Decreased sound tolerance (DST) affects a significant proportion of autistic people throughout their lifetime and, as Zachary J Williams explains, it is important that clinicians are aware of the three distinct subtypes of DST when making a diagnosis.
Autism spectrum disorder (hereafter ‘autism’) is a heterogeneous, lifelong neurodevelopmental condition characterised by difficulties with social communication, repetitive behaviours, and atypical reactions to sensory aspects of the environment.
Notably, an estimated 50-70% of autistic individuals demonstrate clinically significant decreased sound tolerance (DST, i.e. an inability to tolerate everyday sounds) at some point in their lives [1], often resulting in referrals of autistic children and adults to audiologists or other hearing health professionals. As DST in autism appears to represent multiple distinct yet often overlapping syndromes [2] (i.e. hyperacusis, misophonia, and phonophobia), it is extremely important that clinicians be aware of the differences between these conditions and feel comfortable distinguishing between them when making a diagnosis.

Hyperacusis (Figure 1) is a hearing disorder in which sound of moderate intensity is perceived as excessively loud, painful, and/or overwhelming [2]. Individuals with hyperacusis perceive everyday sounds, such as the sounds of domestic appliances or electric hand driers, as uncomfortably loud or, in some cases, physically painful. Though frequently associated with tinnitus and peripheral hearing loss in the general population, hyperacusis in autism is thought to be neurodevelopmental in nature [2], and additional signs of peripheral auditory damage are frequently absent in this population. As in cases of hyperacusis not associated with autism, audiometric testing of uncomfortable loudness levels can support the diagnosis, although this test is typically only appropriate in adolescents and adults without significant cognitive or language impairment. While there is no consensus among professionals regarding the specific criteria used to make a clinical diagnosis of hyperacusis, operational criteria used by my research group to define hyperacusis are presented in Figure 1 to assist clinicians in making this diagnosis.
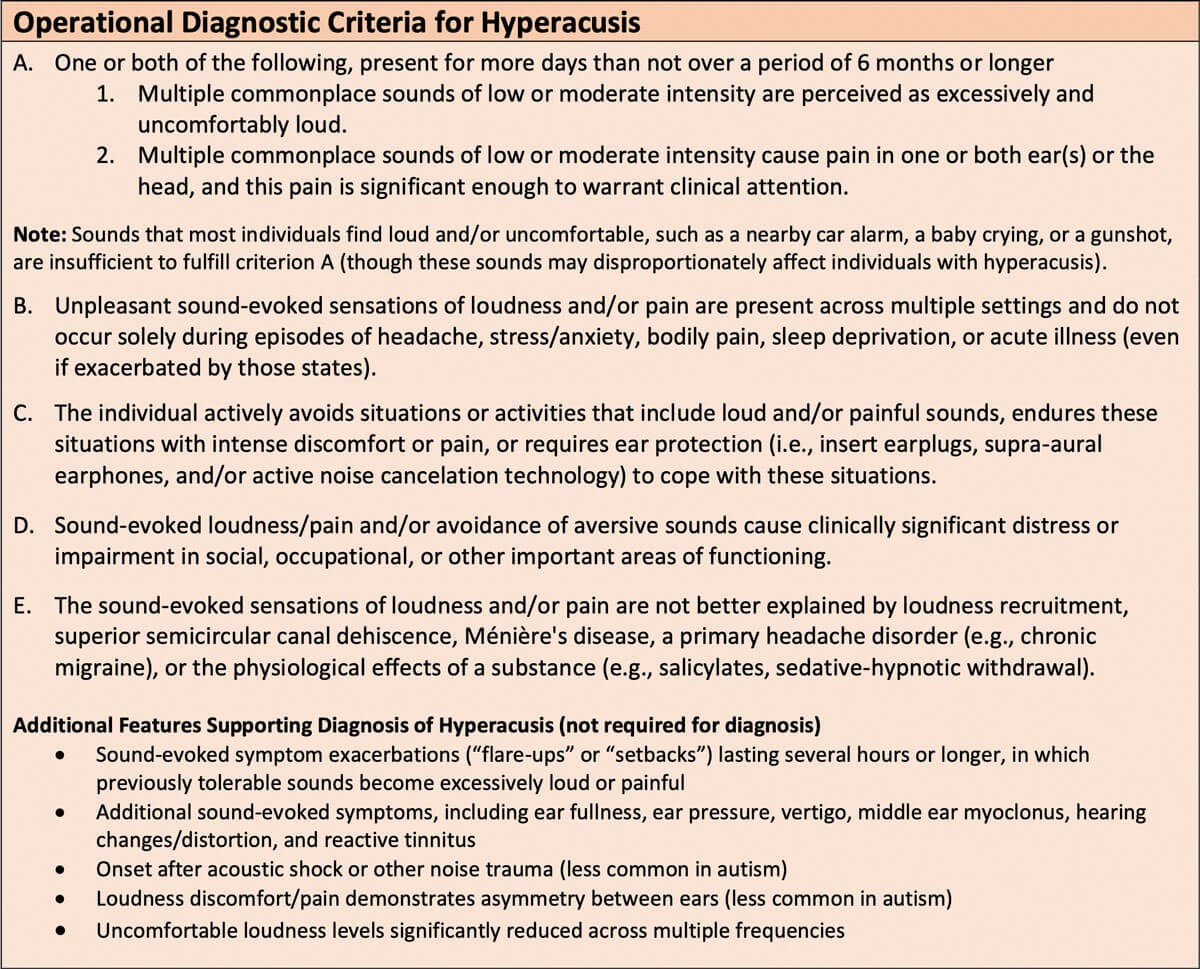

Figure 1. Operational Diagnostic Criteria for Hyperacusis. These criteria are used in an ongoing research study at Vanderbilt University Medical Center to standardise the clinical diagnosis of hyperacusis. Criteria A–E must all be met for a diagnosis to be given. This diagnosis of hyperacusis subsumes both “loudness hyperacusis” (criterion A1) and “pain hyperacusis” (criterion A2), particularly given the unclear distinction between the two subtypes in terms of underlying pathophysiology. For billing purposes, ICD-10-CM code H93.233 (“Hyperacusis, bilateral”) can be used.
Misophonia (Figure 2) is a newly-described condition in which individuals have excessive and inappropriate emotional responses to specific ‘trigger’ sounds (e.g. chewing, tapping, and sniffling), even when those sounds are not loud [2]. Anger, extreme irritation, disgust, and anxiety are the most common emotions, though some individuals may experience rage [3]. Misophonic triggers may evoke a ‘fight or flight’ response, including nonspecific physical symptoms such as muscle tension, increased heartrate, and sweating.
“Though frequently associated with tinnitus and peripheral hearing loss in the general population, hyperacusis in autism is thought to be neurodevelopmental in nature”
Unlike in hyperacusis, in which the acoustic properties of a sound (i.e. intensity, frequency, and duration) strongly predict that sound’s aversiveness, misophonic reactions are heavily context-dependent and may be diminished or absent if individuals with misophonia make the triggering sound(s) themselves [4]. Furthermore, despite large individual differences in specific trigger noises, reactions to those trigger noises, and degree of context-dependence, the majority of individuals with misophonia report that they are triggered at least to some degree by oro-nasal or throat sounds (e.g. chewing, crunching, sniffling, slurping, breathing, coughing, or throat-clearing).

Figure 2. Operational Diagnostic Criteria for Misophonia. Criteria are modified from the 2020 Revised Amsterdam Criteria [4], incorporating information from the 2021 consensus definition of misophonia [3]. Criteria A–F must all be met for a diagnosis to be given. These criteria differ from the Revised Amsterdam Criteria insofar as (a) oro-nasal sounds are not required for diagnosis and (b) misophonia can be diagnosed regardless of other psychiatric or neurodevelopmental conditions, provided that all diagnostic criteria are met. Although misophonia is not formally recognised within systems of medical billing, we suggest that the diagnosis be captured under the ICD-10-CM code H93.299 (“Other abnormal auditory perceptions, unspecified ear”).
A recent expert consensus paper proposed a definition of misophonia for use in clinical and research settings, although concrete diagnostic criteria were not specified [3]. To further support clinicians in making a diagnosis of misophonia, operational research criteria (adapted from the consensus definition [3] and the earlier ‘Revised Amsterdam Criteria’ for misophonia [4]) are provided in Figure 2.
Although the word ‘phonophobia’ has been used to refer to multiple symptoms and conditions within the medical literature (e.g. hyperacusis, episodic DST associated with headaches, and loudness disturbance due to facial nerve damage) the term here is used to refer to a marked fear or anxiety about specific sounds or situations in which a person might encounter unpleasant sounds [2]. In other words, phonophobia refers to a specific phobia of sound, as defined within the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5) [5] and its upcoming text revision (Figure 3). Phonophobia can be circumscribed to very specific sounds or generalised to all sounds with specific qualities (e.g. loud sounds, high-pitched sounds, sudden/unexpected sounds, or sounds associated with a feared object/situation). However, in all cases, the diagnosis is only appropriate if the phobic sound/situation almost always provokes fear and/or anxiety and this fear/anxiety is out of proportion to the danger posed by the specific object/situation.

Figure 3. Operational Diagnostic Criteria for Phonophobia. Criteria are slightly modified from the DSM-5 criteria for specific phobia [5], with additional information regarding the qualifier of fear out of proportion to the circumstances and the ability for ear protection use to qualify for the “avoidance” criterion. Note that for billing purposes, phonophobia should be coded using ICD-10-CM code F40.298 (“Other specified phobia”).
Notably, phonophobia can develop secondary to other DST conditions such as hyperacusis or misophonia. However, in cases where feared sounds result in significant pain, auditory discomfort, or other physical symptoms, an additional diagnosis of phonophobia should be reserved for individuals who experience fear and anxiety to a much greater degree than would be expected for an individual with their same level of hyperacusis/misophonia symptoms. In particularly severe cases of hyperacusis, in which certain sounds may cause extreme pain that persists for multiple days after exposure, fear and avoidance of the aversive sounds is arguably not excessive or irrational, and phonophobia should only be diagnosed if an individual demonstrates the same marked fear of sounds that are not known to greatly exacerbate their hyperacusis symptoms.
“Although hyperacusis, misophonia, and phonophobia are all present in the autistic population, there is a notable lack of evidence-based options for diagnosis and treatment of these prevalent and impairing conditions”
Although hyperacusis, misophonia, and phonophobia are all present in the autistic population, there is a notable lack of evidence-based options for diagnosis and treatment of these prevalent and impairing conditions, particularly in young children and individuals with significant cognitive or language impairments. Nevertheless, even with limited access to a patient’s internal experiences, knowledgeable clinicians may be able to make a clear distinction between different subtypes of DST based on consideration of the sounds the patient finds aversive, the degree to which context modulates their reactions, and the presence of observable fear or anxiety in certain situations (see Figures 1-3).
With regards to management, strategies should be individualised to the patient’s and family’s needs and can include modalities such as behavioural or cognitive-behavioural therapy (often with an exposure/habituation component), occupational therapy, sound generators, amplification, medications, use of ear protection in certain situations, and environmental modifications. Though there is insufficient evidence to strongly support any of these interventions for DST in autism, the treatment of this common symptom remains an area of great clinical need. Thus, additional basic and clinical research is desperately needed on DST in autism and other populations to improve the lives of the millions of individuals who experience these often-disabling sound sensitivity syndromes..
References
1. Williams ZJ, Suzman E, Woynaroski TG. Prevalence of decreased sound tolerance (hyperacusis) in individuals with autism spectrum disorder: A meta-analysis. Ear Hear 2021;42(5):1137-50.
2. Williams ZJ, He JL, Cascio CJ, Woynaroski TG. A review of decreased sound tolerance in autism: Definitions, phenomenology, and potential mechanisms. Neurosci Biobehav Rev 2021;121:1-17.
3. Swedo SE, Baguley DM, Denys D, Dixon LJ, et al. Consensus Definition of Misophonia: A Delphi Study. Frontiers in Neuroscience 2022;16:841816.
https://doi.org/10.3389/
fnins.2022.841816.
4. Jager I, de Koning P, Bost T, et al. Misophonia: Phenomenology, comorbidity and demographics in a large sample. Doering S, ed. PLOS One 2020;15(4):e0231390.
5. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders (DSM-5®). 5th ed. American Psychiatric Association Publishing; 2013.
Declaration of competing interests: ZJW has received consulting fees from Roche and Autism Speaks on projects related to autism.