There are successful models for delivering complex ear surgery where resources may be more limited.
Ear, nose and throat conditions are frequently overlooked when global health issues are considered, but hearing loss is the world’s most common sensory deficit, and hearing impairment is more prevalent in Sub-Saharan Africa than in other parts of the world [1].
It is likely that levels of hearing loss are under-reported in these settings when countries have no access to hearing assessment or the management of identified hearing loss. This, in turn, means children suffering will have speech and educational delay, impacting countries that are not in an economic position to support this.
Whereas the ideal model is locally-led and delivered ear and hearing care, in many low- and middle- income countries, otological surgery is either non-existent or in its infancy. Outreach is one model that can help fill this gap, and should of course be married with meaningful attempts at local capacity development. I recently had the opportunity of talking to four colleagues in the UK and abroad about the challenges of developing otological outreach services and delivering surgical ear care in low-resource settings...
“Despite the long distances travelled, 70-80% of patients operated on after an ear camp return to the next camp for follow-up three months later”
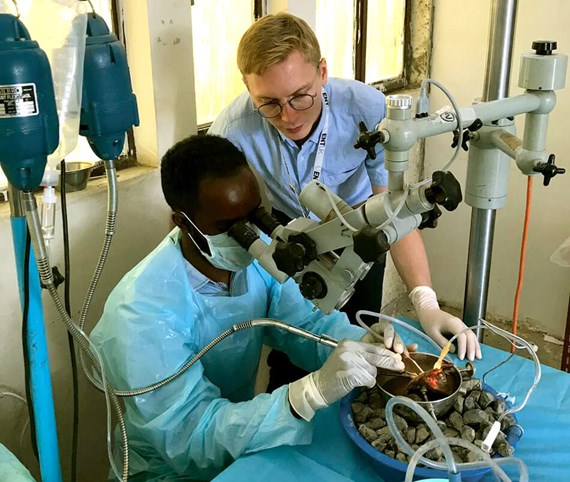
Misha Verkerk (right) at an ear training camp in the Tigray region of Ethiopia.
Mr Misha Verkerk is an ENT Speciality Registrar in London, recently winning ENT UK’s rising star award at BACO 2021. He works with the charity Global ENT Outreach (GEO) and has developed a twice-yearly ear training camp and outreach service in the Tigray region of Ethiopia. I asked him about his experiences in both Mekelle, Ethiopia, and the Ukraine where he has worked with the charity. Misha felt that the biggest difficulties he had faced were finding the person or groups of people that would champion otological services in a country or hospital, and specifically those who wanted to develop the service with the help of external surgeons. Without the desire in a unit for this work to be undertaken it would be near impossible to progress, and rightfully so, as it is entirely inappropriate as an external body to tell communities what they need unless this opinion has been sought.
Misha went on to tell me that developing a regular training camp for in-country surgeons requires sustained commitment from the hosting institution with their doctors giving up free time, and that routine work frequently needs to be reduced. This must be recognised, as often visiting teams will not be the only group of doctors that support a department with in-person outreach work.
“Outreach is one model that can help fill this gap, and should of course be married with meaningful attempts at local capacity development”

Dr Sok Davy Touch, Cambodia.
The ENT surgeons in Mekelle do not have access to a community of colleagues for support and dialogue; something we take for granted in the UK. This was an issue also raised by Otologist, Dr Sok Davy Touch, in Cambodia. Her hospital, the Children’s Surgical Centre (CSC) in Phnom Penh is an NGO and has found recruitment hard. At present, she is the only surgeon delivering ear care in the hospital, as the government medical facilities receive better funding and salaries. Recently COVID has also impacted patient management, as charging for treatment needed to be introduced because donor payments stopped at the start of the pandemic when the county’s economic situation became precarious.
The charge introduced has prevented patients from accessing otological services and COVID has meant patients are also reluctant to travel for treatment and the management of their chronic ear conditions. This further reduction in revenue has also affected the hospital’s ability to recruit staff. Davy told me that working as the only otologist is “lonely; we all need to discuss patients and sometimes we need help and advice with the more complicated cases”.
Many of you will know Mr Robin Youngs and Mr Mike Smith, two British ENT surgeons who have worked in Nepal intermittently for many years. They shared their experiences of setting up and maintaining otological services through the Britain Nepal Otology Service (BRINOS) in Nepalgunj and The Ear Care Centre at Green Pastures Hospital, Pokhara with me. Both surgeons also addressed the difficulties of funding humanitarian hearing and otological health work, and Robin has brought the issue up publicly via Parliamentary Questions, identifying that the UK aid budget for hearing-related conditions was not known and likely to be zero: “We need to start mirroring the global health approach of ophthalmology and eye services. They have a charity infrastructure and staff that are employed to write grants and so can develop their services.
In ENT, people donate their own time and pay their air fares to support charities doing this work” which, as Misha Verkerk says, “requires great personal motivation, working outside of normal hours and giving up free time”. This isn’t sustainable long term at the levels that are needed. The British surgeons that I spoke to acknowledged that the load of humanitarian work should be shared and involve others to enable consultants and trainees to contribute.
All those that I spoke to strongly supported trainee surgeons being involved but at a level that is commensurate with their UK training. As Misha says “trainees gain a huge amount by being involved with outreach work, by teaching and facilitating the Ear Camps, but they are not there to deliver the expert service; the consultants are. They also help spread the word and encourage others to join us on subsequent trips.” The surgeons working in Nepal have identified that there have been issues with foreign nationals coming into the country and performing complex surgery on patients, leaving after a short stay, and providing inadequate follow-up which has led to difficulties both with patient management and future outreach work.
Robin Youngs rightly notes that those working in these settings from abroad need to be aware of visa rules and medical licensing: “After all, we have these rules in the UK too and we should always be respectful of the country we are working in”. Regular visits to a country enable foreign teams to develop mutually beneficial personal and professional relationships but also help the visiting teams understand cultural norms and the nuance of living in rather than visiting a place, which can only be of benefit to patient care.

Mwanaisha Phiri, Audiologist at the Queen Elizabeth Central Hospital, Blantyre, Malawi.
I have also worked in this setting during my registrar training, at the Queen Elizabeth Central Hospital, Blantyre, Malawi, with Dr Wakisa Mulwafu. The time spent there was very formative and has shaped me as a person as well as a surgeon. Whilst the department has benefitted tremendously from Dr Mulwafu’s innovative leadership and has considerably more equipment, at the time, nine years ago, there was no operating microscope. This very much opened my eyes as to what can and cannot be achieved in these working environments and is a factor that should be pre-emptively considered. Mike Smith pointed out that surgeons working in these environments need to be mindful that equipment that requires expensive maintenance is not always appropriate; consequently, training of junior surgeons should include open as well as endoscopic techniques.
In Nepal, as in other outreach settings, there is a need to work sensitively with local colleagues whose salary is dependent on providing care to the local community. Visiting surgeons impact on this and it can lead to disharmony. In Nepalgunj, BRINOS has trained community ear assistants (CEAs) and developed a model where CEAs visit remote regions within a five-day trek from the hospital prior to ear camps to recruit patients. This enables patients from the poorest areas of Nepal and India, who have no access to ear care, to be treated without disadvantaging the local doctors financially. Despite the long distances travelled, 70-80% of patients operated on after an ear camp return to the next camp for follow-up three months later.
“The ENT surgeons in Mekelle do not have access to a community of colleagues for support and dialogue; something we take for granted in the UK”
Going forward, the WHO’s World Report on Hearing [2] will improve the profile of this area of humanitarian work but, as Robin noted, “we need a major grant to improve co-ordination to prevent duplication of work”. We all know that out of adversity comes opportunity and all those I spoke to felt that, whilst the COVID pandemic had wreaked havoc on otological services, some of the challenges of remote working in resource-limited settings could be overcome with the world’s newfound connection and reliance on the internet. Let’s hope that some positives can be taken from this period of global difficulty.
References
1. Mulwafu W, Kuper H, Ensink RJH. Prevalence and causes of hearing impairment in Africa. Trop Med Int Health 2016;21(2):158-65.
2. World Health Organization. World Report on Hearing. Geneva, Switzerland. 2021.
www.who.int/publications/i/item/
world-report-on-hearing
Last accessed April 2021.




