Are we ready to deliver remote care? A question many of us have asked ourselves over the last year. Danielle Glista (Associate Professor, Western University) and colleagues talk through a systematic approach to implementing remote audiological care and suggest gaps in our current readiness.
Globally, we are faced with a great need for audiological care to embrace alternative models of service delivery. This relates to an increasing number of people affected by hearing loss, limited availability of professionals, and an ongoing pandemic requiring social distancing measures.
The connected hearing healthcare model of care emerges as a practical alternative solution for the technology-driven field of audiology [1,2]; this encompasses a plethora of related terms including connected audiology, teleaudiology, eAudiology, and remote care (RC), all describing alternative service delivery options with the potential to improve the accessibility, convenience, and efficiency of services for many individuals.
What is readiness?
Readiness is defined as the degree to which the involved stakeholders are individually and collectively primed, motived, and capable of executing the change [3]. Within the field of audiology, readiness is multilevelled and includes clients/patients, families, healthcare professionals, organisations, and a broader healthcare context. It is also multidimensional, requiring a comprehensive look at many different factors. This article focuses on readiness from the perspective of implementing a service delivery change, from the traditional in-person model of care to one that delivers services at a distance. The variation in uptake and sustainability of telehealth services has been reported to relate closely to the acceptance level of the healthcare professional [4], alongside a lack of technology, infrastructure, professional training, reimbursement guidance, licensure laws, evidence to support implementation, standards, and costs [4]. A more comprehensive understanding of the readiness state of audiologists around RC will help our profession determine how best to support clinical implementation to influence system-wide success.
“The variation in uptake and sustainability of telehealth services has been reported to relate closely to the acceptance level of the healthcare professional”
The emerging concept of readiness in healthcare
There is growing literature concerning the use of guiding frameworks to provide a comprehensive conceptualisation of ‘readiness for change’ across different stakeholder levels and regarding new/revised healthcare service implementation efforts [3,6,7]. These readiness frameworks guide the development of tools aimed at evaluating readiness, structuring change, and developing practice [3].
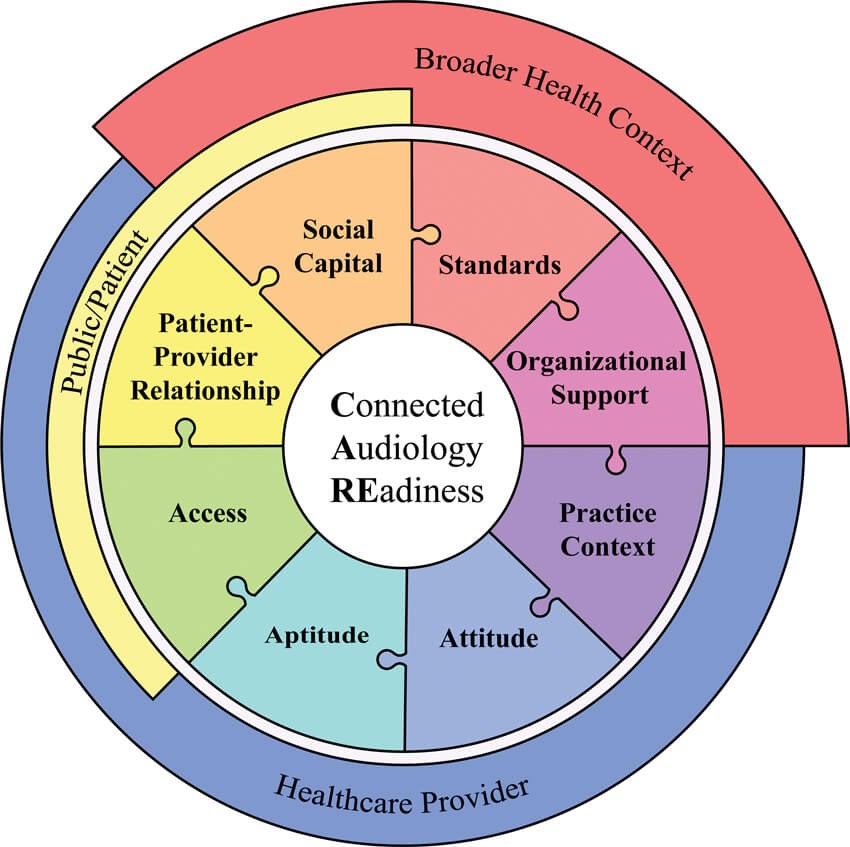
Figure 1. Illustration of the multilevel and multidimensional components
of the Connected Audiology REadiness Framework.
The Connected Audiology REadiness (CARE) Framework (Figure 1), developed at the National Centre for Audiology (NCA), Western University, builds on existing eHealth readiness frameworks, such as the FeRD, while incorporating existing theories on the factors influencing clinician adoption of remote hearing aid support [2] and the characteristics influencing the use of knowledge and evidence in clinical practice [8]. The CARE framework includes eight multidimensional readiness categories [9].
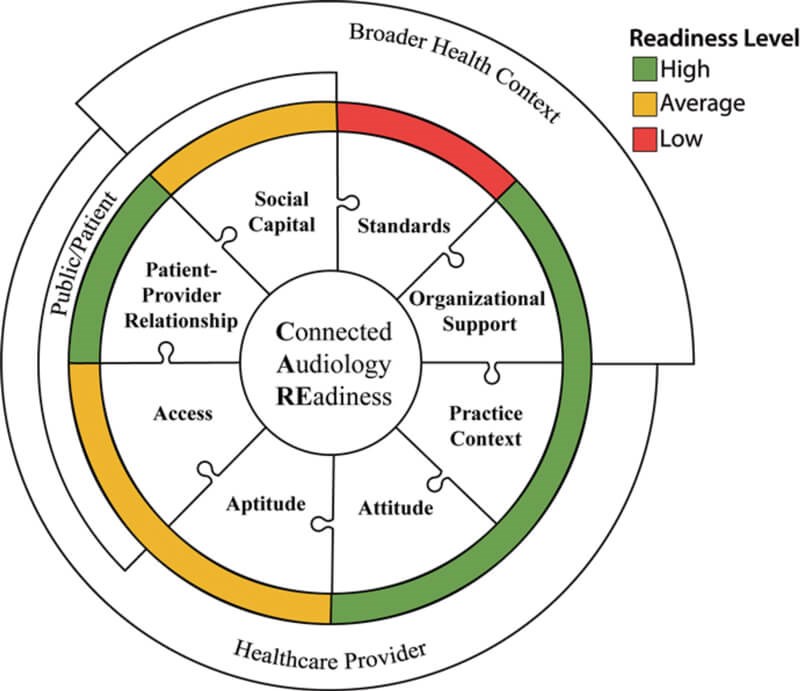
Figure 2. Readiness levels of Canadian audiologists, according to the eight CARE dimensions,
to uptake remote hearing aid support services.
Connected Audiology REadiness in Canada
Recently, the CARE framework has been used in developing a tool to assess audiologists’ readiness to adopt RC: The Connected Audiology Readiness Evaluation. Figure 2 summarises the important findings related to the uptake of RC. Overall, the study results suggest a great need for professional practice guidelines and standards to support implementation, and a moderate need for greater access to technology, infrastructure and professional development opportunities [9,10].
Implementation matters: are you ready?
The CARE tool provides important information regarding factors that influence readiness to uptake RC. Understanding these factors prompts us to consider theories to address barriers to implementation. Through the use of evidence-based methods in the creation of knowledge and processes to make changes in practice behaviour, we can improve the quality, efficiency and effectiveness of remote audiological care [11-15]. According to the CARE results, attention should be given to: (1) standards (protocols, guidelines); and (2) aptitude (knowledge, skills).
“Our implementation activities will include collaboration with end-users to determine behaviour change techniques and materials that best target knowledge, skills and behaviours to facilitate remote care”
Standards readiness
The NCA has adopted the Knowledge-to-Action iKT framework [14,15] to systematically develop protocols/standards (knowledge products) and address the characteristics of the clinician, the context, and the broader healthcare system (application of knowledge) that influences the adoption into clinical practice [15-17]. The CARE study revealed that more than 80% of audiologists did not have access to guidance documents to implement RC [9]. This barrier could result in practice variation and/or non-implementation of RC, both of which can lead to poor quality of services and harmful interventions [15]. Using the iKT framework and active collaboration with end-users of the knowledge, we can develop tailored protocols to guide RC in practice.
It is also important to attend to the factors associated with the integration of knowledge into practice [14,15,18]. Accordingly, we have developed an approach using a multi-component strategy attending to the range of processes, from pre-implementation conditions through to ensuring sustainability [8,19]. We feel it is important to consider supplemental materials, such as education/coaching, feedback, recommendations for set-up and support needed to change practice behaviour across the complex contexts in which RC might occur.
Aptitude readiness
Susan Michie and colleagues at University College London’s Centre for Behaviour Change have created a behaviour change technique-mechanism of action pathway through which behaviour change occurs [20,21]. Findings from the CARE study suggest that audiologists feel they lack knowledge and skills to deliver RC [9]. Research and expert consensus has shown that if a change in knowledge/skills is desired, this might occur via instruction on how to perform the behaviour, feedback, coaching, graded stages of implementation, rehearsals, and information about social and environmental consequences if the behaviour is not performed correctly [20,21]. Our implementation activities will include collaboration with end-users to determine behaviour change techniques and materials that best target knowledge, skills and behaviours to facilitate remote care.
“This barrier could result in practice variation and/or non-implementation of RC, both of which can lead to poor quality of services and harmful interventions”
Take-away message
Are you ready to deliver remote audiological care? This article has described our approach to implementation of remote audiological care that attends to measuring the factors affecting the readiness of clinicians and organisations, and then suggests that gaps in readiness behaviour be addressed through an examination of action pathways through which change might occur.
References
1. Gladden C, Beck L, Chandler D. Tele-audiology: Expanding access to hearing care and enhancing patient connectivity. Journal of the American Academy of Audiology 2015;26(9):792-9.
https://doi.org/10.3766/jaaa.14107
2. Glista D, O’Hagan R, Moodie STF, Scollie S. An examination of clinical uptake factors for remote hearing aid support: A concept mapping study with audiologists. International Journal of Audiology 2020;1-10.
https://doi.org/10.1080/
14992027.2020.1795281
3. Holt DT, Helfrich CD, Hall CG, Weiner BJ. Are you ready? How health professionals can comprehensively conceptualize readiness for change. Journal of General Internal Medicine 2010;25(S1):50-5.
https://doi.org/10.1007/
s11606-009-1112-8
4. Wade VA, Eliott JA, Hiller JE. Clinician acceptance is the key factor for sustainable telehealth services. Qualitative Health Research 2014;24(5):682-94.
https://doi.org/10.1177/
1049732314528809
5. Ravi R, Gunjawate DR, Yerraguntla K, Driscoll C. Knowledge and perceptions of teleaudiology among audiologists: A systematic review. Journal of Audiology and Otology 2018;22(3):120-7.
https://doi.org/10.7874/
jao.2017.00353
6. Maunder K, Walton K, Williams P, et al. A framework for eHealth readiness of dietitians. International Journal of Medical Informatics 2018;115:43-52.
https://doi.org/10.1016/
j.ijmedinf.2018.04.002
7. Rycroft-Malone J. The PARIHS Framework—A framework for guiding the implementation of evidence-based practice: Journal of Nursing Care Quality 2004;19(4):297-304.
https://doi.org/10.1097/0000
1786-200410000-00002
8. Moodie STF. Implementation matters [Doctoral Comprehensive Exam]. University of Western Ontario 2011.
9. Perez L, Scollie S, Moodie STF, et al. An exploration of audiologists’ readiness to adopt connected hearing healthcare for remote hearing aid fitting. 2020 HRS Graduate Research Conference.
10. Glista D. Factors driving clinical readiness and uptake of remote hearing aid support services [Conference Presentation]. ARC 20: Tele-Audiology: Theory to Practice, Virtual.
11. Duda MA, Jaouich A, Wereley TW, Hone MJG. How to apply implementation science frameworks to support and sustain change. In: Pollastri AR, Ablon JS, Hone MJG (Eds.). Collaborative Problem Solving: An Evidence-Based Approach to Implementation and Practice. Springer International Publishing. 2019:33-62
12. Fixsen DL, Blase KA, Naoom SF, Wallace, F. Core implementation components. Research on Social Work Practice 2009;19(5):531-40.
https://doi.org/10.1177/
1049731509335549
13. Fixsen DL, Naoom SF, Blase KA, et al. Implementation research: A synthesis of the literature. Florida, USA; University of South Florida, Louis de la Parte Florida Mental Health Institute, The National Implementation Research Network; 2005.
14. Graham ID, Logan J, Harrison MB, et al. Lost in knowledge translation: Time for a map? Journal of Continuing Education in the Health Professions 2006;26(1):13-24.
https://doi.org/10.1002/chp.47
15. Moodie STF. An integrated knowledge translation experience: Use of the Network of Pediatric Audiologists of Canada to facilitate the development of The University of Western Ontario Pediatric Audiological Monitoring Protocol (UWO PedAMP v1.0). PhD Thesis, University of Western Ontario, 2012.
https://ir.lib.uwo.ca/cgi/viewcontent.
cgi?article=1511&context=etd
16. Glista D, Scollie S, Moodie STF, et al. The ling 6(HL) test: Typical pediatric performance data and clinical use evaluation. Journal of the American Academy of Audiology 2014;25(10):1008-21.
https://doi.org/10.3766/jaaa.25.10.9
17. Moodie STF, Bagatto MP, Miller LT, et al. An integrated knowledge translation experience: Use of the network of pediatric audiologists of canada to facilitate the development of the university of western ontario pediatric audiological monitoring protocol (UWO PedAMP v1.0). Trends in Amplification 2011;15(1):34-56.
https://doi.org/10.1177/
1084713811417634
18. Wensing M, Bosh M, Grol R. Selecting, tailoring, and implementing knowledge translation interventions. In: Straus S, Tetroe J, Graham ID (Eds.). Knowledge Translation in Health Care: Moving from Evidence to Practice. Blackwell Publishing Ltd; 2009:94-112.
19. Kilbourne AM, Neumann MS, Pincus HA, et al. Implementing evidence-based interventions in health care: Application of the replicating effective programs framework. Implementation Science 2007;2(1):42.
https://doi.org/10.1186/1748-5908-2-42
20. Carey RN, Connell LE, Johnston M, et al. Behavior change techniques and their mechanisms of action: A synthesis of links described in published intervention literature. Annals of Behavioral Medicine 2018;53:693-707.
https://doi.org/10.1093/abm/kay078
21. Connell LE, Carey RN, de Bruin M. Links Between Behavior Change Techniques and Mechanisms of Action: An Expert Consensus Study. Annals of Behavioral Medicine 2019;53(8):708-20.
https://doi.org/10.1093/
abm/kay082







