We are delighted to publish a further update on the use of the technique for vocal fold lateralisation in neonates from Laszlo Rovo and Shahram Madani, who have previously informed us of this new technique [1]. These cases are rare but very challenging to deal with and the authors describe their own experience with this novel instrument.
The most common causes for bilateral vocal cord paralysis (BVCP) in children, especially in neonates, are idiopathic, iatrogenic and neurological [2]. The management of these patients associated with stridor and respiratory distress could be a ‘watch and wait’ policy or, due to severity, urgent tracheostomy is often required, which has its known care issues as well as psychological and physical side-effects [4,5].
The endolaryngeal thread guide instrument (ETGI; Mega Kft, Szeged, Hungary megakft@megakft.com) enabled us to perform endoscopic arytenoid abduction lateropexies (EAAL) in this age group as well. This has been shown to be a safe and effective treatment of vocal cord immobility [2].
Materials and methods
Patients
Four newborns with congenital BVCP who had already been admitted to the perinatal intensive care unit (PICU) immediately after birth due to severe stridor and inspiratory dyspnoea, were chosen. As part of the preoperative process, neonatological and neurological examinations and laryngological investigations were performed in four neonates on the fourth, fifth, fifth, and 27th day of life respectively, with a purpose of doing a surgery simultaneously. The miniaturised ETGI was used in the small glottis size and the thin soft tissue layer over the larynx. For exploration of neonatal larynx, the neonatal Miller laryngoscope or a Macintosh Baby laryngoscope was used.
Surgical technique
Operations were performed under general anaesthesia via total intravenous anaesthesia and high-frequency supraglottic jet ventilation with continuous, strict monitoring of saturation and end-tidal CO2 and readiness for possible intubation.
The procedure started with direct endoscopic examination of the upper and lower airways to the level of the distal trachea with a rigid 0 ̊ and 30 ̊ endoscope. A decision on unilateral, left-sided EAAL was taken during the same session and followed immediately after preparation, as follows:
“The mean total surgical time was 17 minutes, with an average of six minutes spent on the lateralisation.”
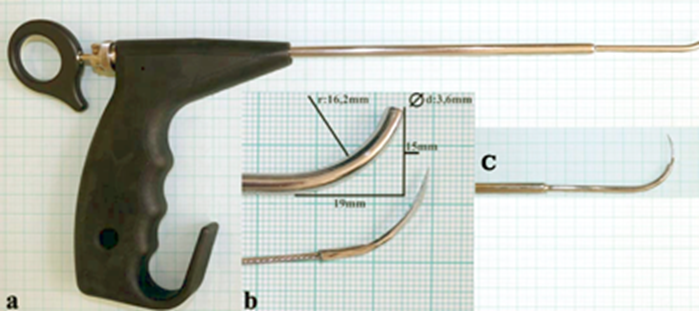
Figure 1. Endolaryngeal thread guide instrument.
a) Handel, stem-pipe, and curved blade in pushed-out position (stem-pipe and blade designed for infants).
b & c) Stem-pipe and blade designed for infants.
As described in our earlier publication [3], after disinfection of the laryngeal mucosa, the ETGI (see Figure 1) was led through the laryngoscope to the glottic level. The mobile arytenoid cartilage was tilted backward and upward with the end of the instrument (see Figures 2 and 3). The built-in, curved blade was then pushed through, under the vocal process, and out to the surface of the neck. A non-absorbable suture thread was (0-Prolene; Ethicon, Somerville, NJ) passed through the eye at the tip of the blade by an assistant surgeon. The doubled-over thread was pulled back with the blade, into the laryngeal cavity.
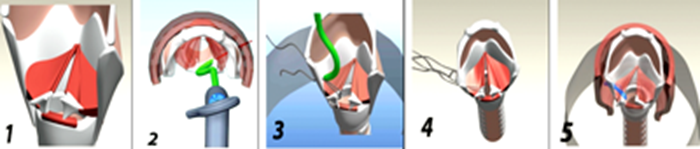
Figure 2. Principle of endoscopic arytenoid abduction lateropexy
1) ETGI is placed under the arytenoid cartilage and, at the same time, the arytenoid cartilage is lateralised to its maximum abduction position and then the blade is pushed out.
2) The suture thread is passed through the eye of the blade.
3) The blade of the instrument is pushed in and then placed over arytenoid cartilage then pushed out of larynx.
4) The suture loop was cut.
5) A knot was then tied in each thread to develop two secure sutures.
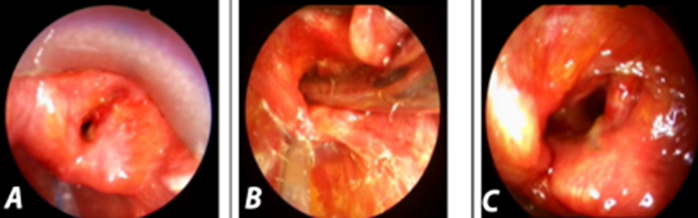
Figure 3. Intraoperative photos: left side EAAL
A) Preoperative glottis picture with severe stridor.
B) Insertion of the ETGI and performing the procedure.
C) Post- operation picture.
The blade was pushed out with the thread above the vocal process to the outer surface of the neck. The assistant surgeon then cut the double-folded thread to remove it from the blade’s eye. The blade was then pulled back into the laryngeal cavity, and the ETGI could be removed from the larynx. A small skin incision was then created to withdraw the ends of the thread by a Jansen hook to the surface of the sternohyoid muscle. The corresponding ends were knotted above it (see Figure 4) [3].
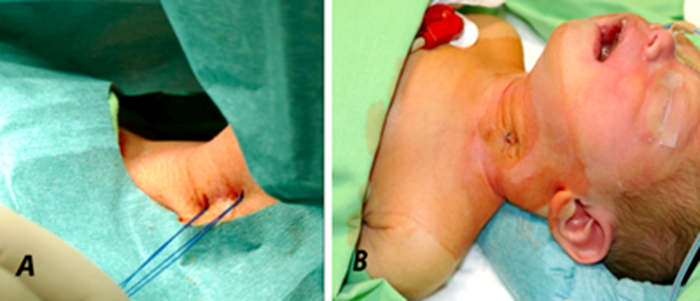
Figure 4.
A) The double thread place and tightened.
B) The double suture hidden under skin and skin closed with one simple suture.
The total operation time (from the introduction of the ETGI until its final removal) was recorded. At the end of the surgery, the babies remained intubated for three to seven days with an uncuffed tracheal tube (inner diameter [ID] = 3 and 3.5mm; Portex siliconised polyvinyl chloride oral/nasal uncuffed tracheal tube; Smiths Medical, Plymouth, MN).
The size of the endotracheal tube was chosen by age-and weight-based formula according to the advice of the anaesthesiologist [3]. Intravenous antibiotic (amoxicillin/clavulanic acid, 25mg/5mg/kg for 12 hours) was administered for four days, and methylprednisolone (4mg/kg) was administered for seven days. On the day of extubation, the patients were given a steroid bolus (see Figure 5).

Figure 5. Extubation on seventh postoperative day. Lateralised left vocal cord, wide glottis with normal breathing.
Nasogastric feeding was used for all patients while they were intubated. The postoperative management took place in the paediatric intensive care unit (PICU) in each case.
Follow-up
The functional outcomes of the surgery in terms of breathing, voice, swallowing, and overall satisfaction were evaluated by the quality of life (QOL) questionnaire of the Lausanne team [4]. Regular endoscopic examinations under general anaesthesia using a rigid 0 ̊ and 30 ̊ endoscope were performed. Body weight gain, length growth, and swallowing difficulty were systematically registered by the parents [2]. The following acoustic parameters were recorded in this study: mean pitch, jitter, shimmer, and harmonics-to-noise ratio.
“It is a one-step quick and easy procedure, which can be performed with low surgical stress, even in the first days of life.”
Results
The mean total surgical time was 17 minutes, with an average of six minutes spent on the lateralisation. No major perioperative or postoperative complications occurred. Extubation was considered safe on the fifth, seventh, third, and seventh postoperative day in the four patients, respectively (see Figure 5). In the case of one of the infant, extubation was attempted on the fourth postoperative day, but due to significant edema of the laryngeal mucosa, the intubation had to be prolonged by three days. All patients were able to tolerate a normal oral diet with no restriction in one- to-three days post-extubation. There was a significant improvement of QOL scores pre and postoperatively. Partial regeneration of vocal cord movements was observed in two of four cases. Lateralisation sutures were not removed in any of the cases.
Conclusion
It is a one-step quick and easy procedure, which can be performed with low surgical stress, even in the first days of life. The airway can be maintained without the risk of any permanent damage to voice production and swallowing function. This is a unique and new innovation in order to be able to perform EAAL and there is no other instrument like it.
References
1. Rovo L, Madani S. Endolaryngeal thread guide instrument (ETGI). ENT & Audiology News 2013;22(4):132‑134.
2. Madani S, Bach A, Matievics V, et al. A New Solution for Neonatal Bilateral Vocal Cord Paralysis: Endoscopic Arytenoid Abduction Lateropexy. The Laryngoscope 2017;127:1608-14.
3. Rovo L, Madani S, Sztano B, et al. A new thread guide instrument for endoscopic arytenoid lateropexy. The Laryngoscope 2010;120:2002-7.
4. Szakacs L, Sztano B, Matievics V, et al. A comparison between transoral glottis-widening techniques for bilateral vocal fold immobility. The Laryngoscope 2015;125:2522-9.
5. Sandhu GS, Nouraei SAR, Rovo L, et al. Bilateral impaired vocal cord mobility. In: Sandhu GS, Nouraei SAR, eds. Laryngeal and Tracheobronchial Stenosis. San Diego, CA: Plural Publishing; 2016:195-227.





