Global Health
Overcoming barriers to ear health in remote WA: partnerships and mobile care
Earbus Foundation delivers culturally safe, mobile ear healthcare to Aboriginal children across remote Western Australia, bridging access gaps. Otitis media, or middle ear disease, is highly prevalent in Aboriginal children in Australia [1]. Studies have shown that otitis media can...
Soundscapes of Zimbabwe: healing a nation one ear at a time
We hear about the life, vision and legacy of Dr Clemence Chidziva — the surgeon transforming ear and hearing care into a new wonder of Zimbabwe. Dr Clemence Chidziva. Tucked in the heart of Southern Africa, landlocked and bordered by...
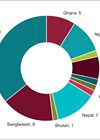
Expanding access to cochlear implants in India: a government-funded journey towards inclusive hearing healthcare
India’s state-funded cochlear implant programmes are transforming hearing care, improving access for children and adults across socioeconomic divides. India boasts a demographic landscape where a substantial portion of its population comprises children, and they play a pivotal role in shaping...
The Malawi Hearing Project
Rachael Collins, ENT trainee in the UK, and Mwanaisha Jauza Phiri, audiologist in Malawi, explore the challenges and innovations in delivering ear and hearing care (EHC) across Malawi. The Malawi Hearing Project, a partnership between QECH and Cambridge Global Health...
Observations and ruminations - a week of collaboration and learning in Ghana
A week of surgical exchange in Ghana reveals the power of collaboration, resilience and mutual learning in advancing global ENT care. Isabelle JM Williams. Isabelle’s perspective It was a Saturday lunchtime at Heathrow airport, terminal 3. Professor David Howard, Miss...
Hearing ‘aid’ for Ukraine
Hearing Aid Recycling (HAR) has partnered with Ukraine’s Vidchui organisation to deliver 1000 hearing aids to those affected by war. This collaboration provides essential support for military personnel and civilians suffering from hearing loss, highlighting the power of global solidarity...
Developing ENT services in Zambia
Lufunda Lukama and Matthew Clark. Lufunda Lukama is an ENT surgeon in Zambia. In a country of 19.6 million, he is one of five such specialists. It is not difficult to see the problem that he, and the country as...
Empowering hearing rehabilitation professionals in Sub-Saharan Africa and Asia
The Hearing Healthcare Alliance empowers professionals across Africa and Asia through comprehensive training programmes, improving local hearing rehabilitation services. According to the World Health Organization (WHO), approximately 430 million people worldwide require rehabilitation for disabling hearing loss [1]. This number...
Helping provide hearing happiness in Malawi
Children with hearing loss in low-income countries face many obstacles. UK-trained audiologist Chikondi Kuthyola shares her story and Malawi’s strides in cochlear implantation. Malawi is one of the poorest countries in the world. In developing countries, deaf children and adolescents...
ENT and audiology in the Land of a Thousand Hills
Rwanda is a beautiful country known as the ‘Land of a Thousand Hills’. It is located in the Great Rift Valley in East Africa and shares borders with Uganda, Tanzania, Burundi, and the Democratic Republic of Congo, all offering direct...
Cochlear implant care for deaf children in Côte d’Ivoire
Deafness is a global public health problem. More than 1.5 billion people (nearly 20% of the global population) live with hearing loss, and 430 million of them have disabling hearing loss, including 34 million children. In sub-Saharan Africa, nearly eight...
Re-establishing ENT services in Liberia after three decades
Liberia is a country located on the West African coast bordered by Guinea, Sierra Leone and the Ivory Coast. Founded in 1821, it is Africa’s oldest modern republic and was established on land acquired for freed US slaves by the...