Tympanic membrane perforations are a common finding in ENT practice. Whilst watchful waiting or formal tympanoplasty are standard options – wouldn’t it be amazing if there was a low cost, safe, in-clinic option to immediately help patients (I hear you cry)? Alok Rathi is one step ahead of you, detailing the potential in-clinic options that might be available to us in the not too distant future.
Tympanic membrane perforation is one of the most common aetiologies for reversible hearing loss and recurrent infections. Tympanoplasty, a surgical procedure to close perforations, is simple and involves freshening margins of perforation and patching the hole with a thin membrane (acting as scaffold). The graft can be harvested from patient’s own body (temporalis fascia/ tragal perichondrium) or be synthetic in nature.
In last few decades, various attempts have been made towards performing this procedure in clinic, which, if successful, will decrease time and cost and, if sufficiently simple, potentially morbidity. This may lead to increased performance and quality of life. American SEER fund has invited applications for innovative tympanic membrane repair material which can be used in war settings. Such materials and techniques could be a boost to paediatric age group reversible hearing loss as they often have morbidity related to hearing and speech.

Figure 1.
Access and visualisation
Otoendoscopy and endoscopic ear surgery has evolved in the last two decades and today many surgeons are familiar with its nuances and dexterity. At present, both microscope and otoendoscope are well-established for office-based procedures. A new device which is claimed to have better visualisation for ear surgeries is in the pipeline from Tympany® (see Figure 1), though further details are not available as it is being patented at present. The lead innovator, an anaesthesia trainee and Bioinnovate® alumnus, mentions it to be best possible way to perform ear surgeries [tympanymedical.com]. Their device appears to be an innovative speculum with circumferential optical fibres at the medial end analogous to chip-tip camera.

Figure 2.
De-epithelisation of margins
Outside conventional excision of the perforation edge, chemical cautery/peel has been the only successful method for this step. Both trichloroacetic acid and silver nitrate have been used successfully. A device developed by Tymcure® (see Figure 2) with an inbuilt special circular knife offers the potential to simplify this step [tymcure.com]. A detailed description of Tymcure® is given later in this article.
“Their device appears to be an innovative speculum with circumferential optical fibres at the medial end analogous to chip-tip camera”
Repair material
Autologous graft harvest may be obsolete in near future. Today we have artificial membrane (e.g. Biodesign®), which has replaced the autologous membrane harvest in many centres. Other options successfully used include platelet rich plasma enriched gelfoam, silk patch, and chitosan patch [1]. Fibroblast growth factor has been used to stimulate growth and close the perforation. Bioprinted ear grafts have been made using chinchilla models. Tymcure® has two layers of bioabsorbable graft which snugly closes the perforation on both sides of drum.
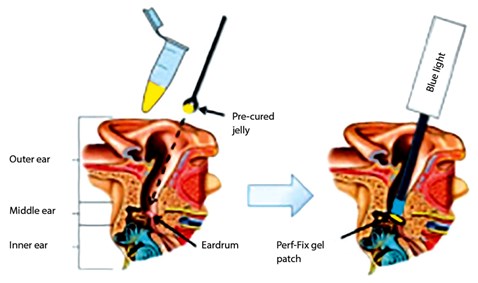
Figure 3.
Non-surgical repair
Perf-Fix (see Figure 3)
A new innovative biomaterial is in prototype stage which pledges to heal perforation without surgery. It is a light gel patch which acts as scaffold and allows membrane to grow across the perforation. This growing epithelial layer will absorb the gel patch. It is expected not to dislodge from the perforation with the vibration of drum due to its inherent pliability. Tympanogen, Inc.® claims it can be applied in an in-office setting in 10 minutes and does not require freshening of margins [tympanogen.com].
Tympanic membrane patcher
This device was developed quite a while ago and, in simple terms, it is a grommet without hole. It helps in immediate seal of the perforation by patcher and helps in gradual healing [2].
Tymcure®
It is an innovative tool, which has a circular operating knife attached to the handle and two biomaterial grafts on either side of the knife. Following topical anaesthesia, a medial biomaterial graft is inserted beyond perforation into middle ear. Then, the circular knife is used to freshen the margin by rotational movement of the handle and finally, a lateral layer of graft is pushed to bring both layers together. They are released by a switch of the handle which keeps the layers intact with the help of tie.
References:
1. Santa Maria PL, Oghalai JS. Is Office-Based Myringoplasty a Suitable Alternative to Surgical Tympanoplasty?
www.sbccp.org.br/
arquivos/LG2014-05/lary24221.pdf
Last accessed October 2019.
2. Kartush JM. Tympanic membrane Patcher: a new device to close tympanic membrane perforations in an office setting. Am J Otol 2000;21(5):615-20.
Declaration of Competing Interests: None declared.





