Otalgia is a common presenting complaint to Ear Nose and Throat Departments. Otalgia is either primary or secondary (referred) [1]. Referred otalgia is a ‘red flag’ symptom and can be a diagnostic challenge for clinicians and radiologists as the pathology may be occult.
This article focuses on the radiological approach to referred otalgia.
To tailor an investigation for evaluation of referred otalgia we must remind ourselves of the neurology of ear pain.
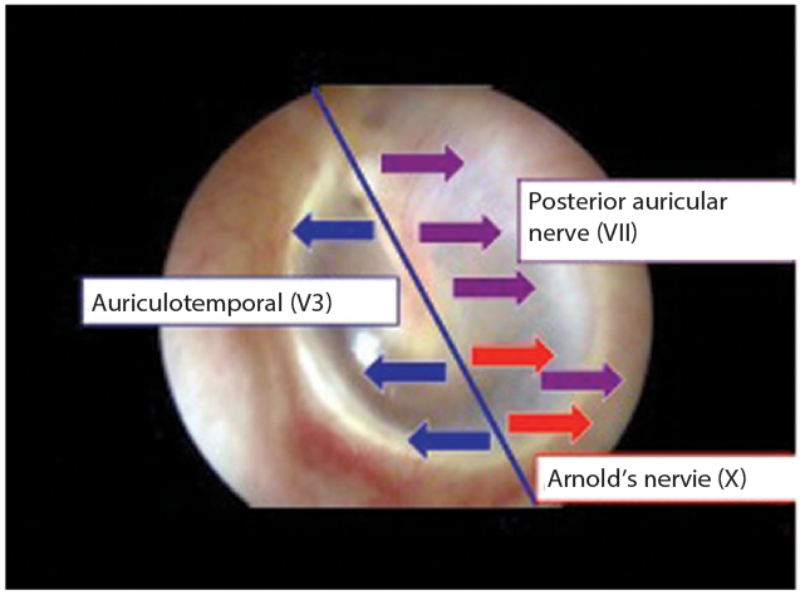
Figure 1: Innervation of the tympanic membrane.
The innervation of the tympanic membrane is complicated. Figure 1 shows a normal tympanic membrane. Using the handle of the malleus as a dividing line, the anterior half of the membrane is innervated by the auriculotemporal nerve, a branch of the trigeminal nerve (the fifth cranial nerve; CNV). The posterior half is supplied by the posterior auricular nerve, a branch of the seventh cranial nerve (CNVII), which is overlapped inferiorly by fibres of Arnolds nerve, from the vagus (tenth cranial nerve; CNX).
The entire medial surface is innervated by Jacobsen’s nerve, a branch of the glossopharyngeal nerve (ninth cranial nerve; CNIX).
The most accepted theory for referred pain is that multiple nerves converge onto a single shared nerve pathway, with the brain unable to identify the source of stimulation [1].
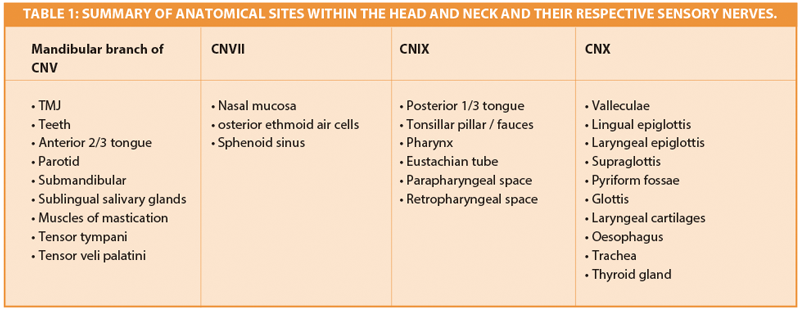
Table 1 is a condensed list of sites within the head and neck innervated by CNV, CNVII, CNIX and CNX. All are potential causes of referred otalgia.
- This is a daunting list! This may be simplified to the ‘five Ts’ – the five most common causes of referred otalgia.
- Temporomandibular joint (TMJ)
- Teeth
- Tongue
- Tonsil
- Throat
This is a well known concept in ENT. This article will focus on the most appropriate imaging for each ‘T’, illustrated by clinical cases.
Temporomandibular joint
A 45-year-old female presented with a three month history of left otalgia. Otoscopy was normal. On examination there was a palpable click of her left TMJ on opening, with deviation of the mandible to the right. The clinical findings suggested that the patient had internal derangement of the left TMJ (Figure 2).
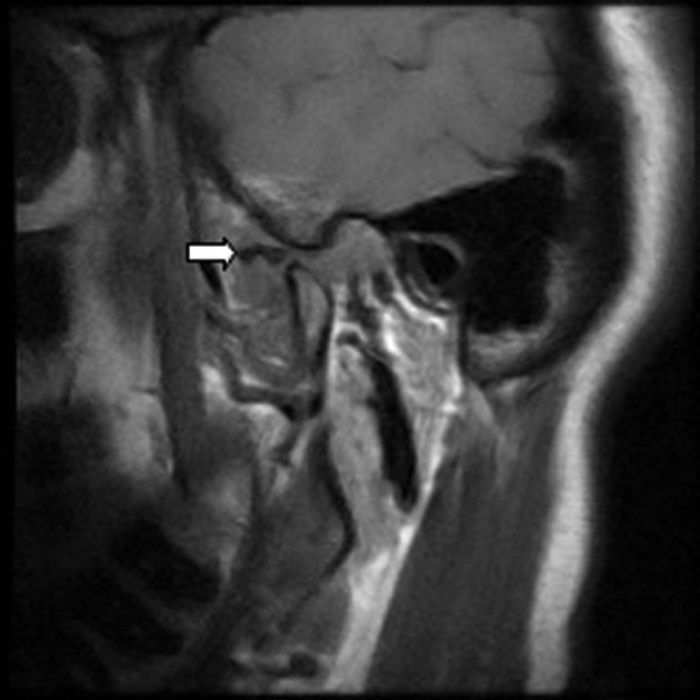
Figure 2: Sagittal T1W MRI of the left TMJ in the open mouth position showing an anteriorly displaced
meniscus (white arrow). The meniscus should be positioned between the condyle and articular eminence.
Of patients with TMJ disorders, 70-78% present with otalgia. Magnetic resonance imaging (MRI) is the preferred imaging technique for the TMJs, being performed with the mouth open and closed in order to assess meniscal displacement and recapture.
Teeth
An 81-year-old female presented with a one month history of right otalgia and a swelling of her right cheek. Otoscopy was normal.
Clinical examination excluded a dental cause, as the patient was edentulous, however an ultrasound demonstrated an abscess over the right masseter muscle. Figure 3 shows an abscess collection in the right buccal space. Figure 4 demonstrates the cause of the abscess (and otalgia) – a tooth root buried underneath the gingiva, with associated buccal bone perforation.
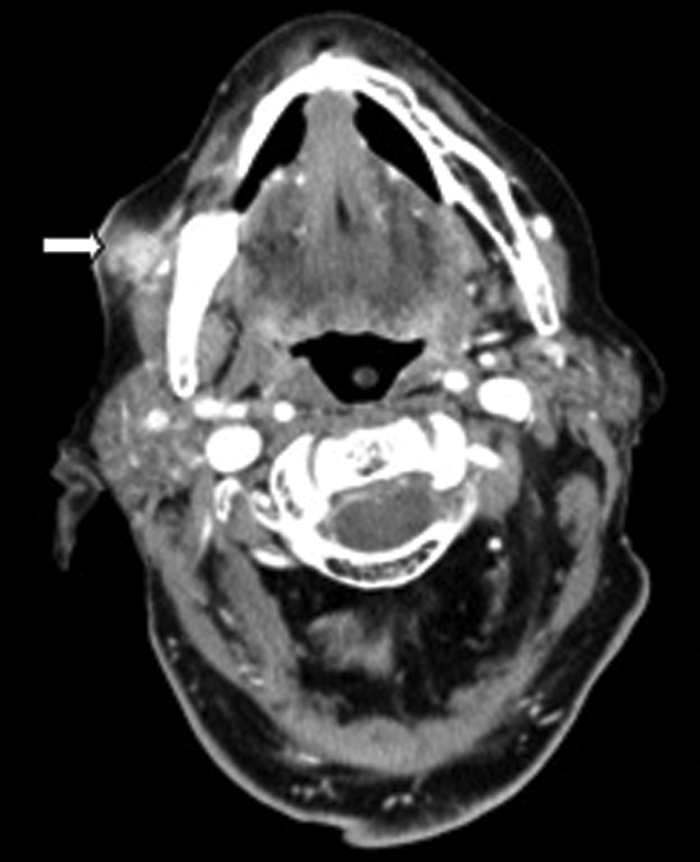
Figure 3: Contrast enhanced soft tissue axial CT demonstrating a buccal space abscess (white arrow).
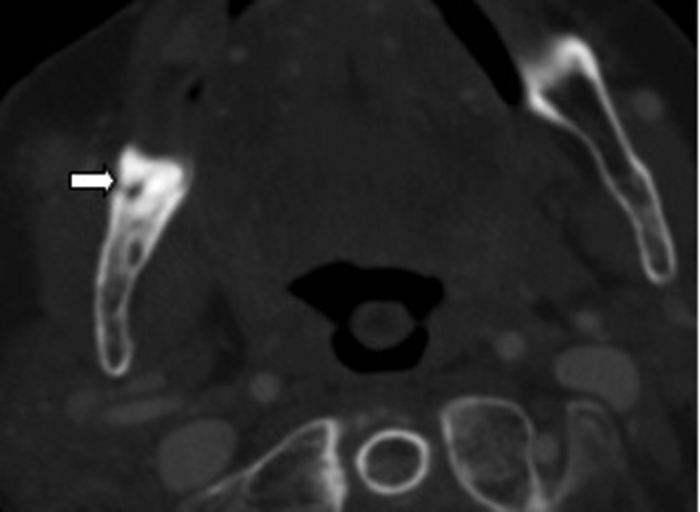
Figure 4: Bone window axial CT demonstrating a retained root (white arrow).
Dental disease, most commonly caries and impacted lower wisdom teeth, are frequent causes of referred otalgia. The imaging modality of choice in the assessment of teeth is radiography.
A commonly used radiograph is the orthopantotomogram (OPT). An OPT is a horseshoe shaped tomographic slice of both jaws, which can be useful in the assessment of caries, periodontal and periapical infections (Figure 5). It is a technique which is prone to positional errors and artefacts which can affect reliability of interpretation. Cone beam CT is being increasingly used in the dental profession but its use specifically for caries assessment is not recommended [2].
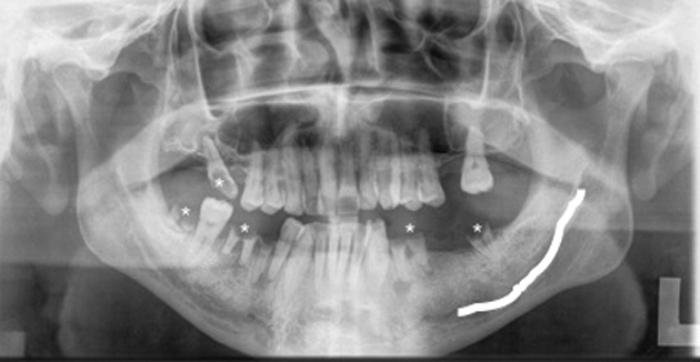
Figure 5: OPT of a different patient showing multiple carious teeth (*).
The left inferior alveolar nerve (white line) is easily identified.
Tongue
A 55-year-old female presented with a three week history of otalgia. Otoscopy was normal. Examination demonstrated an indurated erythematous mass on the left lateral border of the tongue, later confirmed as a squamous cell carcinoma.
The imaging modality of choice for the tongue is contrast enhanced MRI (Figure 6).
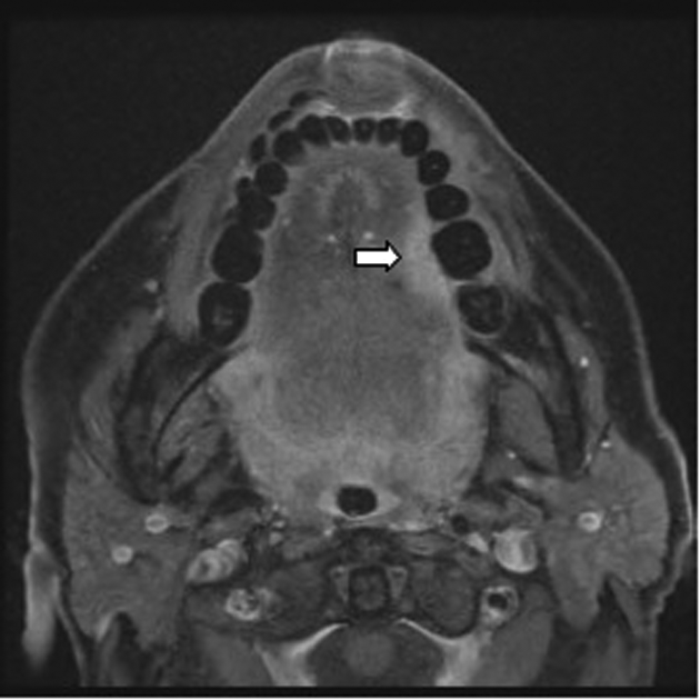
Figure 6: Post contrast T1W FAT SAT axial MRI demonstrating an enhancing
tumour on the left lateral border of tongue (white arrow).
MRI has excellent soft tissue resolution, but is not suitable for all, e.g. patients with pacemakers or cochlear implants. Contrast enhanced CT gives excellent bony and soft tissue detail but is frequently suboptimal in patients with dental restorations (Figure 7).
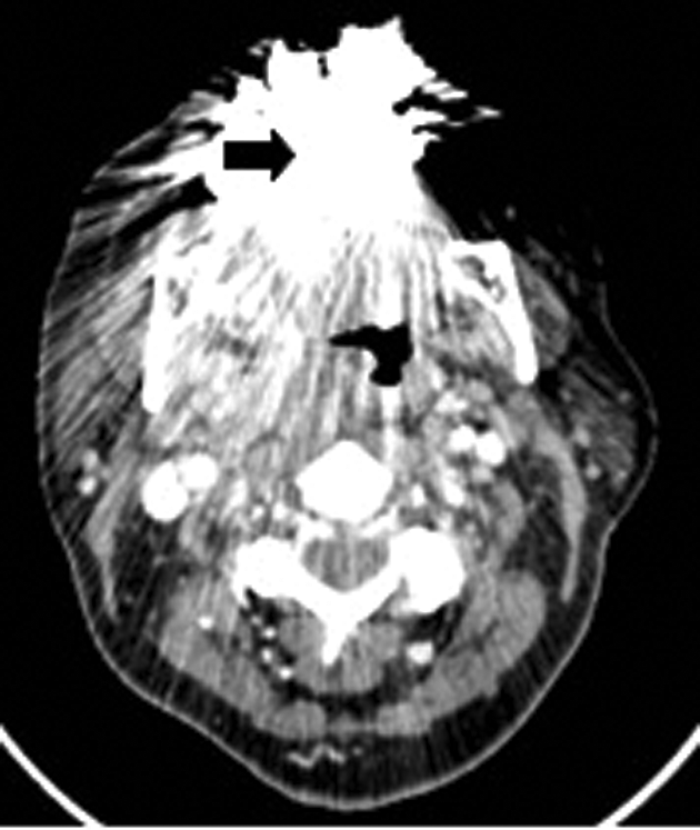
Figure 7: Contrast enhanced soft tissue axial CT demonstrating amalgam streak artefact (arrow).
Tonsil
A 17-year-old male presented with a one week history of left otalgia and general malaise. Otoscopy was normal, but there was asymmetric left tonsillar enlargement. His inflammatory markers were raised suggesting sepsis.
CT (Figure 8) demonstrated a left peritonsillar abscess. In addition Figure 9 shows the patient to have bilateral calcified stylohyoid ligaments. Pharyngitis / tonsillitis are common causes of referred otalgia. Additionally calcification of the stylohyoid ligament greater than 28mm can compress the glossopharyngeal nerve causing dysphagia, tinnitus and otalgia, a collection of symptoms termed as Eagle’s Syndrome.
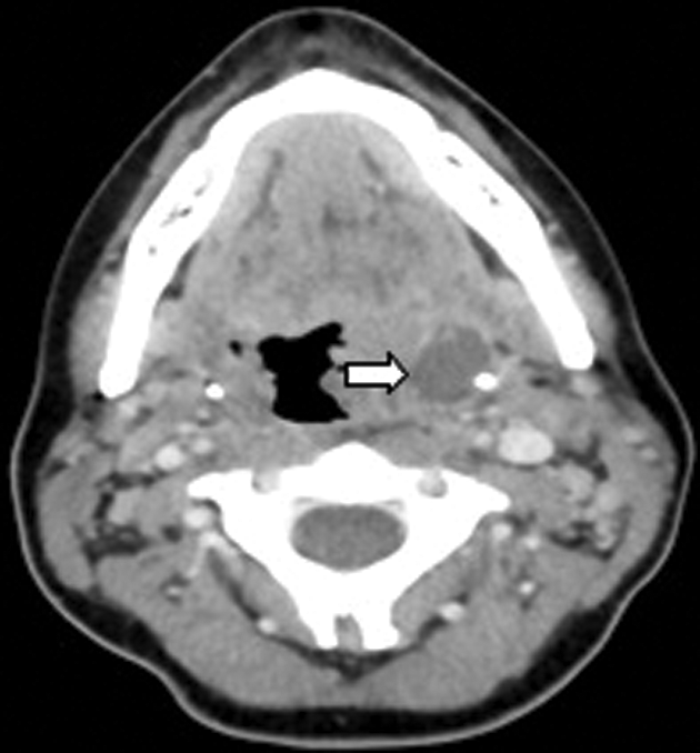
Figure 8: Contrast enhanced CT demonstrating a left peritonsillar abscess (white arrow).
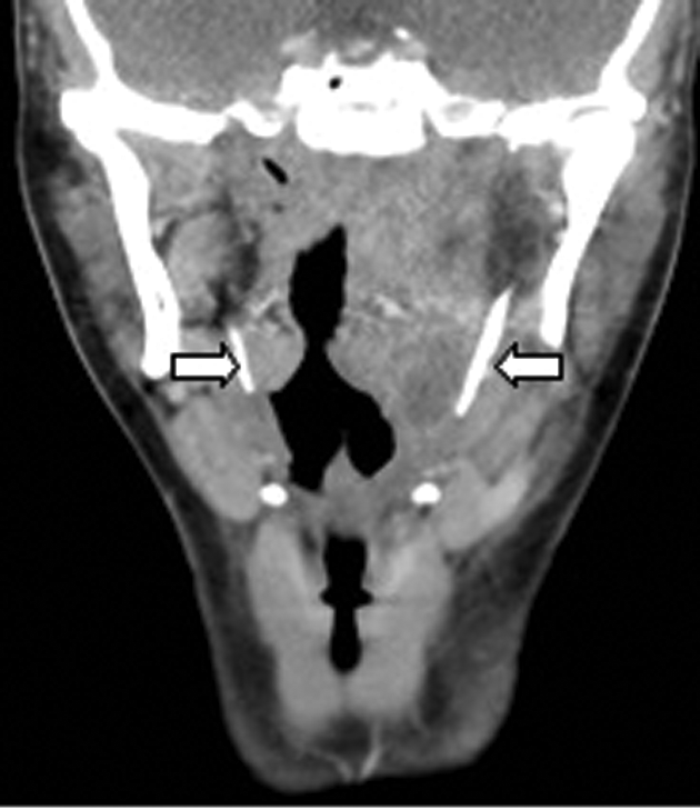
Figure 9: Coronal contrast enhanced CT of the same patient demonstrating
bilateral calcified stylohoid ligaments (white arrows).
The imaging modality of choice of the palatine tonsil and oropharynx in an acute setting is CT. Although MRI may offer superior soft tissue information, it takes longer and its use is limited in an acutely unwell patient who cannot keep still.
Throat
A 47-year-old male presented with right-sided otalgia. Otoscopy was normal. Five years previously he had chemoradiotherapy treatment for squamous cell carcinoma of the right hypopharynx. There was mucosal irregularity of the right pyriform sinus. CT demonstrated a small recurrence in the pyriform fossa (Figure 10). CT is the imaging method of choice for the larynx and hypopharynx. MRI is useful in assessment of thyroid cartilage, however it is sensitive to respiratory motion.
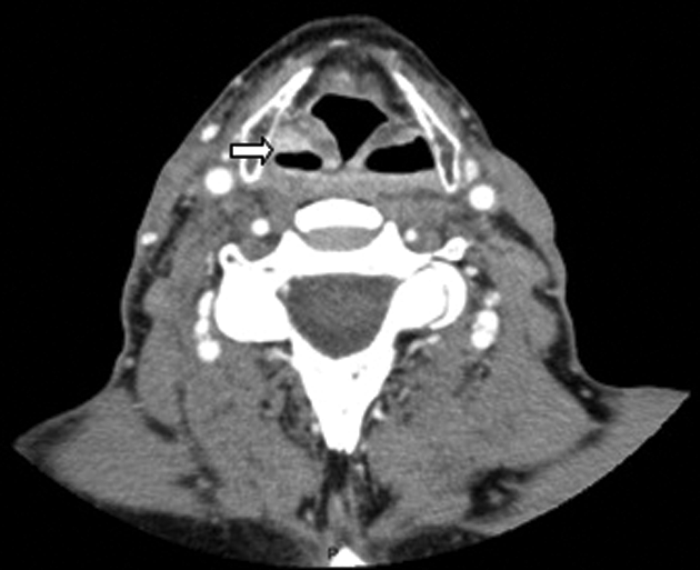
Figure 10: Contrast enhanced soft tissue axial CT demonstrating a small enhancing
squamous cell carcinoma recurrence within the right pyriform fossa (white arrow).
Conclusion
Referred otalgia is a red flag symptom. Clinicians and radiologists should be aware of the five Ts and tailor the imaging requests according to where the clinical suspicion lies.
Acknowledgements
Mr Sandeep Berry, Consultant ENT Surgeon, Ysbyty Brenhinol Morgannwg / Royal Glamorgan Hospital, Wales, UK.
References
1. Chen RC, Khorsandi AS, Shatzkes DR, Holliday RA. The radiology of referred otalgia. AJNR Am J Neuroradiol 2009;30;1817-23.
2. Wright EF. Referred craniofacial pain patterns in patients with temporomandibular disorder. J Am Dent Assoc 2000;131:1307-15.
3. SEDENTEXCT. Radiation Protection: Cone Beam CT for dental and maxillofacial radiology. http://www.sedentexct.eu/content/
guidelines-cbct-dental-and-maxillofacial-radiology
Last accessed March 2014.
4. Horner K, Eaton KA. Selection Criteria for Dental Radiography, Third Edition. London, UK: Faculty of General Dental Practice; 2013.
Additional reading
Weissman JL. A pain in the ear: the radiology of otalgia. AJNR Am J Neuroradiol 1997;18:1641-51.
Ballantyne JC, Groves J. A synopsis of otolaryngology. Third edition. Bristol, UK; J Wright; 1978.
Declaration of Competing Interests: None declared.




