The COVID-19 pandemic has required healthcare services globally to show both resilience and ingenuity in redesigning services to meet the ever-changing needs of our patients. We hear about the redevelopment of clinical pathways within an hearing implant service, and the success and challenges from both a clinician and patient perspective.
A blended service
As Guy’s and St Thomas’ was a front line COVID-19 hospital, the Hearing Implant Centre needed to move any routine care to remote appointments and only offer face-to-face (F2F) appointments where remote care is not possible.
To achieve this, we worked quickly to identify what we could deliver remotely and moved towards a ‘blended service’. We identified that tasks such as audiometry, calibrated speech perception testing and Cochlear Implant programming needed to be performed F2F, but that most other patient contact could be carried out remotely.
To make the blended service work, our team was set up with remote technology, including a Trust laptop with access to the IT system, headsets, mobile phones, and dummy implant devices. Doing so not only enabled us to connect with patients at home, but also enabled our staff to work off-site, further reducing footfall through the department. Virtual rehabilitation, which includes counselling, structured listening activities, interactive telephone and music training, made up the majority of our blended service. To deliver this effectively, we developed a wealth of materials including a variety of information sheets, documents, subtitled videos on our Trust webpage, editable PDF questionnaires and rehabilitation materials for use during remote care sessions or between appointments.
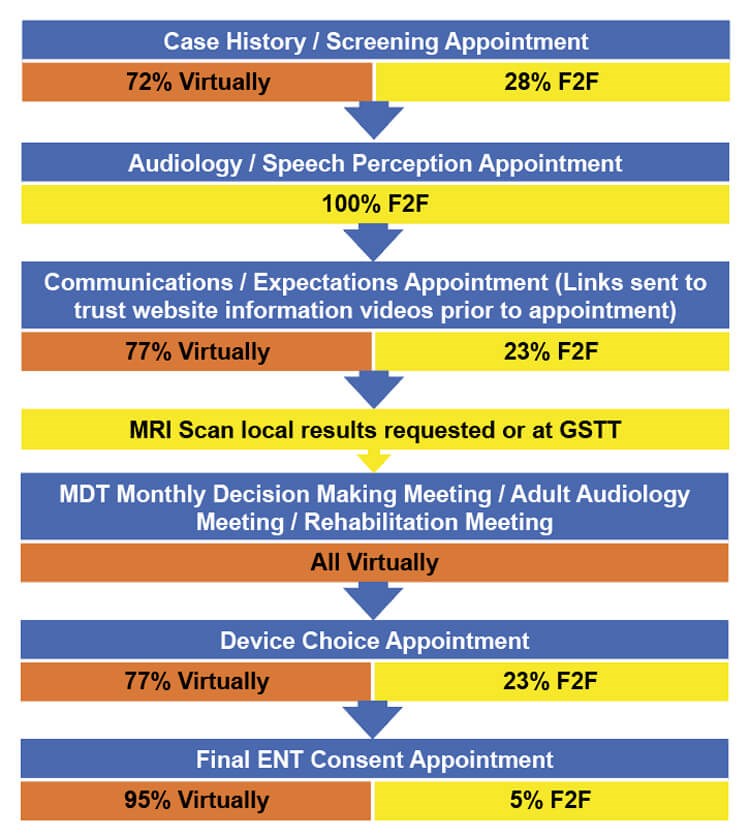
Image 1. The Adult CI Assessment Pathway. Statistics from July/August 2020.
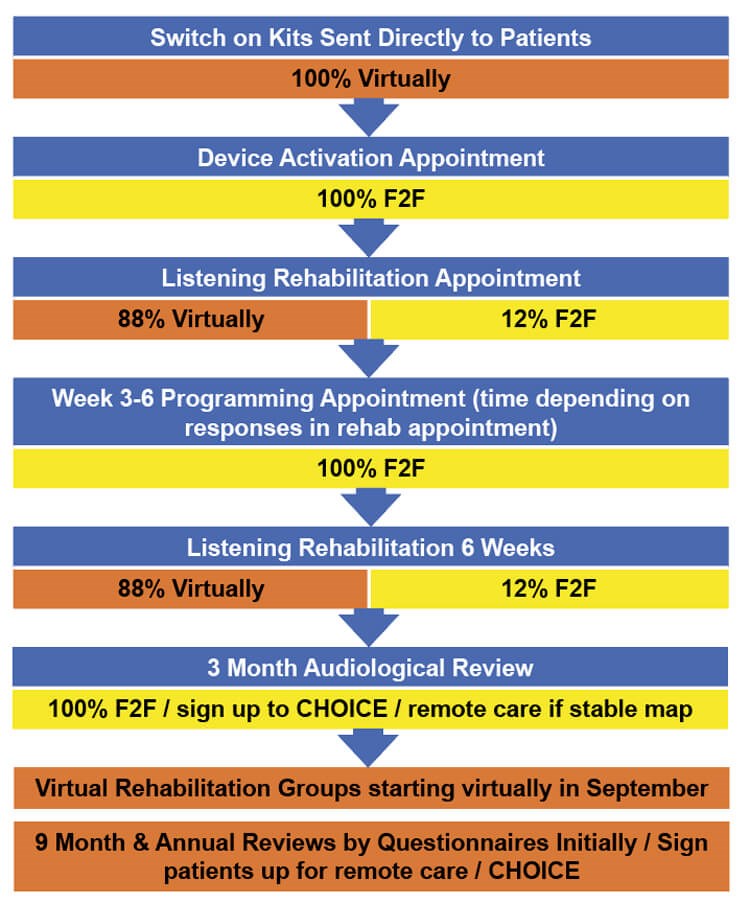
Image 2. The Adult CI Post-Op Pathway. Statistics from July/August 2020.
As can be seen in images 1 and 2 the majority of adult appointments in our blended service are now offered virtually; there is a similar configuration in the paediatric service. This has allowed our patients to continue on their journey to receiving hearing implants and have their postoperative care supported from the comfort of their home. As we already had an established repair service delivered by the cochlear implant companies, we were also able to keep patients’ equipment functioning throughout the pandemic.
Patient feedback
Moving towards a blended service was a significant change in our practice. To measure the impact of this change, a feedback survey was conducted for patients seen for remote care appointments between May and October 2020. Feedback from patients and their families was overwhelmingly positive, with key highlights including:
- 88% of patients reported either a good or very good experience at the appointment.
- 91% of patients reported that they were able to get everything from the appointment that they would have in an F2F.
- 100% of patients either agreed partly or fully that they felt as involved in decisions about their care as they wanted to be.
- 97% expressed an interest in having their next appointment remotely.
Patients were also invited to leave further comments, with themes including the benefits of not having to travel, both with time saving and personal safety, which cannot be underestimated in the current climate. Particularly positive feedback was also received following our group remote music sessions, with one patient reporting that they had “the confidence to listen to music and sing along with it too” and that after the session, they “had a smile on their face all evening”.
There were, of course, challenges presented with remote care appointments, with parents commenting on the difficulty of distracting younger children whilst engaging in a remote care appointment and the limitations of not being able to perform diagnostic assessments over the internet. However, the overall consensus from our initial feedback has been extremely positive.
Staff feedback
Given the sizeable change to our way of working, staff were also asked to provide feedback on their experiences of working remotely and the success of their appointments. As with any change, there have been some early successes and some challenges but, on the whole, staff have embraced our new normal:
“The family were very happy and relaxed to have this appointment. I enjoyed it despite the challenges.”
“Was able to have a good discussion with the patient to review their progress with their implant and identify any specific rehab goals. Easier than back and forth email correspondence and avoiding unnecessary travel for the patient.”
“It worked well to do this via video rather than phone, to build rapport more easily.”
“Video session was good for a conversation with the parent, but not so good for seeing mum playing with the child – as she had to hold phone and child was playing on his own.”
“Would normally see the child in class and observe the listening environment and observe/advise staff.”
“It takes time to keep turning captions on for explanation then off for listening activities.”
What we have learned
- Don’t lose touch with the team - The team meet regularly for virtual case discussions, service improvement meetings and multidisciplinary team meetings via Microsoft Teams. We have also increased our use of telephone calls, rather than emails to individual colleagues to encourage and promote team cohesion.
- Not all platforms are created equally - We trialled multiple platforms and found noticeable differences in stability and functionality. We eventually opted to proceed with Microsoft Teams. However, we have also had Information Governance approval to use alternative platforms that patients are already familiar with, such as FaceTime, WhatsApp call and Zoom, to help with engagement of some families.
- You don’t need to be F2F to use an interpreter - interpreters for British Sign Language (BSL) and non-English speakers have been able to join our remote care sessions. Patients are able to ‘Pin’ the interpreter so that they are large and centre screen.
- Technology does not work for everyone - A small minority of patients didn’t have the technology available or were not confident enough to trial remote care. To help to build the confidence, we have worked to develop patient guides, involved families/carers and asked our assistant to do some test calls with the families. For those who didn’t have the technology, we reviewed their case on an individual basis to determine whether they needed to be seen immediately for a F2F or whether their appointment could be delayed.
- Diversify your resources - We identified that specific paediatric rehabilitation materials (books, toys etc.) are needed to use with parents when working across a remote platform. We have secured some charitable funding to support this and look forward to improving our offer further.
- Find your new normal - Initially it took some time to find our feet with remote care and we found that the flow of discussions and the appropriate virtual etiquette did not come naturally. We have since developed some guidelines to support our staff in adapting to delivering remote care.
What’s next?
- We await an upgrade to Microsoft 365 to allow us to make use of additional functionality, such as advanced live captioning.
- We continue to increase the number of patients accessing remote care, with a view to see all rehabilitation patients with a stable map remotely.
- We continue to develop our rehabilitation materials across both paediatrics and adults to fully support our patients as our experience grows.







