Passive whole body rotation tests are widely considered to be the ‘gold standard’ for the identification of bilateral peripheral vestibular disorders (bPVD), but also have a part to play in identifying unilateral disorders (uPVD). In this article Paul Radomskij discusses the benefits of taking your patients for a “short spin”, reviewing the application and clinical utility of passive rotation tests in identifying vestibular disorders and why they should be considered to be an essential part of your vestibular test battery.
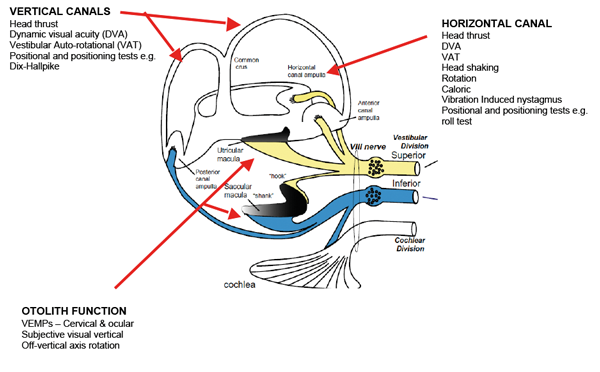
Figure 1: The peripheral vestibular labyrinth system and some of the vestibular tests available. Adapted from Curthoys IS. A critical review of the neurophysiological evidence underlying clinical vestibular testing using sound, vibration and galvanic stimuli. Clinical Neurophysiology 2010;121:132–44.
Vestibular test battery and rationale for rotation tests
It is well understood that the evaluation of patients with dizziness and / or imbalance can not only be a cause of consternation and worry for the patient but also the clinician. Whilst a good history and basic clinical tests can partially complete the diagnostic jigsaw there will always be a need to carry out objective tests of vestibular function on some patients. The range of tests available in a fully equipped vestibular laboratory is extensive; Figure 1 illustrates some of these tests and the part of the peripheral vestibular labyrinth system being assessed.
“When determining the best vestibular ‘frequency’ to test, it is useful to go back to the basics of the auditory system.”
Of course each test is not only assessing a particular end organ and pathway, but can also be considered to be assessing its function at a particular frequency. The frequency sensitivity of the vestibular system (vestibular-ocular reflex, VOR) is demonstrated in Figure 2. Like the auditory system, the vestibular system is frequency dependent. The horizontal semicircular canal of the vestibular apparatus is arranged in such a way that it is able to represent various frequencies spectra, likewise the auditory system. Whether the neural vestibular system has tonotopic frequency representation like the auditory system is not known.
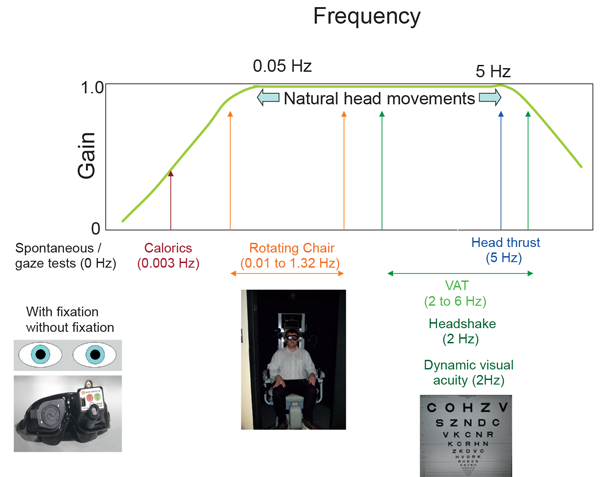
Figure 2: Frequency response of vestibular system – horizontal semi-circular canals
(modified from a diagram provided by Dr Paul Bacon).
In determining the appropriate test battery, it would be helpful to know which part of the vestibular apparatus as well as vestibular test frequency is going to be the most sensitive and specific in identifying the patient’s vestibular disorder.
Maes et al. (2011) carried out an excellent study investigating the “clinical usefulness of rotatory, caloric and vestibular evoked myogenic potential (VEMP) tests in unilateral peripheral vestibular pathologies” [1]. Surprisingly, they found that rotation tests (nominal low frequency of 0.01Hz, 0.05 Hz and high of 0.1Hz) had a higher sensitivity but lower specificity than the caloric test in identifying uPVDs. Correspondingly, the VEMP test was more specific but less sensitive than the caloric test.
When determining the best vestibular ‘frequency’ to test, it is useful to go back to the basics of the auditory system. For example, when investigating hearing, it is standard practice to measure a range of frequencies, typically 250Hz to 8 kHz and on occasions it might be useful to measure even up to 16 kHz. Measuring the hearing levels at only one frequency, would clearly provide limited information on the overall frequency sensitivity of hearing but it might be enough to predict, with a reasonable level of confidence, normal hearing. If you could only test one frequency, for example in neonates, it might be sensible to choose 4 kHz [2], as this appears to be the most sensitive in the identification of sensorineural hearing loss. If a hearing loss is estimated, other frequencies can then be tested.
Switching now back to the vestibular system. To have a complete understanding of its function or dysfunction, one might think it is necessary to carry out a range of tests that would allow the frequency sensitivity of the vestibular system (‘vestibulo-gram’) to be established across the full operational range. However, a good history and basic clinical ‘bedside’ tests may be sufficient to either make a diagnosis and / or plan treatment for most patients. It is clearly unrealistic to develop a full vestibulo-gram for every patient with dizziness.
However, in the era of evidence based treatment, some patients will still require at least some objective tests to establish the status of their vestibular system and clarify whether their symptoms have a vestibular or non-vestibular cause. So, which vestibular test frequency has the greatest diagnostic capacity and accuracy? Which tests should be carried out? If you are lucky, either through fortunate inheritance or by design, you may have access to a range of balance testing equipment; if you are very lucky this will include a motorised rotating chair. The latter would allow you to carry out a rapid evaluation of the horizontal semi-circular canals over a range of frequencies. It is usually well tolerated and easy to modify in patients as required. In seven years of testing on our new system, only one patient tested has come close to being sick. Clearly passive horizontal whole body rotation tests (where the patient’s entire body is moved as opposed to active head rotation in which the patient voluntarily moves their own head) are limited in that they are used to assess only “20% of the vestibular system”.
However, depending on the type of system used, the rotating chair can be used to evaluate vestibular system frequency response from 0.01Hz to 1.28Hz, although testing above 1Hz involves additional technical challenges, specifically minimising relative movement between the patient’s head and their body. The peak velocity for each of these sinusoidal test frequencies can be as low as 30˚s-1 (as may be used for testing patients with motion sickness) to 120˚s-1 or higher (for patients with bilateral hypo-function).
From our audit of 1500 patients, the highest diagnostic yield for uPVD (33.9%) was derived from testing at either a low frequency of 0.01 Hz (motorised chair) or even lower frequency equivalence of 0.003 Hz (the caloric test1). The diagnostic yield for uPVD at higher test frequencies is relatively small (4.2% at 0.32Hz). Perhaps the rumour of the demise of the caloric test in the era of objective head thrust test is either incorrect or at best premature. Testing patients with suspected bilateral vestibular failure, residual function can be established with the rotating chair, e.g. a patient may have abnormal responses at low frequency sinusoidal rotations (e.g. 0.01Hz) but normal at higher frequencies (e.g. 0.28Hz).
If you decide to take your patients for a spin, a basic test battery might include the following:
- Impulsive rotation with a peak velocity of 60˚s-1, measuring the per- and post- rotation responses to clockwise and counter-clockwise.
- Sinusoidal rotations with a peak velocity of 60˚s-1 over a range of frequencies, e.g. 0.01, 0.02, 004, 0.08, 0.16, 0.32, 0.64 Hz.
- Repeating the sinusoidal tests at 0.08 or 0.16Hz with fixation to assess VOR suppression.
- By projecting a more complex static pattern across the patient’s full field of vision (e.g. stripes or random pattern of circles), one can assess the interaction between optokinetic nystagmus and rotational VOR and thereby have a measure of VOR enhancement. This parameter has been useful in the evaluation of patients with visual dependency (‘visual vertigo’).
Needless to say, software analysis of test results is essential and would require a small chapter to go through in detail. Indeed if you want to know more, you are directed towards the excellent textbook, Balance Assessment and Management (Jacobson and Shepard, 2014) [3]. The key principle to note is that the resulting nystagmus from the rotation tests can be reduced to a few basic parameters: peak eye velocity, gain (eye velocity divided by chair velocity), asymmetry or directional preponderance (difference in gain between right and leftwards rotations), phase difference (error between timing of max head velocity versus maximum chair velocity), time constants (time for nystagmus velocity to decay to e-1 of max velocity) and spectral purity (how ‘good’ are your results).
1The caloric test is often quoted as being equivalent to a low frequency sinusoidal rotation of 0.003Hz. This equivalence may be derived as follows. Consider the time it takes for the caloric response to decay from the peak, Td, to be 90 seconds. Td could be viewed as a ¼ cycle of a sine wave; the period of the sine wave would be 4*Td. Therefore, the frequency is equivalent to 1 / (4*Td) i.e. 1/360=0.003Hz!
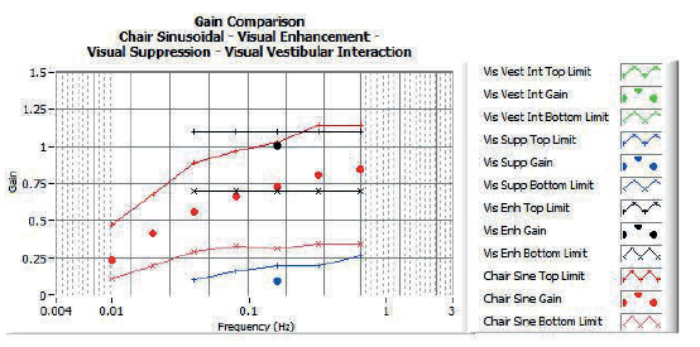
Figure 3: Sinusoidal rotation result – normal gains.
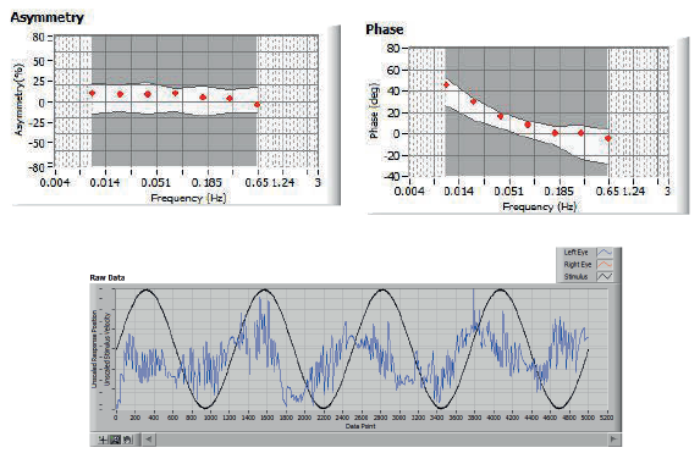
Figure 4: Sinusoidal rotation result – normal phase and asymmetry.
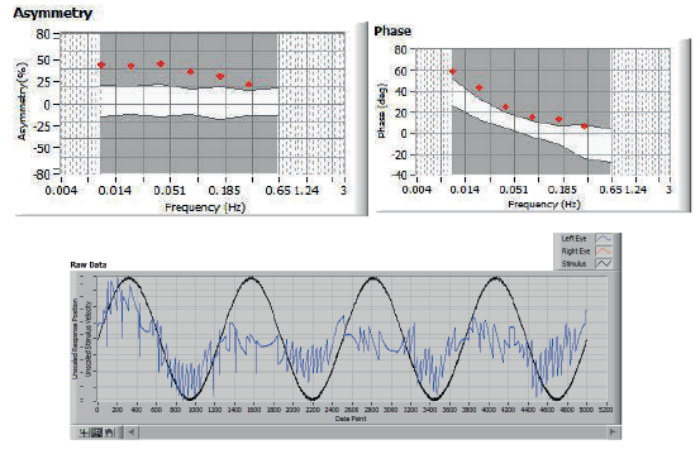
Figure 5: Sinusoidal rotation result – abnormal phase (increased) and asymmetry (left direction preponderance).
From these parameters, it is possible to infer a substantial amount of information about the status of the vestibular system. For example, phase lead abnormality is often increased in peripheral vestibular disorders and decreased in central; peripheral disorders may often result in significant asymmetrical rotation response (no central signs identified with ocular-motor testing) whereas central may be expected to result in abnormally short or long time constants (possible velocity storage mechanism abnormality / dis-inhibition). Clearly there are always going to be exceptions to these guidelines and more research is required. However, one cannot simply assume that rotation tests can never differentiate between central and peripheral vestibular disorders. Rotation tests combined with ocular motor testing are a powerful tool in differential diagnosis, although the caloric test still remains the ‘gold’ standard for identifying peripheral vestibular lesions. Figures 3 and 4 are sinusoidal rotation results from a normal subject and Figure 5 shows results from a patient with confirmed right peripheral vestibular lesion. Using a modified rotating chair with greater torque than most commercially available, it is possible to conduct even more sophisticated tests of otolithic function, specifically off-vertical axis rotation and unilateral centrifugation.
References
1. Maes L, Vinck BM, Wuyts F, D’Haenens W, Bockstael A, Keppler H, Philips B, Swinnen F, Dhooge I. Clinical usefulness of the rotatory, caloric, and vestibular evoked myogenic potential test in unilateral peripheral vestibular pathologies. Int J Audiol 2011;50(8):566-76.
2. Sutton G, Lightfoot G, Stevens J, Booth R, Brennan S, Feirn R, Meredith R. Guidance for Auditory Brainstem Response Testing in Babies Version 2.1. NHSP Clinical Group; 2013. Available from
http://www.thebsa.org.uk/wp-content/
uploads/2014/08/NHSP_ABRneonate_2014.pdf
3. Jacobson GP, Shepard NT (Eds). Balance assessment and management. 2nd Edn. San Diego, CA; Plural Publishing; 2014.
Acknowledgements
A big thank you to Sam and Spike from the Audiology department at St George’s Hospital, London for help with the photography (Figure 2).
Declaration of competing interests: None declared.
SUMMARY
Disadvantages of rotation tests
-
Whole body rotation tests are mainly designed to test the lateral semi-circular canals i.e. only 20% of the vestibular labyrinth
-
Both labyrinths are tested simultaneously therefore it is difficult to provide ear-specific information, even with techniques such as a sinusoidal pulsed test paradigm
-
Relatively expensive.
Advantages of rotation tests
-
Considered to be the ‘gold standard’ for the assessment of bilateral vestibular dysfunction
-
Rotation test frequency of 0.01Hz, in combination with gaze testing, may be more sensitive but less specific than caloric testing at identifying unilateral peripheral lesions
-
Rotation tests are easily tolerated by adults and children and can be modified for patients with motion sensitivity or bi-lateral reduction in function. Typically adults find the tests interesting and many are able to intuitively understand the basic physiology
-
One can test a wide range of frequencies and peak velocities, specifically the frequency components 0.01 to 1.32 Hz, significant components of the vestibulo-gram. To rotate or not to rotate? The answer from the author is a resounding ‘yes’.