Prevention and treatment of hearing loss needs to be viewed through a public health lens, but what does that look like? Kelly Reavis and colleagues explain the steps to addressing hearing healthcare from a public health perspective and why this approach is important.
According to recent Global Burden of Disease Studies, hearing loss was the fourth leading cause of years lived with disability in 2013 and 2015 [1]. Because people are living longer, there is the potential for there being upwards of 528 million adults over the age of 65 with hearing loss in the near future.
The consequences of untreated hearing loss are broad and include direct impacts on speech understanding and communication, enjoyment of music and access to environmental sounds, as well as secondary impacts related to cognitive decline, social isolation, emotional dysfunction and increased risk of mortality [2, 3]. As such, hearing loss in older adults is a major public health concern, and prevention and treatment of hearing loss should be a healthcare priority viewed through a public health lens [4].
“With increasing life expectancy comes the challenge of ageing without increasing disability.”
Unfortunately, although interventions for hearing loss are effective, the uptake of interventions to rehabilitate hearing loss in developed countries is low. Additionally, there is lack of access to hearing loss rehabilitation in developing countries. Even if intervention uptake and access were improved, the supply of hearing aids only meets 10% of the global demand [5]. Part of the problem of supply and demand is that the treatment of hearing loss traditionally falls within a medical model. Age-related hearing loss does not typically result from pathologies requiring medical (surgical/pharmaceutical) intervention and yet the hearing health care delivery model is subject to the same constraints and expenses imposed by systems designed to treat otologic trauma.
For these reasons, there is interest in developing alternative approaches to fill the unmet needs of the ageing sector worldwide. One approach is to view determinants of hearing health and barriers to hearing healthcare through a public health lens which acknowledges both individual and societal influences on the prevention of hearing loss and uptake of aural rehabilitation among ageing adults. For example, improving accessibility to hearing healthcare, as well as affordability, is a public health tenet. As such, enabling individuals to manage their deteriorating hearing through the use of various types of inexpensive hearing prostheses (e.g. low cost hearing aids and/or personal amplifiers) puts treatment into the hands of a greater number of individuals.
“Hearing loss in older adults is a major public health concern, and prevention and treatment of hearing loss should be a healthcare priority viewed through a public health lens.”
While an individual level approach is necessary in the greater context of hearing healthcare, to tackle the rising problem of hearing loss, it is also necessary to reduce behaviours that lead to hearing loss on a societal scale. Public health approaches aim to promote health and prolong life, free of disease and disability, among populations rather than individuals. Acknowledging that social and physical determinants shape the burden of hearing loss in terms of population distribution, severity and rehabilitation is critically important because this can help lead the way to developing effective population-based interventions. In turn this results in lasting population health effects.
A public health approach typically has three actionable arms: assessment, policy and assurance. Assessment is the surveillance of a population to elucidate the risk and impact of hearing loss in terms of persons, place, time and to highlight disparities. Policy seeks to leverage our understanding of the causal pathways leading to hearing loss and implementation of regulations to mitigate those risks and support healthy lifestyles. Policy also includes harnessing community partnerships to further solve hearing difficulties. Finally, assurance is the process of enforcing and evaluating policy development. Taken together, a public health approach can advance the hearing healthcare needs of populations.
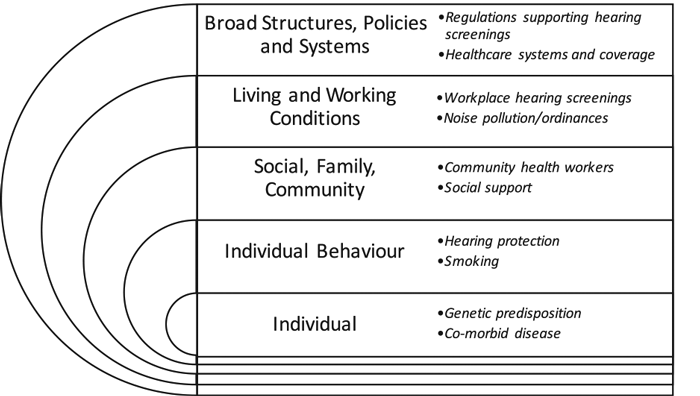
Figure 1. Adapted from the social ecological model (SEM) [6]. Within the concentric circles are the varying levels which exert influence on acquired hearing loss. Therefore, each level is an opportunity to intervene to prevent hearing loss.
Furthermore, to reduce the number of individuals with a hearing loss we need to consider the larger ecological context within which hearing loss occurs. Using a theoretical model in which all upstream factors (i.e. from the individual to society) are considered, we can identify influential factors beyond the individual or individual behaviour that contribute to the occurrence of hearing loss. Many such conceptual frameworks exist. One worth highlighting because of its simplicity and thoroughness is the Social-Ecological Model (SEM, Figure 1) [6]. The model views the health and well-being of an individual in the larger context of family, community and society (identified by the larger print in Figure 1). It acknowledges there are multiple determinants of population hearing health beyond biologic factors and innate traits and is crucial to inform a public health approach. A conceptual framework, such as the SEM, helps to explicitly define the pathways by which an influential factor can cause hearing loss or by which an intervention is expected to reduce hearing loss. Accordingly, the conceptual framework can provide the hearing healthcare field with specific elements to assess.
“Public health approaches aim to promote health and prolong life, free of disease and disability, among populations rather than individuals.”
While there are some public health practices in place for the prevention and early identification of hearing loss, they commonly only target children. Generally speaking, health efforts to stem the rising tide of ageing adults with hearing loss are few and far between despite the fact that hearing loss in this demographic is a major public health concern which warrants our attention. We propose that:
- Hearing healthcare clinicians and scientists, and the public health community raise awareness of hearing loss among the general population, policy makers and primary care providers.
- Efficacious and cost-effective strategies to detect and treat hearing loss are needed and should be applied and evaluated among adults.
- Efforts should be made to create an ongoing surveillance system that uses standardised definitions and methods to monitor hearing loss trends longitudinally.
- The causes of hearing loss beyond noise over-exposure be better defined and understood. These should include the effects of age, sex, racial groups and socioeconomic status.
- Barriers to effective interventions, such as hearing aids, should be explored and strategies to overcome such barriers must be tested.
- Finally, public health concepts and the clinician’s role in helping to achieve better hearing health among populations should be incorporated into audiology training programmes.
With increasing life expectancy comes the challenge of ageing without increasing disability. Negative impacts associated with hearing loss do not have to be synonymous with ageing. Prevention and treatment of hearing loss through a public health model, which places the focus on populations, groups and communities, may better help to serve the needs of many – as the goal in public health is to provide the maximum benefit for the largest number of people.
References
1. Wilson BS, Tucci DL, Merson MH, et al. Global hearing health care: new findings and perspectives. Lancet 2017; [Epub ahead of print] DOI: 10.1016/S0140-6736(17)31073-5.
2. Feeny D, Huguet N, McFarland BH, et al. Hearing, mobility, and pain predict mortality: a longitudinal population-based study. Journal of Clinical Epidemiology 2012;65(7):764-77.
3. Strawbridge WJ, Wallhagen MI, Shema SJ, et al. Negative consequences of hearing impairment in old age: a longitudinal analysis. Gerontologist 2000;40(3):320-6.
4. Reavis KM, Tremblay KL, Saunders G. How Can Public Health Approaches and Perspectives Advance Hearing Health Care? Ear and Hearing 2016;37(4):376-80.
5. World Health Organization. Deafness and hearing loss. 2015;
http://www.who.int/mediacentre/factsheets/fs300/en/
Last accessed 25 September 2017.
6. Institute of Medicine. Who Will Keep the Public Healthy? Educating Public Health Professionals for the 21st Century. Washington, DC; The National Academies Press; 2003.







