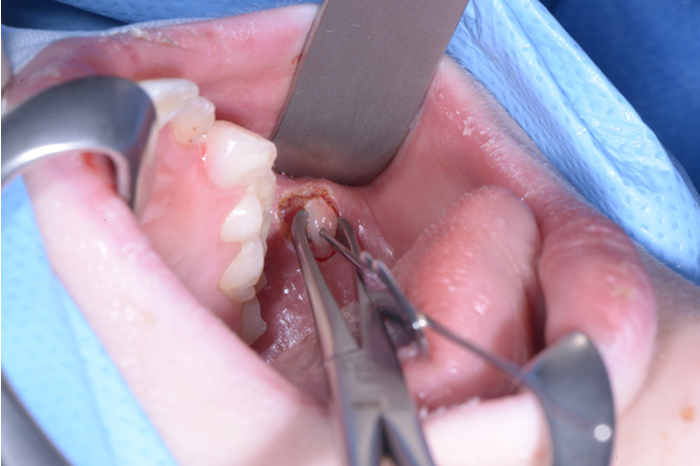
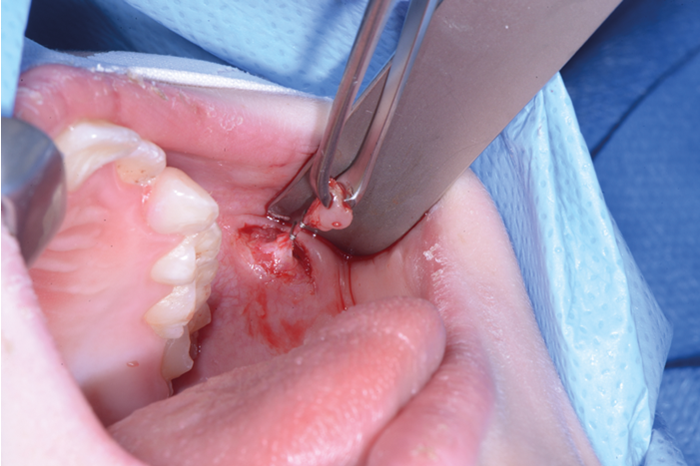
Figure 4. Clipping of duct.
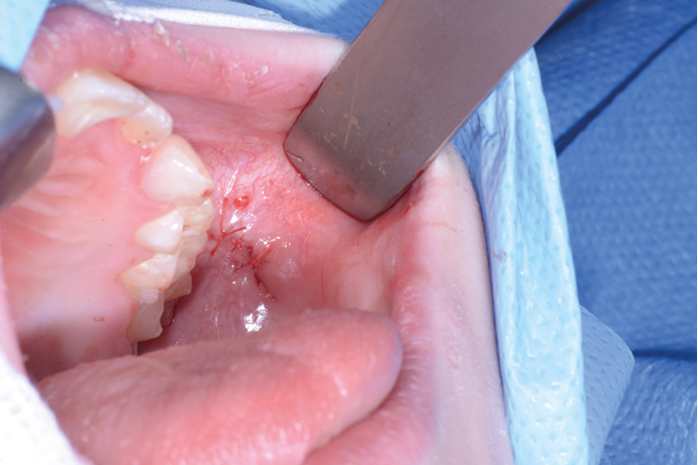
Figure 5. Closure with 5.0 vicryl.
Submandibular clipping
2% lignocaine 1:80000 adrenaline via dental syringe and needle is used for infiltration of the floor of the mouth (see Figure 1). The sublingual papilla (opening of Wharton’s duct) and the plica sublinugualis are identified and halfway between the two landmarks, a superficial mucosal incision is made using needle-point-monopolar diathermy (see Figure 2). Care must be taken not to make this initial incision too deep so as to prevent injury to the duct. Blunt dissection is then performed to identify the duct which is then skeletonised and a length of 0.5cm of the duct is cleared from surrounding connective tissues (see Figure 3). Vascular clips (Ligaclips, No. 100) are applied to the duct, one distal and two proximally (see Figure 4) and then the duct is divided. The mucosal incision is then closed with 5.0 vicryl (see Figure 5).
Figure 6. Lacrimal probe used to identify opening of Stenson’s duct.
Figure 7. Circular incision with monopolar needle.
Figure 8. Allis forceps grasping surrounding mucosa and cannulated duct.
Figure 9. 0.5cms of duct skeletonised.
Figure 10. Clips applied to duct.
Figure 11. Mucosal incision closed with 5.0 vicryl.
Parotid duct clipping
The Stensen duct orifice is identified adjacent to the second upper molar on the buccal mucosa and cannulated using a lacrimal probe, which can prove difficult to identify in children with craniofacial abnormalities due to altered anatomy (see Figure 6). The area around the duct is infiltrated with 2% lignocaine 1:80000 adrenaline via dental syringe and needle. A circular incision is made around the opening using a monopolar needle (see Figure 7). Care must be taken to not go too deep, superficial to the probe as the duct may be injured. Once the incision is complete the probe in situ, along with the small island of mucosa, is grasped using an Allis clamp (see Figure 8). The soft tissue around the probe is then dissected by a combination of blunt and sharp dissections. Whilst the probe remains in the duct, this is simple to do without transecting the duct. When most of the soft tissue is removed the probe can be seen through the duct clearly. At this point the allis is removed and the probe withdrawn. The mucosal island is grasped with forceps and two vascular clips are applied (see Figure 10). The duct opening is buried and the mucosal incision is closed with 5.0 vicryl (see Figure 11).
The incisions, particularly in the cheek, should be closed accurately to prevent the patient from chewing on it. The mouth is washed and, after a short period of observation to ensure recovery from anaesthesia, the patient is discharged home.
Outcomes
Klem and Mair, originally described salivary ligation in a series of five patients in 1999 [5]. They reported a substantial decrease in drooling in all five patients. Following this in 2003, Shirley et al reported that salivary duct clipping was successful in 81% of their 21-patient series using a subjective post-procedure questionnaire [6]. Hakim et al retrospectively reviewed a series of 18 patients in 2008 and found a significant reduction in the number of bibs and shirts used (P<.001), an improvement in circumoral skin problems, choking episodes and aspiration and a positive impact on the mean Glasgow Children’s Benefit Index (GCBI) [7]. More recently, Scheffer et al reported significant reduction in both drooling quotient score and caregivers visual analogue scale in a series of 21 patients [14].
Potential complications
Clipping obstructs the salivary ducts and concerns were raised about potential postoperative sialadenitis or post-prandial pain and swelling. Postoperative transient neck swelling was noted in all 21 patients in Shirley’s series. However, there were no similar issues reported by Hakim et al nor Klem et al.
Our experience in Sheffield is that the postoperative period is uneventful, and gland swelling is unusual. Clipping of the ducts may lead to functional atrophy of the glands. This mechanism has been confirmed in the literature with decreased uptake in technetium 99m albumin aggregate scans after duct clipping [5].
Comparison to medical treatments
Medical treatments are an alternative to salivary clipping; however failure occurs in up to two thirds of patients that subsequently undergo clipping [7]. The two main medical treatments are botulinum toxin injections and anticholinergic medications.
There is good evidence for the efficacy of botulinum toxin [4], but the effects are temporary, meaning frequent hospital trips for already complex children and potentially multiple anaesthetics as described in a series of 45 children by Jongerius et al [8], in comparison to one anaesthetic for clipping surgery.
Anticholinergic medication can be in the form of oral liquids, tablets or transdermal patches and a systematic review found some evidence that benztropine, glycopyrrolate, and benzhexol hydrochloride are effective in the treatment of drooling but could not make firm conclusions [3]. Although these medications are a non-invasive conservative option, they are not without complications and patients often get autonomic-system-mediated side-effects including blurred vision, constipation, urinary retention, sedation, irritability, headache and increase in frequency of seizures [9].
Comparison to surgical treatments
There are many other surgical approaches for control of sialorrhoea, the most described being submandibular duct relocation which has good results, with up to 87% patients having improvement in drooling and 57% of patients having complete cessation [10]. However, whereas clipping is relatively pain-free and undertaken as a day-case procedure, duct relocation can be associated with severe postoperative pain and in-patient stay [11]. Ranula formation is a postoperative issue [12] with re-routing surgery and some patients have ongoing swelling requiring submandibular excision [10]. In addition, this type of surgery is contraindicated in potential aspirators. Many of the patients requiring drooling intervention are at risk of aspiration and in this patient population salivary clipping has no risk of aspiration and appears to be the safer and less invasive option.
“Our experience in Sheffield is that the post operative period is uneventful and gland swelling is unusual.”
Submandibular gland excision is a commonly performed procedure. However, there is up to a 36% risk of temporary marginal mandibular weakness with up to 7% of patients having a degree of permanent weakness [13] and the hypoglossal, lingual and facial nerves are also at risk. In a patient population with poor oro-motor coordination and communication difficulties, this risk is something best avoided.
Major salivary duct clipping has been shown to be effective in various series [5-7, 14] and is an efficient, safe and permanent method of controlling drooling in complex children with minimal side-effects and a positive impact on their quality of life.
References
1. TahmassebiJ F, Curzon M. Prevalence of drooling in children with cerebral palsy attending special schools. Dev Med Child Neurol 2003;45(9):613-7.
2. Walshe M, Smith M, Pennington L. Interventions for drooling in children with cerebral palsy. Cochrane Database of Systematic Reviews 2012:(11), Art. No.: CD008624.
3. Jongerius PH, van Thiel P, van Limbeek J, et al. A systematic review for evidence of efficacy of anticholinergic drugs to treat drooling. Archives of Disease in Childhood 2003;88:911-4.
4. Reid S, Johnstone B, Wesstbury C, et al. Randomized trial of botulinum toxin injections into the salivary glands to reduce drooling in children with neurological disorders. Developmental Medicine & Child Neurology 2008;50:123-8.
5. Klem C, Mair EA. Four-duct ligation: a simple and effective treatment for chronic aspiration from sialorrhea. Arch Otolaryngol Head Neck Surg 1999;125(7):796-800.
6. Shirley WP, Hill JS, Woolley AL, Wiatrak BJ. Success and complications of four duct ligation for sialorrhea. Int J Pediatr Otorhinolaryngol 2003;67(1):1-6.
7. Hakim E, Richards S, Thevasagayam M. Major Salivary Duct Clipping for Control Problems in Developmentally Challenged Children. Arch Otolarnygol Head Neck Surg 2008;134(5):470-4.
8. Jongerius P, van der Hoogen F, Limbeek J, Fons G, van Hulst K, Rotteveel J. Effect of Botulinum Toxin in the Treatment of Drooling: A Controlled Clinical Trial. Pediatrics. 2004;114(3):620-7.
9. Fairhurst C, Cockerill H. Management of drooling in children. Arch Dis Child Educ Pract Ed 2011;96:25-30.
10. Uppal, H. De R, D’Souza A, Pearman K, Proops D. Bilateral submandibular duct relocation for drooling: an evaluation of results for the Birmingham Children’s Hospital. European Archives of Oto-Rhino-Laryngology. 2003; 260(1);48-51.
11. Panarese A, Ghosh S, Hodgson D, McEwan J, Bull PD. Outcomes of submandibular duct re-implantation for sialorrhoea. Clin Otolaryngol Allied Sci. 2001;26(2):143-6.
12. Mankarious L, Bottrill I, Huchzermeyer P, Bailey C. Long-term follow-up of submandibular duct rerouting for the treatment of sialorrhea in the pediatric population. Otolaryngol Head Neck Surg. 1999;120(3):303-7.
13. Smith W, Markus A, Peters W. Submandibular gland surgery: an audit of clinical findings, pathology and postoperative morbidity. Ann R coll Surg. 1993;75:164-7.
14. Scheffer A, Bosch K, van Hulst K, van den Hoogen. Salivary duct ligation for anterior and posterior drooling: Our experience in twenty-one children. Clin Otol. 2013;38(5):425-9.