Tinnitus is the perception of sound without an external source. The estimated prevalence in adults is between 10-15% [1]. In patients with significant tinnitus, prompting them to seek medical attention, 50% will have improved to mild or no tinnitus by five years. Around 20% of patients with tinnitus will require clinical intervention [2].
The trigger for tinnitus in the vast majority is hearing loss and emotional stress. The commonest causes of such hearing loss are presbycusis and noise induced hearing loss, although any cause of conductive or sensorineural hearing loss can trigger tinnitus. It is also important to appreciate that patients with normal audiometric thresholds will have some degree of degenerative cochlea damage and exhibit reduced auditory input to the central nervous system [3, 4]. This peripheral damage is thought to result in central neural plastic changes that influence the balance between excitatory and inhibitory processes leading to a promotion of increased neurological activity, particularly with the primary auditory cortices and the subsequent emergence of the tinnitus perception [5].
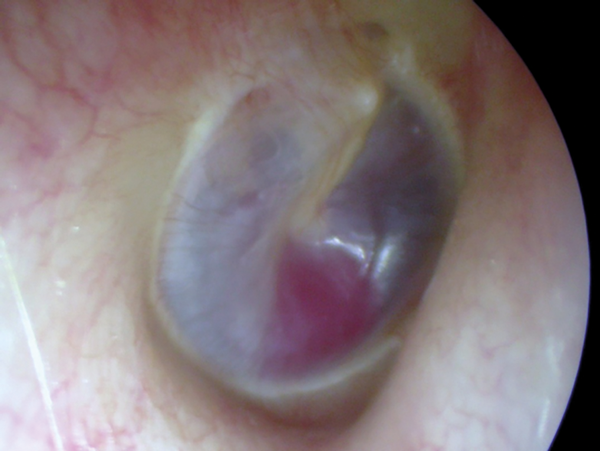
Figure 1: Glomus tympanicum in right middle ear seen with otoendoscopy.
Clinical assessment
Effective management of tinnitus requires an accurate diagnosis as treatment options vary. This is facilitated through a careful history, examination and special investigations. During assessment the following five factors should be determined as they help guide management [1]:
- Primary or secondary. Primary tinnitus is idiopathic and may or may not be associated with sensorineural hearing loss (SNHL). Secondary tinnitus is associated with a specific underlying cause other than SNHL e.g. acoustic neuroma, glomus tumour (Figure 1) or vascular anomaly, otosclerosis, chronic otitis media.
- Recent onset or persistent. Tinnitus less than six months in duration is recent onset. Persistent tinnitus has been present over six months.
- Bothersome or non-bothersome. Tinnitus is bothersome when it causes distress, affects quality of life and patient seeks active management to alleviate it.
- Subjective or objective. In the vast majority tinnitus is subjective and only perceived by the patient. Rarely it is objective and can be perceived by others e.g. clicking sounds associated with palatal or middle ear myoclonus.
- Pulsatile or non-pulsatile. Pulsatile tinnitus is perceived by the patient as a pulsation in the ear or head which may or may not be in rhythm with their heartbeat. Sometimes it can be heard by the examiner with a stethoscope.
“Effective management of tinnitus requires an accurate diagnosis as treatment options vary.”
A thorough history should include the cardinal otological symptoms (hearing loss, tinnitus, ear pain, ear discharge and vertigo), as well as enquiry about specific risk factors for tinnitus such as age, loud noise exposure, ototoxic drugs, previous ear disease, family history of deafness, excessive alcohol / caffeine intake, anxiety / depression, cognitive impairment, diabetes, hypertension, rheumatoid arthritis and temporomandibular joint symptoms.
All patients should be examined with otoscopy and have a cranial nerve assessment. In the presence of localising signs or other neurological / balance symptoms patients should have their balance formally assessed. In patients with objective and / or pulsatile tinnitus examination should include auscultation of the heart, head and neck as well as examination of the palate and orbits (including fundoscopy to look for papilloedema, e.g. idiopathic intracranial hypertension). If cognitive impairment is suspected the clock-drawing test can be used as a cognitive screening instrument.
The Tinnitus Handicap Inventory (THI) [6] is a useful validated tool to assess tinnitus severity and monitor response to any treatment [7]. Patients with scores suggesting severe to catastrophic tinnitus may benefit from further assessment of depression severity (PHQ-9 Depression scale) and anxiety disorder (GAD-7 Anxiety scale) as an urgent referral to the acute mental health team may be warranted.
All patients with tinnitus which is persistent, unilateral or associated with hearing loss should undergo audiometry and tympanometry to determine severity and type of hearing loss, asymmetry, need for imaging and to guide treatment. Depending on the history, blood investigations may be warranted including full blood count, fasting glucose and lipids, thyroid function test and autoimmune profile.
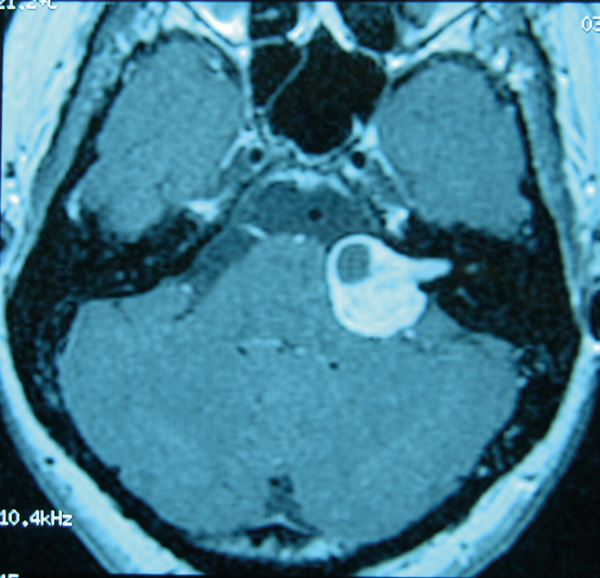
Figure 2: Gadolinium enhanced MRI scan showing a left vestibular schwannoma.
Imaging studies are not indicated unless tinnitus is unilateral, pulsatile, or there is asymmetric hearing loss or focal neurological abnormalities. Patients who report experiencing unilateral subjective tinnitus with or without hearing loss should undergo gadolinium enhanced MRI in order to exclude any cochlear or retrocochlear abnormality (Figure 2). Patients with pulsatile tinnitus should undergo CT angiography.
Treatment
For secondary tinnitus, treatment depends on the causal condition, e.g. surgical removal for a glomus tympanicum.
For early onset primary tinnitus or non-bothersome primary persistent tinnitus, reassurance and advice may be all that is required.
For bothersome primary persistent tinnitus, the goal of treatment is to induce the patient to habituate to the tinnitus signal so that it no longer evokes a negative emotional reaction [8, 9]. The espoused mode of action differs between techniques but most interventions strive to in some way normalise central plastic changes that have been induced by hearing loss and are implicit in the generation / perception of the tinnitus signal. Treatment should be multidisciplinary and patient focused, utilising a range of options which include relaxation techniques, provision of a hearing aid, sound therapy, and cognitive behavioural therapy. There is good research evidence supporting the effectiveness of cognitive behavioural therapy in reducing tinnitus related distress [10, 11].
Recent advances in tinnitus management include neuromodulation which aims to influence central neural activity in order to reduce pathological processes. Examples of such therapies include transcranial magnetic stimulation (TMS) and Acoustic Coordinated Reset® which strive to reduce neural excitability / synchrony within the central auditory system [12].
References
1. Tunkel TE, Bauer CA, Sun, GH, et al. Clinical Practice Guideline: Tinnitus. Otolaryngol Head Neck Surg 2014;151(S2): S1-S40.
2. Cooper JC. Health and Nutrition Examination Survey of 1971–75: Part II. Tinnitus, subjective hearing loss, and well-being. J Am Acad Audiol 1994;5(1):37-43.
3. Job A, Raynal M, Kossowski M. Susceptibility to tinnitus revealed at 2 kHz range by bilateral lower DPOAEs in normal hearing subjects with noise exposure. Audiol Neurootol 2007;12:137-144.
4. Weisz N, Hartmann T, Dohrmann K, et al. High-frequency tinnitus without hearing loss does not mean absence of deafferentation. Hear Res 2006;222(1-2):108-14.
5. Eggermont JJ,, Roberts LE. Tinnitus: animal models and findings in humans. Cell Tissue Res 2015;361(1):311-36.
6. Newman CW, Jacobson GP, Spitzer JB. Development of the Tinnitus Handicap Inventory. Arch Otolaryngol Head Neck Surg 1996;122:143-8.
7. McCombe A, Baguely D, Coles R, et al. Guidelines for the grading of tinnitus severity: the results a working group commissioned by the British Association of Otolaryngologists, Head and Neck Surgeons, 999. Clin Otolarynogol 2001;26:388-93.
8. Jastreboff PJ. Tinnitus. In: Gates GA, ed. Current Therapy in Otolaryngology: Head and Neck Surgery. 6th ed. St. Louis, USA; Mosby; 1998: 90-5.
9. Jastreboff PJ, Hazell JWP. A neurophysiological approach to tinnitus: clinical implications. Br J Audiol 1993; 27:7–17.
10. Cima RFF, Maes IH, Joore MA, et al. Specialised treatment based on cognitive behaviour therapy versus usual care for tinnitus: a randomised controlled trial. Lancet 2012;379:1951-9.
11. Martinez-Devesa P, Perera R, Theodoulou M, Waddell A. Cognitive behavioural therapy for tinnitus. Cochrane Database Syst Rev 2010;9.
12. Tass P, Adamchic L, Freund H, et al. Counteracting tinnitus by acoustic coordinated reset Neuromodulation. Restorative Neurology and Neuroscience 2012;30(2):367-74.
Declaration of competing interests: MW acts as a clinical advisor to the manufacturer of the T30 neurostimulator (Neurotherapies Reset GmbH) for the provision of acoustic CR neuromodulation therapy.