Dr Westerberg attended a workshop on Physician Wellness hosted by Dr Osler a few years ago at our Canadian Society of Otolaryngology-Head and Neck Surgery meeting. The list of symptoms of stress and burnout resonated as typical of almost a daily state at the time and emphasised how stressful our chosen profession can be. At the same time, we chose this profession for the personal satisfaction it provides almost daily. As intimated by Dr Osler, as professionals we need to “check in…listen to…and monitor ourselves…” for the betterment of our patients
Around the world, the COVID-19 pandemic is having a significant impact on physicians’ emotional, psychological and physical wellbeing. Even before COVID-19, medicine was recognised as a demanding and high-stress profession in which physician wellness was often overlooked.
Now, physicians are faced with added stress from the unknowns of a novel coronavirus and its high transmissibility, overwhelming patient surges, lack of personal protective equipment, physical isolation, new ethical dilemmas, and keeping up to date on rapidly changing protocols and evolving health information. All these factors contribute to increased stress levels and the risk of burnout.
Recognising the unprecedented pressure on physicians resulting from the COVID-19 pandemic, the 2021 IFOS World Congress in Vancouver, Canada, will feature an all-new Physician Health, Wellness and Diversity track to raise awareness, inform, and share best practices on physician health and wellbeing.
“Physician burnout and poor mental quality of life has been correlated with increased self-assessment of medical errors, lowered patient compliance, and lowered patient satisfaction with their care”
Some people may ask: how is stress different from burnout? Stress is a state of mental or emotional strain resulting from demanding circumstances; when stress levels become too high or are prolonged, burnout becomes a risk. Burnout is a work-related, stress-induced problem characterised by emotional exhaustion, cynicism or feelings of depersonalisation, and a reduced sense of personal accomplishment. In 2019 it was defined in the 11th revision of the ‘International Classification of Diseases’ (ICD-11):
“Burn-out is a syndrome conceptualised as resulting from chronic workplace stress that has not been successfully managed. It is characterised by three dimensions:
- feelings of energy depletion or exhaustion;
- increased mental distance from one’s job, or feelings of negativism or cynicism related to one’s job; and
- reduced professional efficacy.
Burn-out refers specifically to phenomena in the occupational context and should not be applied to describe experiences in other areas of life.”
Burnout has significant impact on the individual, patient care, and healthcare systems. Physicians with burnout report decreased quality of life, worsened physical and mental health, weakened social relationships, increased likelihood of substance use, and increased risk of suicidal ideation. Physician burnout and poor mental quality of life has been correlated with increased self-assessment of medical errors, lowered patient compliance, and lowered patient satisfaction with their care. For healthcare systems, physician burnout can lead to lowered productivity and efficiency with workplaces that struggle with recruitment and retention issues, increased job turnover, increased early retirements, increased stress leaves, resignations, and reduced work hours.
“Physician health experts are sounding the alarm of a potential fourth wave of COVID-19 amongst healthcare providers: psychological trauma, mental illness, and burnout”
Can a pandemic be a traumatic experience? After the SARS outbreak in 2003, both healthcare workers and the general population who had self-quarantined reported symptoms of posttraumatic stress disorder and depression. Physician health experts are sounding the alarm of a potential fourth wave of COVID-19 amongst healthcare providers: psychological trauma, mental illness, and burnout.
COVID-19 has emphasised the importance of physician health and wellness. Consider the following tips to stay well and prevent burnout during a pandemic:
- Meet your basic needs and make sure you’re eating healthy, drinking fluids, sleeping and resting regularly. Avoid negative coping strategies such as excessive intake of caffeine, sugar, alcohol or drugs.
- Do one thing every day for your mind, one thing for your body, and one thing for your soul.
- Stay connected through regular check-ins with your family and friends.
- Stay updated on what’s happening with COVID-19 but limit your media exposure to just a few trusted sources of information.
- Check in with yourself regularly: monitor yourself over time for any symptoms of depression or distress and seek support if it becomes overwhelming.
- Gauge where your mood is using the self-assessment tool in Figure 1.
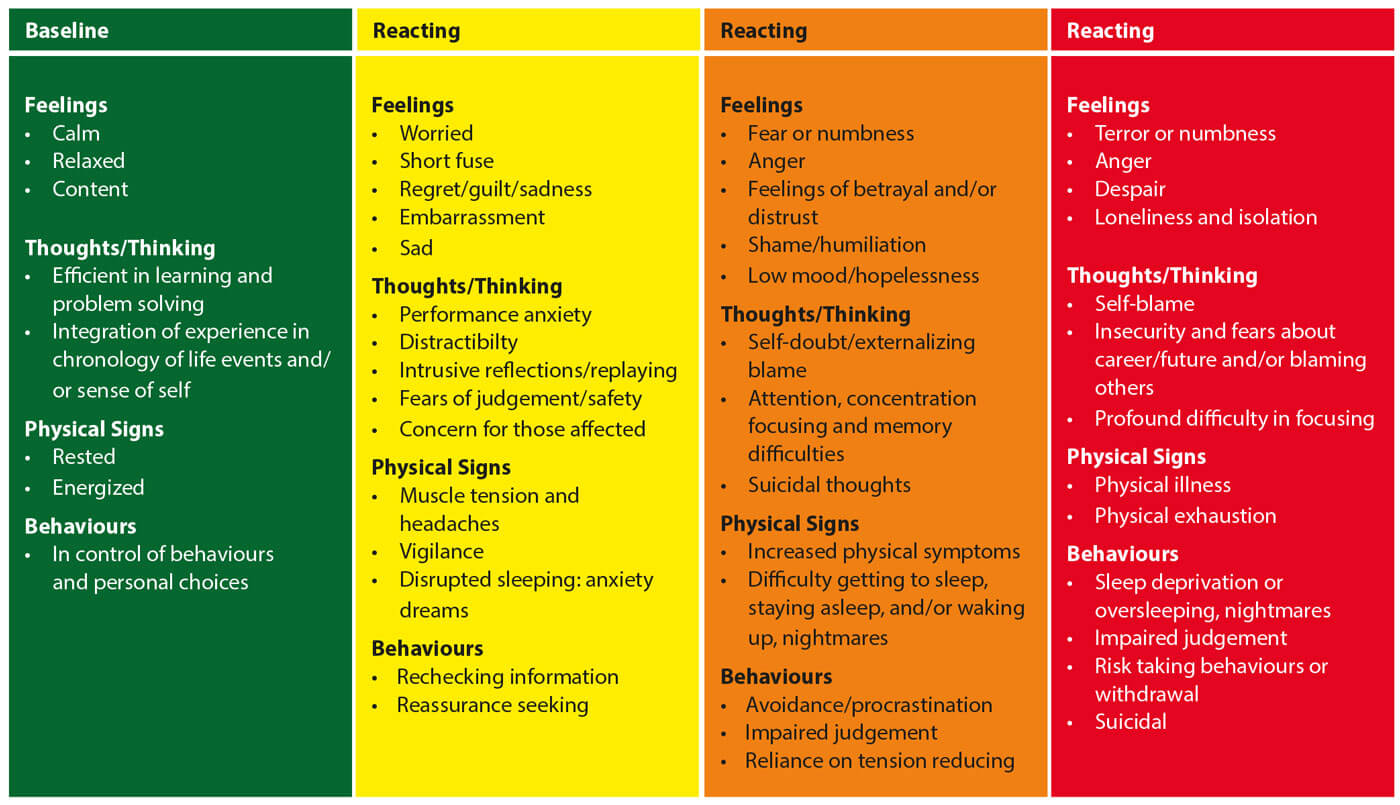
Figure 1. Graphic adapted from Road to Mental Readiness, Canadian Armed Forces
© October 2017 Drs Kerri Ritchie & Caroline Gérin-Lajoie, The Ottawa Hospital.
After checking in, ask yourself what you can do to keep your spirits up, recharge or move towards the green colour. Listen to your feelings and learn to recognise your signs of distress when they appear.
“If the COVID-19 pandemic were to have any silver linings, could it be to shine a more public light on the importance of physician health and wellness?”
Peer support is another important wellness strategy during times of crises. Before checking in with colleagues, ask yourself:
- Am I listening, communicating, and connecting with all my colleagues?
- Am I a courageous leader and colleague or am I succumbing to my own fears and projecting them onto others?
- Am I inspiring others and providing a context for them to exercise courage?
Sir Winston Churchill is credited with saying, “Never let a good crisis go to waste”. Once the initial wave of COVID-19 subsides, an early stability sets in with an opportunity for our brains to reset to the new crisis conditions. This early stability phase is an opportunity for a transformation and change; an opportunity to think differently about our physical and mental health. If the COVID-19 pandemic were to have any silver linings, could it be to shine a more public light on the importance of physician health and wellness?
Join the discussion and we’ll see you in Vancouver, Canada. Find more information at www.ifos2021vancouver.com and follow us on Twitter @IFOSVancouver.




