Technology and innovation has provided modern head and neck surgeons with successive generations of robotic surgical systems, fibre-optic lasers, and novel tools which have ushered in a new era of minimally invasive surgery for tumours of the pharynx and larynx. Chris Holsinger gives us an overview, while clinical trials are underway to define the precise role of these technologies at the present time.
Over the past decade, transoral ‘endoscopic’ head and neck surgery (eHNS) has evolved from the fringes to the frontline of multidisciplinary treatment for head and neck cancer (HNC) [1]. In the past, the role of frontline surgery for patients with oropharyngeal cancers was limited, due to the morbidity of transmandibuar and transfacial approaches. The few indications for transoral minimally invasive surgery and conservation laryngopharyngeal surgery relegated the surgeon, by-and-large, to the task of salvage therapy and heroic radical resections.
Transoral eHNS brings a fresh approach, utilising access to the pharynx through the natural orifice of the mouth. Surgeons can now use a variety of new technologies to resect early stage cancers using an ‘inside-out’ approach: innovative fibreoptic lasers, flexible laparoendoscopic systems (Medrobotics “Flex” System, Medrobotics, Raynham, MA, USA), and a fully robotic surgical system (da Vinci® Surgical System, Intuitive Surgical Inc, Sunnyvale, CA, USA). Regardless of the proprietary technology used, a subspecialty within head and neck surgery had emerged as transoral eHNS. Independent of technology, these approaches use a common route of access and surgical incisions made entirely within the mouth, eliminating any external deformity. Attention to haemostasis and careful objective management of surgical margins – time-honoured principles of surgical oncology, though – are maintained.
Among the techniques used in transoral eHNS, transoral robotic surgery (TORS) has seen rapid and widespread adoption over the past decade. In 2009, the United States Food and Drug Administration approved the use of the da Vinci® Surgical System for ‘transoral otolaryngology’ procedures. During TORS, the surgeon remotely controls robotic instruments and a stereo-endoscope that can be docked within the mouth, providing a three-dimensional view of the surgical field and the ability to perform two-handed surgery in the confined space of the oral cavity and pharynx. Thus, real surgery is performed using a simulated ‘virtual’ environment in a specially designed console, affording the surgeon with enhanced visualisation of the target surgical anatomy and two instruments capable of dexterity (540° of rotation) that exceeds the mechanics of the human.
For the first time, the instruments used by the surgeon have no physical connection to the surgeon’s hand. Despite this virtual and remote telepresence control, every move of each surgical instrument arm and the camera is directly controlled by the surgeon using a ‘master-slave’ robotic configuration.
The first case reports of robotic surgery for an oropharyngeal tumour were published in 2005 and, since then, a rich retrospective literature has emerged supporting the role of TORS. Early reports demonstrated good rates of local control and good disease-specific survival [2], independent of p16 status [3]. A large multicentre study of transoral robotic head and neck surgery was recently published, demonstrating two-year locoregional control rate of 91.8% and overall survival of 91.0% in 410 patients treated in 11 centres across the world. Ninety percent of patients had tumours arising within the oropharynx; 84% of these were T1-2 tumours. This large experience may demonstrate the safety, feasibility and efficacy of robotic surgery for patients with HNC.
In general, after robotic head and neck surgery, patients return to normal speech and swallowing function in the immediate postoperative period, usually within two to three weeks. Surgical wounds heal by secondary intention and flap reconstruction is rarely needed for properly selected cases.
Some sceptics, however, remain wary of this approach, citing concerns about “close” surgical margins compared to standard open technique, as well as the high rate of radiation therapy required postoperatively. Two studies (from the University of Pennsylvania and the University of Pittsburgh) demonstrated high rates of local control (> 90%), for carefully selected patients who only received TORS and neck dissection – and no postoperative radiation therapy. Nonetheless, the multidisciplinary head and neck oncologic community is eager for prospective clinical trial data to better understand the role of this new approach.
In October 2013, the Eastern Cooperative Oncology Group (ECOG) launched a phase II clinical trial, E3311. The underlying hypothesis of the study is that transoral eHNS (including TORS) can facilitate de-intensified (reduced dose) postoperative radiation therapy (RT) and maintain loco-regional disease control, while improving swallowing function. The primary objective is to evaluate progression-free survival in “intermediate-risk” patients, comparing two postoperative RT doses: 50 Gy versus a standard dose of 60 Gy. Final pathologic staging defines those patients with intermediate risk as those with close margins (<3mm), the presence of 2-4 metastatic lymph nodes or extracapsular extension (ECE) of tumour outside any of these nodes of <1 mm. These intermediate-risk patients are randomised to receive either a standard postoperative dose of 60 Gray or 50 Gray in the study arm.
An estimated 377 patients are required to complete the study of two years. Seventy-one surgeons from more than 40 centres in North America are credentialed and accruing patients on this trial. TORS has relied on rigid instruments and technology primarily designed for abdominopelvic and thoracic surgery. Although this first-generation platform has facilitated significant improvements in the practice of transoral eHNS, the scale and design of this system is not ideally suited to the oral cavity and pharynx. Recently, a new flexible and fully robotic surgical system (DaVinci Sp, Intuitive Surgical, Inc) has been described [5].
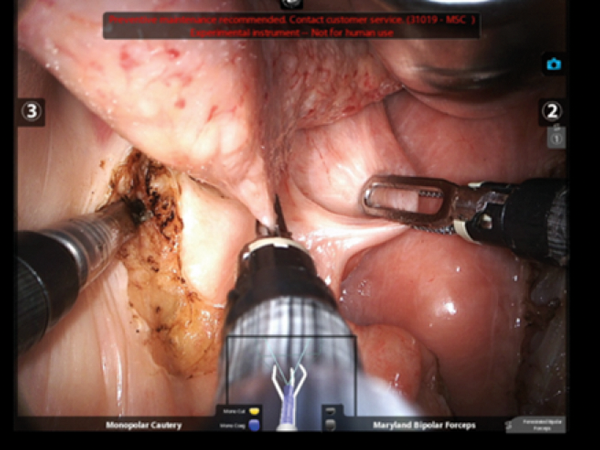
This flexible robotic surgical system is deployed through a single arm and cannula, with a flexible camera and three instrument arms. In human cadaver studies, this smaller system routinely allowed four arms to be used simultaneously during transoral surgery of the oropharynx. As a result, this next-generation robotic surgical system allows three-handed surgery within the oropharynx, improving traction-countertraction and thus revealing a more accurate understanding of the complex three-dimensional relationships of the lateral oropharyngeal wall (Figure 1).
Figure 1: Three instruments from da Vinci SP Surgical System (Model SP999; Intuitive Surgical Inc, Sunnyvale, CA, USA) are shown here exposing the collapsed folds of the lateral oropharyngeal wall.
Conclusion
Robotic head and neck surgery has been widely adopted over the past decade. This transoral minimally invasive approach permits oncologic margins similar to open surgery, while minimising morbidity and deformity. The impact of TORS on the dose and schedule of postoperative radiation therapy is currently being evaluated in prospective national clinical trial ECOG3311. Using this first-generation technology, TORS has permitted surgeons to provide refined pathologic staging while minimising change in speech or swallowing. New flexible systems may be available soon for clinical use to expand the reach and further refine the technique and outcomes of robotic head and neck surgery.
References
1. Holsinger FC, Ferris RL. Transoral Endoscopic Head and Neck Surgery and Its Role within the Multidisciplinary Treatment Paradigm of Oropharynx Cancer: Robotics, Lasers, and Future Innovations. J Clin Oncol 2015;10;33(29):3285-92.
2. White HN, Moore EJ, Rosenthal EL, et al. Transoral robotic-assisted surgery for head and neck squamous cell carcinoma: one- and two-year survival analysis. Arch Otolaryngol Head Neck Surg 2010;136(12):1248-52.
3. Cohen MA, Weinstein GS, O’Malley BW, et al. Transoral robotic surgery and human papillomavirus status: Oncologic results. Head Neck 2011;33(4):573-80.
4. de Almeida JR, Li RJ, Magnuson JS, et al. Oncologic Outcomes following Transoral Robotic Surgery (TORS): A Multi-institutional Study. JAMA Otolaryngol Head Neck Surg 2015;141(12):E1-E9.
5. Holsinger FC. A Flexible, Single-Arm, Robotic Surgical System for Transoral Resection of the Tonsil, Lateral Pharyngeal Wall: Next-Generation Robotic Head and Neck Surgery. Laryngoscope 2015; [Epub ahead of print] doi:10.1002 lary.25724.
Declaration of Competing Interests: None declared.
ABOUT THE AUTHOR
Dr Holsinger is Chief of Head and Neck Surgery and leads the multidisciplinary Head and Neck Oncology programme at Stanford University. Dr Holsinger has led several efforts to transform cancer care delivery within the Cancer Center, most recently focussing on standardising and improving the quality of multidisciplinary tumour boards. At Stanford, he also founded the programme in Robotic Surgery, which coordinates clinical operations, as well as provides continuing educational opportunities for residents, fellows and staff in the surgical subspecialties. This multidisciplinary programme is also studying the value and cost of robotic surgery across several organ sites, measuring the impact of reduced length of stay and postoperative dose reduction of adjuvant therapies. Dr Holsinger’s surgical practice focusses on the surgical management of benign and malignant diseases of the thyroid, as well as head and neck cancers. Nationally, he has led the efforts to promote prospective clinical trials and innovation in head and neck surgery, especially robotics.
SUMMARY
-
Robotic surgery plays an important role in the multidisciplinary management of oropharyngeal cancer, but with the current technology may have only limited use for the larynx and hypopharynx.
-
Patients ideally suited for transoral robotic surgery are patients with early T-stage tumours with no or low-volume neck metastases: T1-2, N0-N2b, M0.
-
Prospective ongoing clinical trials, such as ECOG 3311, will further refine optimal eligibility criteria for which HNC patients benefit from frontline treatment with robotic head and neck surgery.
-
Next-generation, flexible robotic systems may be introduced into pre-clinical testing and thus provide a surgical platform better suited to perform robotic head and neck surgery.