Introduction
Since its advent in 1964 when Dotter percutaneously dilated a stenosed femoral artery [1], interventional radiology has undergone tremendous advancement in both imaging and devices that have enabled the operator (interventional radiologist) to access very distal small vasculature and perform procedures that were hitherto not possible.
The role of an interventional neuroradiologist in otorhinolaryngology is not only in therapeutic neurointerventional procedures such as in reducing intraoperative blood loss, as by preoperative embolisation of head and neck tumours, preventing active bleeding, as in controlling intractable epistaxis, carotid occlusion in threatened or imminent ‘carotid blowout’, but also in certain diagnostic procedures.
Tumour embolisation
The main aim of tumour embolisation is ‘preoperative devascularisation’ of tumour prior to surgery. In some patients who are unfit for an anaesthetic, it may also be used as a palliative procedure.
Preoperative embolisation is most commonly used in the management of juvenile nasal angiofibroma (JNA) which is an uncommon benign tumour of adolescent males with a very rich blood supply. This lesion arises in the pterygo-palatine fossa and then expands aggressively into the nasopharynx and nasal cavity through the sphenopalatine foramen.
Embolisation is very effective in minimising intraoperative blood loss and is now a well-accepted part of the treatment of JNA [2]. (Figure 1 shows a case of preoperative embolisation of a juvenile angiofibroma).
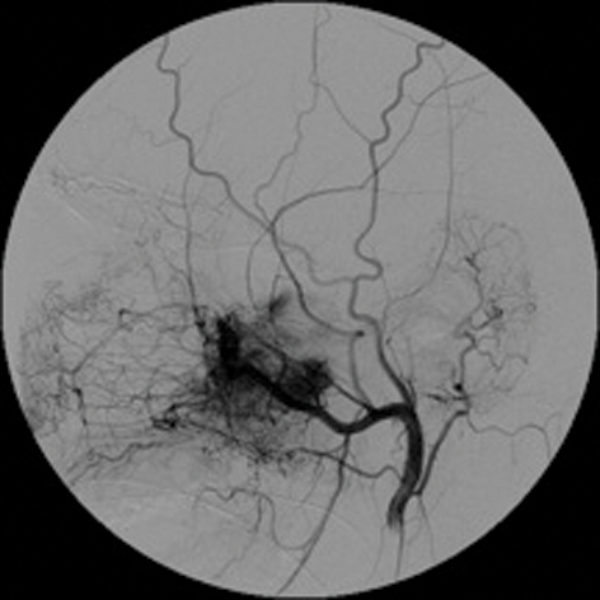
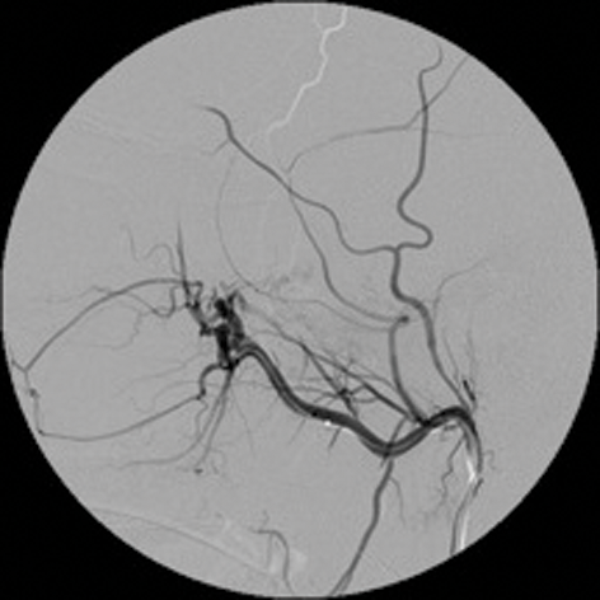
Figure 1: Juvenile angiofibroma before and after embolisation.
Embolisation is also effective in paragangliomas (glomus tympanicum, glomus jugulare and carotid body tumours). These are tumours arising from paraganglionic chemoreceptor cells which receive their blood supply from the ascending pharyngeal artery. They can be multicentric, locally invasive with malignant potential. Preoperative embolisation of paragangliomas greatly facilitates surgery and reduces the operative time and reduces the associated morbidity [3, 4]. (Figure 2 shows a case of preoperative embolisation of a glomus vagale tumour).
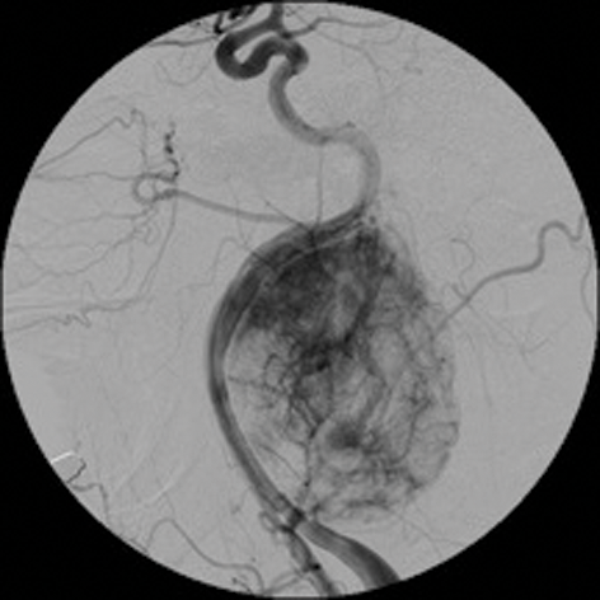
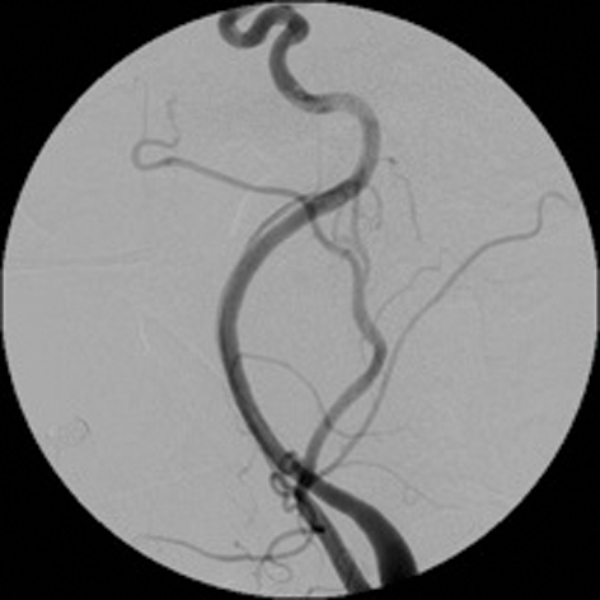
Figure 2: Glomus vagale before and after embolisation.
Arterio-venous fistulas
Arterio-venous (AV) fistulae are abnormal connections between arteries and veins which can be congenital, spontaneous or traumatic. Treatment of AV fistulae of head and neck also falls within the remit of interventional neuroradiology. These lesions are often difficult to treat surgically because of multiplicity of feeders and difficulty in access etc.
Endovascular treatment of AV fistulas involves preservation of the normal vasculature and occluding both the distal and proximal vessels of the fistula.
Detachable balloons, particles and / or sclerosants, and stents are used in the endovascular treatment of these lesions. (Figure 3 shows a case of a traumatic external carotid-jugular AV fistula treated by coil embolisation).
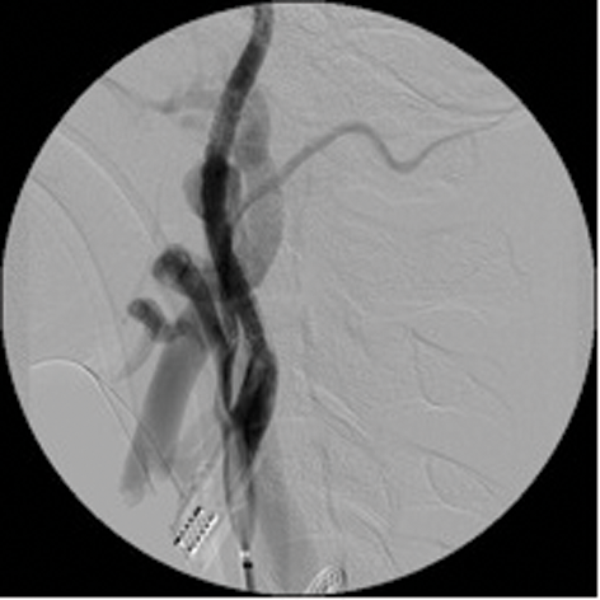
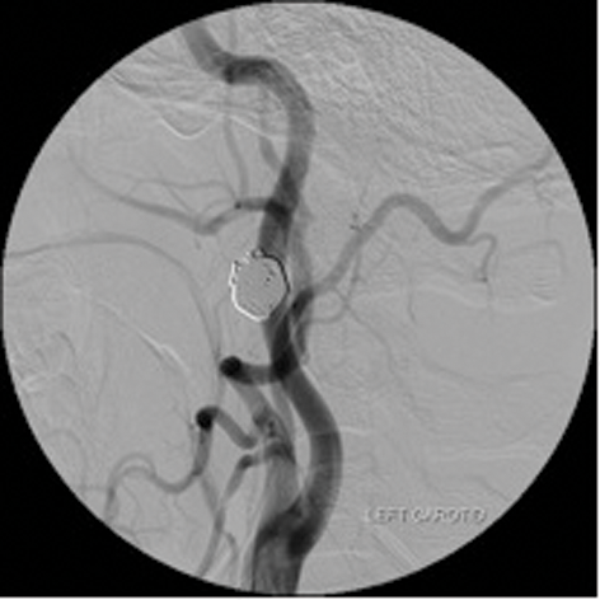
Figure 3: ECA- jugular fistula before and after embolisation.
Epistaxis
Most cases of epistaxis are from an anterior nasal artery and are treated with simple procedures viz. cautery and nasal packing. However, interventional neuroradiology plays an important role in cases of intractable posterior epistaxis after failure of conventional treatment (posterior nasal packing). Super-selective embolisation of the bleeding artery with particles / coils is an effective treatment in such cases with a low complication rate [5-10].
Surgical procedures such as ligation of the anterior ethmoidal artery, sphenopalatine artery or internal maxillary artery may be performed in such cases. However, the minimally invasive nature of the endovascular technique makes it an attractive option. Also if for some reason the endovascular treatment is not effective there is always the surgical option available.
On the other hand once the internal maxillary or sphenopalatine artery is surgically ligated there is no safe access available to the interventional neuroradiologist. For this reason, in our centre, cases of intractable posterior epistaxis are first treated by the interventional neuroradiologist, with the ENT surgeon performing microsurgical ligation only if the endovascular technique is in effective.
Embolisation in cases of epistaxis involves injection of polyvinyl alcohol (PVA) particles (150-350 microns), gel foam pledgets and at times coil embolisation after selective catheterisation of the internal maxillary artery (IMA).
Carotid blowout
Carotid blowout (both threatened and imminent) is a well-recognised, dreaded complication of advanced head and neck cancer, which occurs in up to 3-4% of patients following radical neck dissection [11]. Surgical ligation in such patients is technically difficult (due to ongoing infection, post-surgical / radiotherapy fibrosis) and it is often impossible to identify the exact source of bleeding. Surgery in carotid blowout carries approximately a 40% risk of mortality and 60% incidence of neurological complications [12, 13]. Traditionally such patients have been managed conservatively on an end of life pathway.
Endovascular treatment is now the gold standard for this condition. Three techniques can be employed by interventional neuroradiologists to treat ‘carotid blowout’. The first involves permanent balloon occlusion (PBO) of the carotid artery with a detachable balloon thus preventing blood flow into the bleeding vessel [12]. Prior to performing permanent balloon occlusion a ‘temporary balloon occlusion’ is performed with a non-detachable balloon in order to identify the patients at risk of cerebral ischaemia secondary to parent vessel occlusion. Such patients can also be treated by selective occlusion of the bleeding vessels, leaving the main carotid artery patent [14]. The third option involves placement of a ‘covered’ carotid stent [15-18], across the site of vessel blowout.
Despite successful treatment such patients can present with re-haemorrhage or with delayed stent thrombosis / stenosis [16, 17]. Hence all patients with threatened or imminent carotid blowout should be discussed in a multidisciplinary meeting to identify those patients in whom intervention would be beneficial.
Future perspective
Intense research is ongoing in endovascular treatment of malignant diseases with several promising developments in endovascular therapy which include catheter directed superselective intra-arterialchemotherapy, microcatheter directed gene therapy and tumour radiofrequency ablation [19].
With the continual ongoing improvement in imaging technology, microcatheter design and expansion in the interventional neuroradiological workforce it is anticipated that there will be a continuous expansion of the indications for using interventional radiological treatment [20]. In the future it may be possible to perform many of these procedures on an outpatient basis [21], which will require increasing collaboration between specialities in order to safely and effectively deliver these services.
References
1. Rösch J, Keller FS, Kaufman JA. The birth, early years, and future of interventional radiology. J Vasc Interv Radiol 2003;14:841-53.
2. Siniluoto TM, Luotonen JP, Tikkakoski TA, et al. Value of pre-operative embolization in surgery for nasopharyngeal angiofibroma. J Laryngol Otol 1993;107:514-21.
3. Valvanis A, Christoforidis G. Applications of interventional neuroradiology in the head and neck. Semin Roentgenol 2000;35:72-83.
4. Horowitz M, Whisnant RE, Jungreis C, et al. Temporary balloon occlusion and ethanol injection for preoperative embolisation of carotid-body tumour. Ear Nose Throat J 2002;81:536-8, 540, 542 passim.
5. Moreau S, De Rugy MG, Babin E, et al. Supraselective embolization in intractable epistaxis: review of 45 cases. Laryngoscope 1998;108:887-8.
6. Elden L, Montanera W, Terbrugge K, et al. Angiographic embolization for the treatment of epistaxis: a review of 108 cases. Otolaryngol Head Neck Surg 1994;111:44-50.
7. Siniluoto TM1, Leinonen AS, Karttunen AI, et al. Embolization for posterior epistaxis. An analysis of 31 cases. Arch Otolaryngol Head Neck Surg 1993;119:837-41.
8. Scaramuzzi N, Walsh RM, Brennan P, Walsh M. Treatment of intractable epistaxis using arterial embolization. Clin Otolaryngol Allied Sci 2001;26:307-9.
9. Gurney TA, Dowd CF, Murr AH. Embolization for the treatment of idiopathic posterior epistaxis. Am J Rhinol 2004;18:335-9.
10. Oguni T, Korogi Y, Yasunaga T, et al. Superselective embolisation for intractable idiopathic epistaxis. Br J Radiol 2000;73:1148-53.
11. Cohen J, Rad I. Contemporary management of carotid blowout. Curr Opin Otolaryngol Head Neck Surg 2004;12:110-5.
12. Citardi MJ, Chaloupka JC, Son YH, et al. Management of carotid artery rupture by monitored endovascular therapeutic occlusion (1988–1994). Laryngoscope 1995;105:1086-92.
13. Chaloupka JC, Putman CM, Citardi MJ, et al. Endovascular therapy for the carotid blowout syndrome in head and neck surgical patients: diagnostic and managerial considerations. AJNR Am J Neuroradiol 1996;17:843-52.
14. Morrissey DD, Andersen PE, Nesbit GM, et al. Endovascular management of hemorrhage in patients with head and neck cancer. Arch Otolaryngol Head Neck Surg 1997;123:15-9.
15. Bates MC, Shawsham FM. Endovascular management of impending carotid rupture in a patient with advanced head and neck cancer. J Endovasc Ther 2003;10:54-7.
16. Lesley WS, Chaloupka JC, Weigele JB, et al. Preliminary experience with endovascular reconstruction for the management of carotid blowout syndrome. AJNR Am J Neuroradiol 2003;24:975-81.
17. Broomfield SJ, Bruce IA, Luff DA, et al. Endovascular management of the carotid blowout syndrome. J Laryngol Otol 2006;120:694-7.
18. Pride GL Jr, Horowitz MB, Purdy PD. Endovascular problem solving with intravascular stents. AJNR Am J Neuroradiol 2000;21:532-40.
19. Montgomery ML, Sullivan JP. Advances in interventional radiology. The search for less invasive management sparks new approaches. Postgraduate Med 2001;109:93.
20. Bakal CW. Advances in imaging technology and the growth of vascular and interventional radiology: a brief history. J Vasc Interv Radiol 2003;14:855-60.
21. Young N, Chi KK, Ajaka J, et al. Complications with outpatient angiography and interventional procedures. Cardiovasc Intervent Radiol 2002;25:123-6.
Declaration of Competing Interests: None declared.




