Marie Wardle is the Programme Director of the Interpersonal Therapy department in the West Midlands, UK and part of her role is to deliver supervision training courses for therapists in the region. Therapists, whether supporting patients with psychological or physical health problems often have to deal with information or emotions which may well have an impact on their own wellbeing. Here she explains the role of supervision for therapists and how such supervision could be delivered in the audiology profession.
Supervision is a formal arrangement for therapists to discuss their work regularly with someone who is experienced in the same profession, and also qualified in supervision. In some settings supervision may also incorporate elements of training and assessment.
Supervision can be conducted on a one-to-one basis between a supervisor and supervisee, or in group supervision with more than one supervisee. In some settings, peer supervision groups can be formed, and this can also be very effective. Peer group supervision is not recommended for a newly qualified therapist, as members of the group should ideally be of equal status with similar training and experience. Whatever the chosen format, the supervisory relationship is at the heart of effective supervision [1]. The role of a supervisor is to “send the other person away more aware, more informed, skilled and encouraged than she was when she came in” [2].
The role of supervision is to have a place to go and not know the answers, and a place to work things out. It’s also a place to be reassured, supported, and somewhere to take the emotional disturbance of clinical work to be survived, shared, understood and reflected upon, and to receive helpful and constructive feedback.
Traditionally, clinical supervision has been more aligned to working within psychological therapies. This is standardised practice and covers issues around managing risk, organisational issues, ethical considerations, the therapy process, and a written contract will often be written up that outlines the responsibilities of each party. The British Association for Counselling and Psychotherapy (BACP) Ethical Framework is available online for anybody who wants to understand more about the principles of supervision [3]. However, we are seeing more interest from other NHS professionals who want to receive regular supervision to support their work in a wide range of in-patient and out-patient clinics. Patients, who attend treatment for their physical health may well also be experiencing psychological difficulties, and the therapist may not know how to support the patient, or where to get additional help and resources for that person. The therapist can often be left with distress, feelings of being overwhelmed, or at a loss as to how to process the information that has been passed to them. The benefits of having regular and ongoing formal supervision are many, and support good practice. Supervision is also important for the therapist’s own health and well-being.
“The benefits of having regular and ongoing formal supervision are many, and support good practice.”
Supervision can be set up in various ways, depending on the setting and what type of practice people are employed in, and what the supervision is for. Different models can be employed to assist in the process and can help to shape and focus the supervision practice. This article gives a brief overview of four well-known models that can be employed in clinical supervision, but there are many more models that can be used.
The developmental model
This model is continually identifying new areas for growth and learning, and focuses on the change in awareness, motivation and autonomy. The supervisor will consider what stage the supervisee is at, i.e. beginner, intermediate, or advanced, and recognise that the levels of motivation, autonomy and self-awareness may differ from person to person.
The therapy specific model
This is where the supervision will mirror and model the therapeutic process, with shared orientation modelling maximised as the supervisor teaches and theory is fully integrated into training. This can be particularly good where there is a specialised service or product, rather than generic supervision, and particular components need to be discussed as part of the supervisory process.
The process model
This was devised by Hawkins and Shohet [4] and is used commonly in counselling and psychotherapy supervision. This model focuses on the therapist’s and supervisor’s countertransference, and can be very valuable in gaining insight into what is happening for the client in the client/therapeutic relationship. Whilst the client and therapist may be grappling with something that is not understood or known between them, somehow within supervision, that which is hidden or still unconscious can be revealed; almost like magic the solution is visible. The image above gives a flavour of how the process unfolds, but also captures the ‘super vision’ that is somehow accentuated between the therapist and supervisor when a ‘space’ is created to explore the arena together (Figure 1).
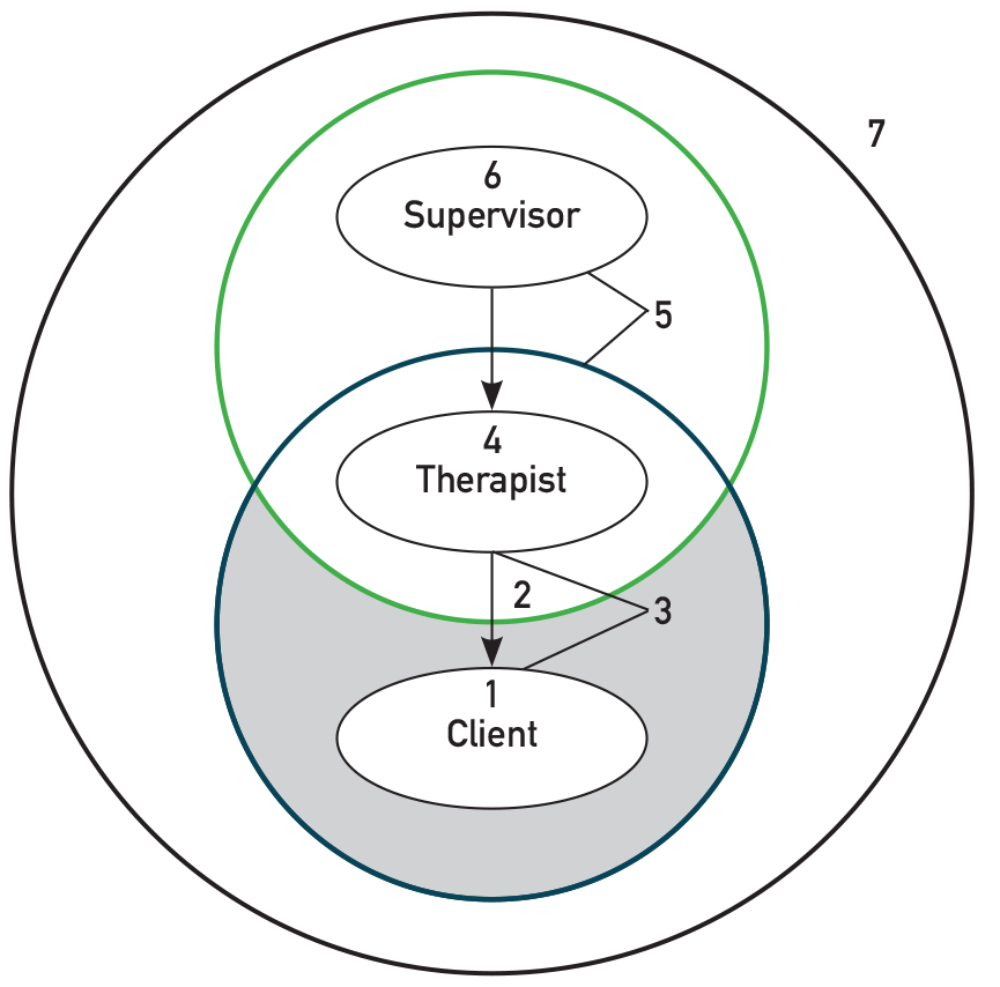
Figure 1. The process supervision model.
Taken from Hawkins and Shohet [4].
The cyclical model
Devised by Page and Woskett (2001) [5], this is a simple, clear, five-stage model, with every stage also having five areas to address. As the model is quite focused, it lends itself to working around a medical model and compliments evidence based practice.
Stage 1 – ‘The contract’ looks at the ground rules: time-keeping, boundaries, relationship expectations and accountability. This stage provides structure and direction.
Stage 2 – ‘Focus’ addresses relevant issues, objectives, presentation, approach and priorities. Any clinical risks at this juncture would be addressed and guidance as to how to manage these would follow.
Stage 3 – ‘The space’ identifies a place where insight can occur. We investigate, challenge, but offer containment and a sense of security for the insecurities of the supervisee. We would hope to open up the creative space and voice, slow things down, pause and allow new ideas and images to surface.
Stage 4 – ‘The bridge’ involves consolidation, information giving, goal setting, action and planning.
Stage 5 – ‘Review’ is where we feed back, give appraisal and evaluation, review and summarise.
Training to be a supervisor
There are lots of supervision training courses that are available, and some reside within the NHS. There are some very basic courses available, or those that can attain a postgraduate level of training, usually within university settings, or smaller training institutions. Most courses will look at various models. It is worth considering whether such courses are more geared towards psychological therapies or whether they specialise in supervision for other professionals.
Final thoughts
Having regular supervision can really prevent things getting stuck and allow new insights and new energy to move things forward in our clinical work. Supervision is also about promoting safe practice. With the new Data Protection Regulations (GDPR) now in force we are all affected in how we use, store and access sensitive data about our clients and patients. In supervision we continue to develop our practice, and reduce the isolation that can often come in busy clinical settings. This can only enhance the well-being of the workforce and promote good working relationships, having time set aside from the demands of our daily practice and caseload.
References
1. Stafford DE. Supervision – the grown-up relationship? Therapy Today 2008;19(6):42-4.
2. Houston G. Supervision and Counselling. London, UK; Rochester Foundation; 1990.
3. BACP. Ethical Framework for Good Practice in Counselling and Psychotherapy. Lutterworth, UK; BACP; 2010.
4. Hawkins P, Shohet R. Supervision in the Helping Professions (Third Edition). London, UK; Open University Press; 2007.
5. Page S, Wosket V. Supervising the Counsellor, A Cyclical Model (Second Edition). London, UK; Routledge; 2001.





