James Bates and Chris Frerk are both passionate about how human factors science can improve safety in healthcare and have co-authored this article describing how communication, ergonomics and other non-technical skills are making operating theatres safer. There is no doubt that this work will continue to develop our practice and this article explains how.
The scientific discipline of Human Factors (HF) is a broad-based specialty with influences from psychology, anthropology and engineering. In the clinical context it is defined as “enhancing clinical performance through an understanding of the effects of teamwork, tasks, equipment, workspace, culture and organisation on human behaviour and abilities” [1].
The value HF can add in healthcare is being increasingly recognised, partly because of widespread reporting of patient stories [2,3] which have raised awareness and understanding, but the pace at which HF is becoming embedded in clinical practice varies widely between hospitals, specialities and clinicians. This article briefly describes some of the aspects of HF that are particularly relevant to ENT and anaesthesia with examples to help improve patient outcomes and clinician experience.
Teamworking, communication and culture
The ability to lead and work as part of a team is now recognised as an essential skill for ENT surgeons; just having a ‘good pair of hands’ is no longer enough. Being able to articulate the surgical plan to the team, cover possible areas of difficulty and the preparations needed to be in place to deal with them are critical aspects of the leadership role. These skills appear to come naturally to some but can be taught, learned and practised by all. Being able to decrease the authority gradient within the team (while still maintaining the leadership role) facilitates ‘speaking up’, allowing useful contributions from all members of the team contributing to patient safety and also making for a pleasant working environment. Human factors science describes the key components of these skills which can be taught and assessed using validated tools such as NOTSS (Non-Technical Skills for Surgeons).
The WHO checklist, published in 2008, was designed to encourage these behaviours within surgical teams and is supported by patients [4]. While a recent BMJ article has questioned if the impact of the WHO checklist is being overestimated [5], the authors acknowledge that it has had a meaningful impact through improving team dynamics and communication which are key elements in HF.
Within the ENT theatre team, surgeon and anaesthetist have traditionally had a close working relationship, because of the shared airway. The HF term that encompasses the working relationship is ‘shared situation awareness’ where the two clinicians both understand the big picture including their colleague’s current and likely future requirements to enable optimal surgical and anaesthetic care. This can only be facilitated by continuing non-confrontational dialogue between professionals.
Equipment design, physical and mental workload
The design of the equipment we use directly impacts on our clinical performance, and assessment of how workers interact with equipment is a vital part of the human factors professionals’ work. Sub-optimally designed equipment affects our working environment and impacts directly on patient care.
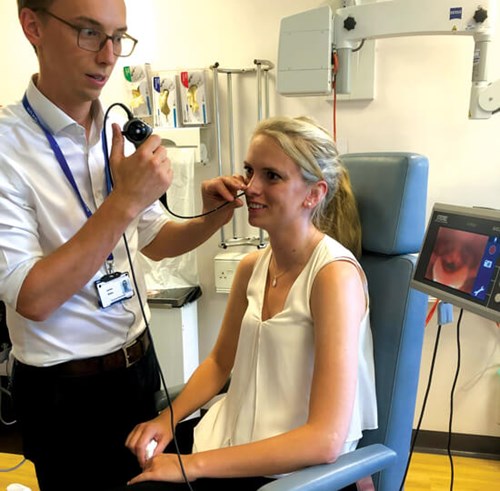
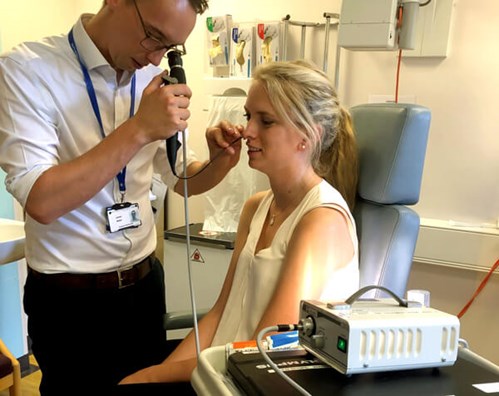
Figure 1a & 1b. A comparison between two designs of flexible nasendoscope.
An example which all ENT surgeons can relate to is the flexible nasendoscope. The use of chip camera scopes with high-definition screens allows the clinician to work in a much more comfortable position through a long clinic than when having to use a traditional optical nasendoscope with an eyepiece (see Figure 1a & 1b). As well as reducing the risk of musculoskeletal disorders over the course of a career, the tiredness and discomfort associated with poor positioning during a long clinic undoubtedly risks impairing performance towards the end of the day.
Even small differences in design, such as in the hand grip and tip control lever, can make the use of one nasendoscope easier and less tiring than another; similarly, scopes that require external power sources are more difficult to transport and use, especially when attending an emergency. The lack of facility for recording and storing images with some nasendoscopes also clearly impacts on patient safety. All of these factors should be taken into consideration when making purchasing decisions as choosing the best-designed equipment decreases the surgeon’s workload improving the margins for safe care.
New surgical and anaesthetic equipment and techniques are continually being developed. New doesn’t always mean better but if there is evidence of improved patient outcomes, we should work to incorporate new developments into our practice. It is important to understand that learning new techniques with new equipment takes up a significant proportion of a clinician’s spare mental capacity, eroding safety margins and during this ‘learning period’ we should compensate for this, perhaps by booking one less case in each clinic or operating list.
Many surgeons will understand this in relation to the changing practice of paediatric tonsillectomy for obstructive sleep apnoea. Intra-capsular tonsillectomy (tonsillotomy) with the use of coblation is a contemporary technique becoming more popular than the more conventional extra-capsular tonsillectomy [6]. It is claimed that tonsillotomy has a reduced postoperative haemorrhage rate loss, pain and a quicker return to normal activities [7]. Once familiar and comfortable with the technique, few surgeons would return to their previous practice but anyone who has made the transition will know well the increased workload associated with learning the new technique.
We should understand that this is equally true for anaesthetists. Many rhinologists are aware of research demonstrating that total intravenous anaesthesia (TIVA) is associated with improved surgical field and decreased intraoperative blood loss when compared to inhalation anaesthesia [8]. However, fewer than 10% of anaesthetists use TIVA regularly and there are significant differences in the technical skills and cognitive workload required to deliver anaesthesia using a total intravenous technique compared to using traditional inhaled anaesthetic methods. This makes many anaesthetists reluctant to try to develop these skills on a busy ENT list where turnaround times are critical to avoid patient cancellations. Providing support to anaesthetic colleagues while they develop skills in new techniques (such as reducing the number or complexity of cases on a list) will allow the hospital’s ENT service to evolve in line with developing evidence.
An extreme example of this is seen with recent developments in laryngeal surgery, an area that has always pushed the boundaries of teamwork with anaesthetist and surgeon making various compromises to deliver the best outcome for each patient. The ideal airway for the surgeon is one that is completely stationary and is free of tubes, catheters or other equipment obscuring the view of any part of the larynx. A new method of oxygen delivery is able to facilitate this in certain situations. Transnasal humidified rapid-insufflation ventilatory exchange (THRIVE) is able to provide apnoeic oxygenation while enabling unencumbered access to the glottis and is revolutionising elective and emergency airway surgery.
Although this provides potential advantages to patients, developing this service adds a significant workload to anaesthetic teams, requiring TIVA (as discussed above) while simultaneously removing one of the anaesthetists professionally mandated critical safety monitors (capnography). This requires optimal co-operation and communication between surgical and anaesthetic teams to ensure continued safety during surgery. Teams that embrace human factors as part of their normal way of working will find it less difficult to introduce and maintain new services, such as this, safely into their practice.
Conclusion
Team working, communication, culture, equipment design, physical and mental workload all affect our performance. A negative impact in any one of these domains has a detrimental effect on patient safety. HF as a discipline is used to identify areas for improvement and help to optimise our performance. There is no doubt that HF will continue to impact our clinical practice although the rate of change of clinical practice to include HF has been described as glacially slow [9]. The majority of HF education in healthcare is delivered as part of simulation training, and although this now forms part of the curriculum in ENT surgery, it is not yet as widely embedded as in anaesthesia training. This probably simply reflects the fact that the majority of simulation faculty have a background in anaesthesia and so the training is continued outside of the simulation suite and is incorporated into everyday clinical work.
This article describes HF examples relevant to both ENT surgeons and anaesthetists, however the implementation of good HF practice is the responsibility of every clinician, department and hospital. The purpose of including good HF principles is to improve our performance with the aim of improving patient safety.
References
1. Catchpole K. Spreading human factors expertise in healthcare: Untangling the knots in people and systems. BMJ Quality and Safety 2013;22(10):793-7.
2. Just a Routine Operation.
www.youtube.com/
watch?v=JzlvgtPIof4
Last accessed October 2019.
3. The Human Factor – Learning from Gina’s story.
https://chfg.org/the-human
-factor-learning-from-ginas-story/
Last accessed October 2019.
4. Russ SJ, Rout S, Caris J, et al. The WHO surgical safety checklist: Survey of patients’ views. BMJ Quality and Safety 2014;23(11):939-46.
5. Urbach DR, Dimick JB, Haynes AB, Gawande AA. Is WHO’s surgical safety checklist being hyped? BMJ 2019;366:I4700.
6. Gorman D, Ogston S, Hussain SSM. Improvement in symptoms of obstructive sleep apnoea in children following tonsillectomy versus tonsillotomy: a systematic review and meta-analysis. Clinical otolaryngology 2017;42(2):275-82.
7. Kim JS, Kwon SH, Lee EJ, Yoon YJ. Can Intracapsular Tonsillectomy Be an Alternative to Classical Tonsillectomy? A Meta-analysis. Otolaryngology--head and neck surgery 2017;157(2):178-89.
8. Lu VM, Phan K, Oh LJ. Total intravenous versus inhalational anesthesia in endoscopic sinus surgery: A meta-analysis. Laryngoscope 2019 [Epub ahead of print].
9. Hollnagel E, Wears R, Braithwaite J. From Safety-I to Safety-II: A White Paper.
www.england.nhs.uk/signuptosafety
/wp-content/uploads/sites/16/
2015/10/safety-1-safety-2-whte-papr.pdf
Last accessed September 2019.






