Philippa James and Lucy Shiels explain the development of the ‘Autism Listening Clinics’, highlighting a recommended clinical approach for audiologists, the importance of remote microphone technology and sharing some wonderful caregiver experiences.
Auditory challenges in autistic children
Autism spectrum disorder (ASD) is a complex neurodevelopmental condition that generally affects communication and socialisation. In recent years, the number of children diagnosed with ASD has increased and is now estimated to be one in 57 in the UK [1]. As such, paediatric audiologists often work with families who have either recently had a child diagnosed with ASD or are currently undergoing investigations into a possible diagnosis. The audiologist’s involvement with these patients typically ends with the ruling out of a peripheral hearing loss as a potential contributing factor to the child’s symptomatology. However, autistic children commonly present with complex auditory challenges that could be identified and managed by audiologists who move beyond basic audiometry.
“Autistic children experience middle ear infections and otitis-related complications associated with conductive hearing loss and grommet insertion at a higher incidence compared to their age-related neurotypical peers”
Atypical sensory processing, including that of the auditory system, is a core characteristic of ASD. Although debated, currently there are no conclusive findings supporting an increased risk of sensorineural hearing loss in autistic children [2]. However, autistic children experience middle ear infections and otitis-related complications associated with conductive hearing loss and grommet insertion at a higher incidence compared to their age-related neurotypical peers [3]. Additionally, it is well established that auditory filtering – that is, the ability to hear, function and respond to auditory information in the presence of noise, is one of the most common sensory issues affecting autistic children [4]. There is a substantial amount of evidence documenting atypical processing of auditory information on clinical behavioural assessments such as speech in noise and dichotic integration tests and electrophysiological tests directly assessing neural function e.g. ABR, and cortical auditory evoked potentials. Why is this important? In the real world, listening difficulties have been linked to academic underachievement [4], can impact attention and general behaviour, and likely exacerbate the communication challenges central to an ASD diagnosis.
Audiologists have the skillset and opportunity to play an important role in the detection and management of listening difficulties that can directly impact other features of ASD, such as a speech and language delay. However, a streamlined clinical approach to achieving this is lacking.
Developing a clinical model for assessing listening challenges in autistic children
In collaboration with Sonova AG, research teams at the University of Melbourne, University of North Texas and Hearts for Hearing in Oklahoma have been working on the development of an efficient and approachable audiologic test battery, sensitive to the auditory challenges commonly reported by autistic children. ‘Autism Listening Clinics’ were set up at each of the three sites and an extensive test battery was administered to patients which assessed hearing acuity, middle ear status, functional listening skills, and cognitive abilities including auditory memory and attention. A collection of multisite data has recently been analysed to document the auditory functioning of 71 autistic, school-aged children with normal sound detection thresholds. The data was processed to inform test selection for a streamlined assessment battery.
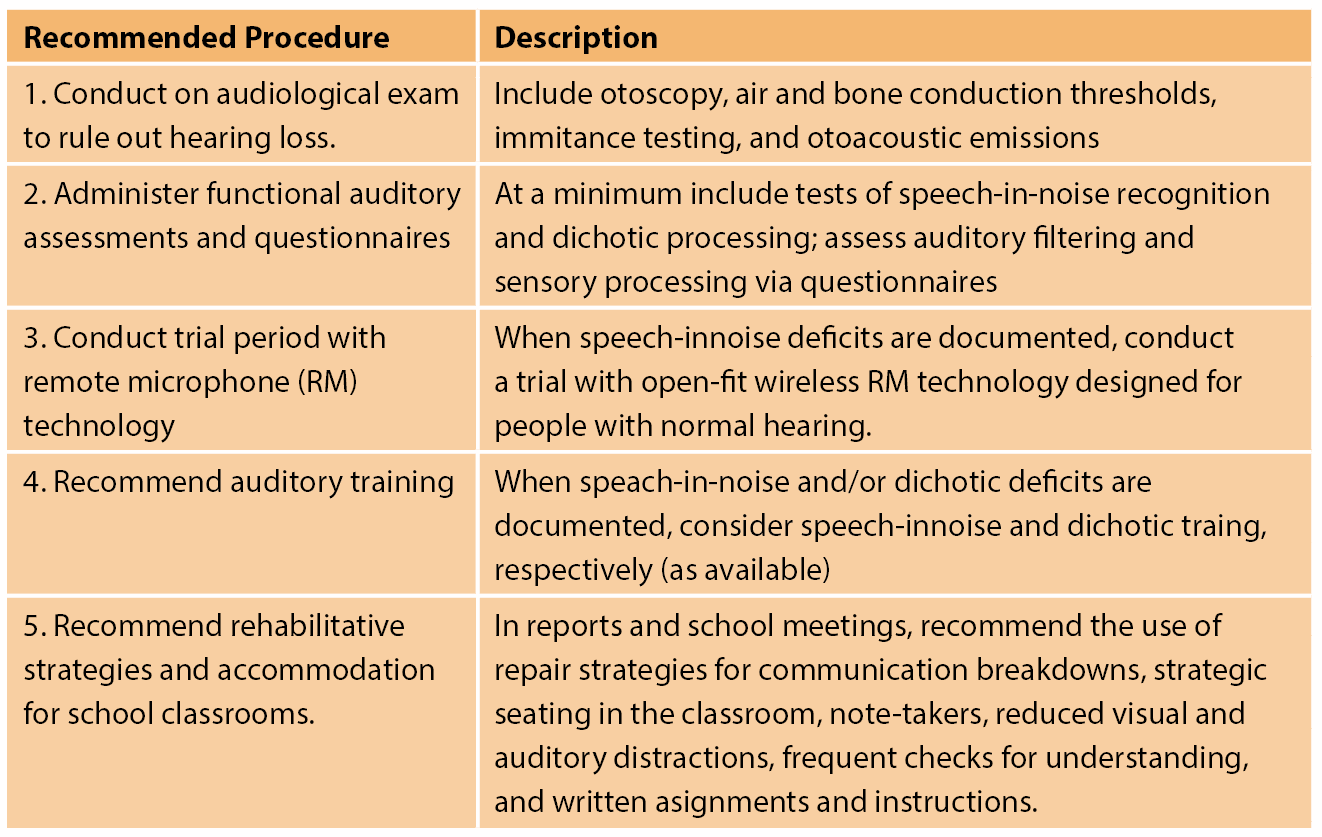
Table 1. Recommended Approach to Access and Manage Auditory Deficit in Children with Autism Spectrum Disorder.
Most patients (86%) showed poorer than expected performance on at least one auditory task, despite all having normal hearing acuity, average cognitive ability (FSIQ), and most demonstrating enhanced auditory memory abilities. Participants with ASD performed significantly worse than expected compared to a theoretical neurotypical population on four out of eight clinical domains: auditory filtering via a sensory processing questionnaire, auditory attention, speech discrimination-in-noise and dichotic integration. Performance on the auditory and sensory measures were not correlated with variations in the cognitive status of our participants or their attention abilities. The latter finding suggests concentration issues do not sufficiently explain listening deficits in this population. Based on these results, Table 1 summarises a recommended clinical approach for audiologists working with autistic, school-aged children [5].
The findings of this initial analysis further highlight the importance of going beyond the audiogram when assessing autistic children.

Philippa James and a patient of the Autism Listening Clinic, the University of Melbourne.
Management of listening challenges using remote microphone technology
There is now a strong evidence base for the use of remote microphone technology as a management strategy for auditory filtering concerns in autistic children. Recent research has demonstrated many positive results from device utilisation in school settings, including improved speech perception in noise, reduced classroom listening challenges and reduced listening-related stress. Our research aims to extend these findings in larger groups of school-aged autistic students as well as document other ‘real-world’ benefits provided to children utilising this technology across a range of settings.
“There is now a strong evidence base for the use of remote microphone technology as a management strategy for auditory filtering concerns in autistic children”
Every autistic child presents uniquely, and we are witnessing a diverse range of additional benefits from our six-week device trials. In busy public settings, parents commonly find the devices are useful for enhancing communication, providing subtle social coaching at a distance and reducing the likelihood of meltdowns from sensory overload. For younger children, many have also used the devices as a vital tool to ensure safety awareness, e.g. near busy roads.
This range of benefits is further demonstrated in stories from the caregivers of some of our patients:
Taliah – 11 years old
“Taliah has struggled with sensory processing disorder and auditory overload in a very extreme way, at times resulting in her becoming unresponsive. The Roger devices have provided a means for Taliah to remain calm and focused, reducing the incidence of these episodes.
Within the school setting, Taliah is now able to hear the teacher, focus and understand instructions. This has improved her ability to participate within the classroom. Taliah has also had less auditory overload issues as she has been able to hear clear instructions with minimal impact from background noise.
When out in public, Taliah can hear her parents, allowing her to engage in conversations as well as improving her safety, as Taliah can now hear and respond to important instructions e.g. when crossing a road or in a busy car park.
We are so grateful to have found the Roger devices and for the benefits that they have afforded us.”
Nick – six years old
“Nick has been using the device and the teacher still says it makes such a difference. He is able to give encouragement, redirection and remain a calm voice as he knows Nick can hear what he is saying. The teacher also says it is a clear indicator of behaviour and frustration change when he takes it out. It provides him seconds-worth of warning before they can expect Nick to run out of the classroom which, after running away nine times from the classroom from mid-March to end of April, is vital information for safety reasons. Thank you so much for bringing this to the community.”
Conclusion
Listening difficulties are common and debilitating in autistic children, and it is our job as audiologists to detect and manage these auditory challenges. The families we work with have shown great interest in having their children’s auditory skills assessed and are appreciative and relieved to have practical management options offered that address their real-world concerns. Using the findings from our multisite analysis, we have streamlined our clinical protocol to focus on the most prevalent auditory deficits seen in autistic children and are excited to assist other clinics in learning how to better support this wonderful community.
References
1. Roman-Urrestarazu A, van Kessel R, Allison C, et al. Association of Race/Ethnicity and Social Disadvantage With Autism Prevalence in 7 Million School Children in England. JAMA Pediatrics 2021;175(6):e210054.
2. Beers AN, McBoyle M, Kakande E, et al. Autism and peripheral hearing loss: a systematic review. Int J Pediatr Otorhinolaryngol 2014;78(1):96-101.
3. Ackerman S, Reilly B, Bernier R. Tympanostomy Tube Placement in Children With Autism. Journal of Developmental & Behavioral Pediatrics 2012;33(3).
4. Ashburner J, Ziviani J, Rodger S. Sensory processing and classroom emotional, behavioral, and educational outcomes in children with autism spectrum disorder. Am J Occup Ther 2008;62(5):564-73.
5. Schafer EC, Mathews L, Dunn A. Listening Difficulties in Children with Autism Spectrum Disorder. The Hearing Journal 2021;74(4):46-7.
6. Schafer EC, Wright S, Anderson C, et al. Assistive technology evaluations: Remote-microphone technology for children with Autism Spectrum Disorder. Journal of Communication Disorders 2016;64:1-17.