The management of unilateral vocal cord paralysis has changed in the last few years: this has largely come about as a result of improvements in technology, meaning that medialisations are quicker and easier to perform than previously. This article will provide a brief overview of current practice.
Presentation
Patients with a unilateral vocal fold paralysis (UVFP) will generally present with a breathy and quiet voice, associated with vocal fatigue. In addition, the effectiveness of the cough is reduced (causing the characteristic ‘bovine’ cough). The lack of glottic competence can also cause aspiration, particularly of liquids. It is now known that silent aspiration results in excess morbidity and mortality [1].
Historical treatment
In the past, patients would have been advised to avoid intervention for several months before deciding whether surgical intervention was warranted. In the interim, voice therapy would have been provided, but patients might have been left virtually aphonic to wait for resolution of the paralysis or compensation from the contralateral side. At that point, an Isshiki type 1 thyroplasty (medialisation laryngoplasty) might have been offered, or an injection medialisation under general anaesthetic.
Investigations
In cases in which there is no obvious precipitant (surgery to the neck or thorax), investigation should comprise cross-sectional imaging from the skull base to the diaphragm (i.e. tracing the course of the recurrent laryngeal nerve). Consideration can also be given at this point to performing electromyography (EMG). EMG can provide useful prognostic information when it is unclear as to whether the vocal fold will recover function, and hence whether one might await recovery. However, as will be shown below, early interventions are now so simple to perform that there is probably little justification for not intervening in these cases – it can be argued that this significantly reduces the role of EMG.
Vocal fold medialisation injection (injection laryngoplasty) under local anaesthetic
The advent of high-quality distal chip endoscopes has dramatically improved the ability of clinicians to achieve outstanding views of the larynx with the very familiar technique of nasal endoscopy. This means that transcutaneous injections can easily be performed by a surgeon, with an assistant undertaking the endoscopy.
Why would a patient wish to have a vocal fold medialisation injection under local anaesthetic? Several reasons present themselves:
- Patients may well recently have had surgery (thyroidectomy, neck dissection, oesophageal surgery), and many of this group will be reluctant to contemplate a return to the operating theatre; the option of a quick injection in the outpatient clinic is a very attractive one.
- Patients can have immediate treatment at the time of presentation; this is particularly useful for patients who are receiving palliative care, who wish to have a rapid restoration of voice (and swallow) for the final few weeks or months of their lives.
- When performing injections in the awake patient, the exact degree of medialisation can be monitored – in this way, it is possible to be very precise in judging the amount of filler material needed to achieve good glottic closure. In addition, the improvement in voice quality can also be assessed in real time.
Injection technique
There are virtually no absolute contraindications to medialisation injection in the clinic. It is our experience (over 400 injections) that if a patient will tolerate nasal endoscopy, they will easily tolerate injection medialisation. Transcutaneous injection is generally preferred (as opposed to transoral); after injection of local anaesthetic into the airway (sometimes supplemented with pre-procedure nebulised lidocaine), one of three different approaches can be used:
Trans-thyrohyoid
Approaching the vocal folds from above gives an excellent view of the tip of the needle as it enters the upper surface of the vocal fold (Figures 1-2).
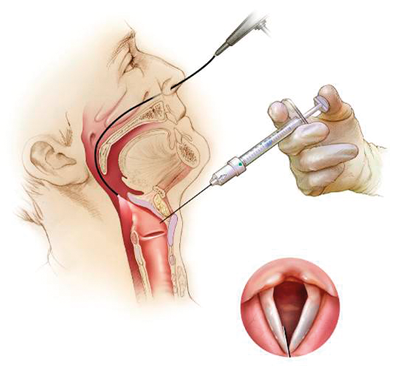
Figure 1. Thyrohyoid approach for percutaneous medialisation injection.
(Diagram used with permission of Merz Pharma.).
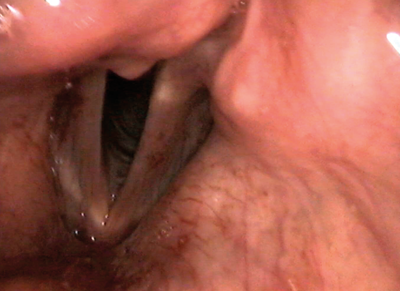
a.
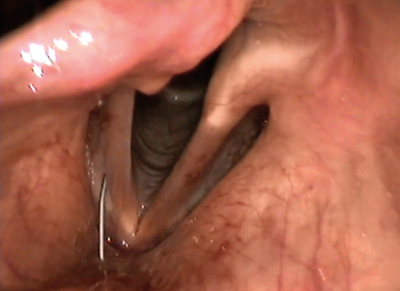
b.
c.
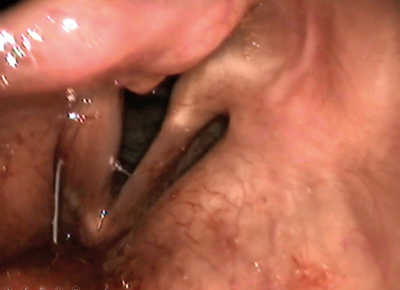
Figure 2. Endoscopic view of medialisation injection via thyrohyoid approach;
note the progressive bulking of the right vocal fold as the material is injected.
Trans-cricothyroid
In cases in which the thyroid notch is difficult to palpate (as is often seen in female patients), the cricothyroid approach brings the needle into the subglottis and approaches the paralysed vocal fold from below (Figures 3-4).
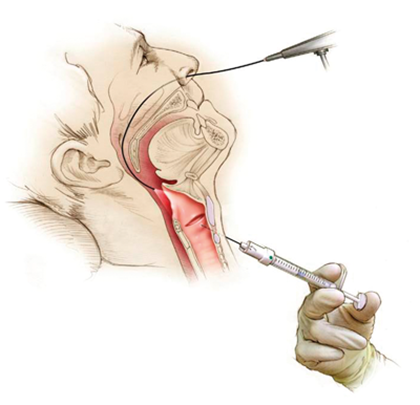
Figure 3. Cricothyroid approach for percutaneous medialisation injection.
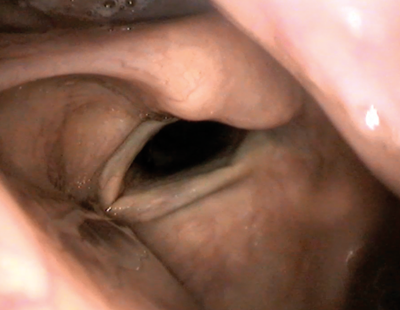
a.
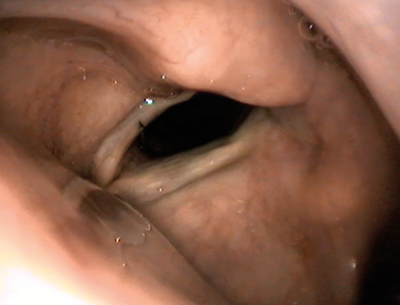
b.
c.
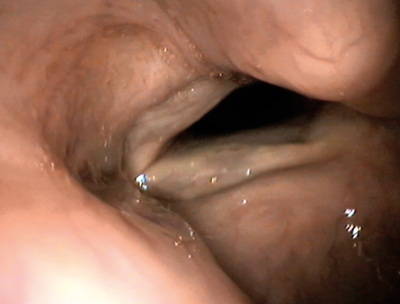
Figure 4. Endoscopic view of medialisation injection via cricothyroid approach.
Trans-thyroid cartilage
This technique is rarely required, and can be difficult if the thyroid cartilage is calcified (Figure 5).
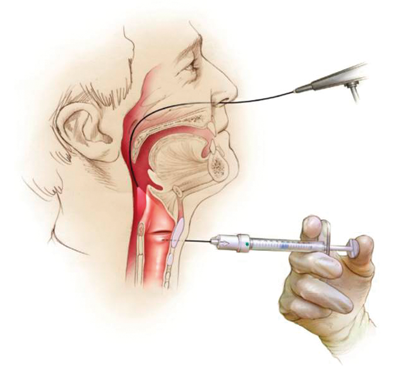
Figure 5. Trans-thyroid approach for percutaneous medialisation injection.
Benefits of early injections
The benefits to patients in terms of an early restoration of voice (and swallow) are clear; but in addition, it appears that early injection can reduce the likelihood of thyroplasty being required in future: in other words, a single, early injection may be the only intervention required [2-5].
Further treatment
If a patient has had an injection and the voice deteriorates, a repeat injection is a perfectly reasonable option. In the longer term, an Isshiki type 1 thyroplasty (medialisation laryngoplasty) can be offered, with or without an arytenoid repositioning procedure.
Reinnervation techniques (described elsewhere in this edition of the magazine) are showing promising results; the long-term outcomes of trials are eagerly awaited.
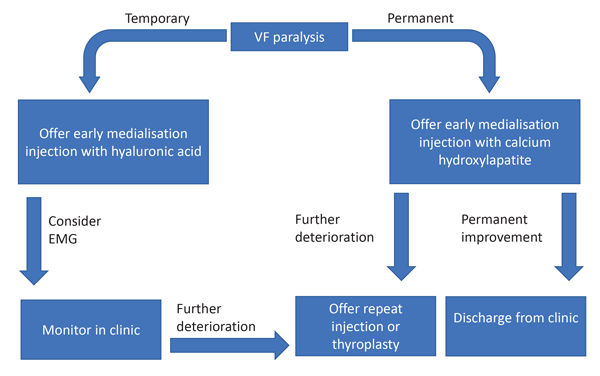
Figure 6. Suggested protocol for management of patients with UVFP.
Summary
Vocal fold medialisation injection under local anaesthetic is transforming our management of vocal fold paralysis. Our proposed algorithm for managing patients with UVFP is shown below (Figure 6). Early intervention is becoming the norm, with little justification for a prolonged ‘watch and wait’ policy.
Key points
-
Paradigms are shifting in managing VF paralysis
-
With easy-to-perform LA injections, it is probably not acceptable to ‘watch and wait’ for several months if the patient requires a rapid improvement
-
Consider early injection
-
EMG may be appropriate for patients keen to avoid early intervention.
References
1. Nouraei SAR, Allen J, Kaddour H, et al. Vocal palsy increases the risk of lower respiratory tract infection in low-risk, low-morbidity patients undergoing thyroidectomy for benign disease: A big data analysis. Clin Otolaryngol 2017;42(6):1259-66.
2. AlghonaimY, Roskies M, Kost K, Young J. Evaluating the timing of injection laryngoplasty for vocal fold paralysis in an attempt to avoid future type 1 thyroplasty. J Otolaryngol Head Neck Surg 2013;42(1):24.
3. Fang T-J, Pei Y-C, Li H-Y, Wong AMK, Chiang H-C. Glottal gap as an early predictor for permanent laryngoplasty in unilateral vocal fold paralysis. Laryngoscope 2014;124:2125-2130.
4. Friedman AD, Burns JA, Heaton JT, Zeitels SM. Early versus late injection medialization for unilateral vocal cord paralysis. Laryngoscope 2010;120(10):2042-6.
5. Vila PM, Bhatt NK, Paniello RC. Early-injection laryngoplasty may lower risk of thyroplasty: A systematic review and meta-analysis. Laryngoscope 2018; . [Epub ahead of print] doi: 10.1002/lary.26894.
6. Snyder SK, Angelos P, Carty SE, et al. Injection of bulking agents for laryngoplasty. Surgery 2018;163(1):6-8.