
Family members currently have minimal involvement in the appointment.
Image by Caitlin Grenness.
Hearing loss in older adults not only affects the patients themselves, but also their family members. This article outlines the findings of recent research into how family members are typically being involved in current audiology practice, and how audiologists might move towards a more family-centred approach to clinical practice.
Hearing impairment is highly prevalent among older adults, and can have a significant impact on their everyday lives. Communication difficulties resulting from a hearing impairment not only affect the person themselves but also their families (known as third-party disability).
A growing body of research has found that family members can experience considerable communication difficulties, psychosocial stresses, reduced intimacy in the relationship with the person with hearing impairment, and decreased quality of life [1, 2]. For this reason, it is recommended that audiologists use a family-centred care approach, where services are planned around the whole family, not just the individual client. Family-centred practice involves three key elements and associated aspects: practices that build relationships, practices that support choice and participation and technical quality (Figure 1).
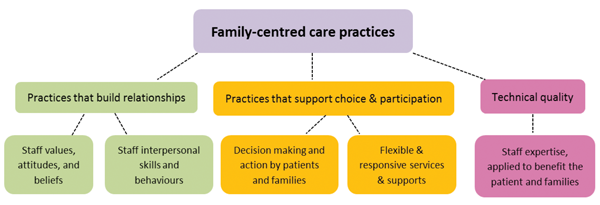
Figure 1: Family-centred care approach to clinical practice (adapted from Department of
Human Services and Department of Education and Early Childhood Development, 2011 [6]).
“A family-centred care approach is likely to improve the uptake of hearing rehabilitation and improve outcomes for people with hearing loss.”
However, little attention to date has been given to the role of family members within audiology appointments. To address this issue, a large programme of research at The University of Queensland and The University of Melbourne, Australia, (partially funded by the Australian HEARing Cooperative Research Centre) is currently investigating the following questions:
- What do patients, family members, and clinicians want?
- How are family members currently involved in hearing rehabilitation?
- How can audiologists implement family-centred care into their clinical practice?
What do patients, family members, and clinicians want?
To address the first question, interviews were conducted with older adults with hearing impairment, their family members and audiologists. The interview findings showed that all participant groups would value the involvement of family. Participants acknowledged that the role of family members in hearing rehabilitation is complex and multifaceted, but also emphasised that audiologists had a commanding opportunity to facilitate family-centred practices within hearing rehabilitation. Participants emphasised the significant role that family members play in the help-seeking process as well as in decision-making about rehabilitation.
Family member involvement was valued for establishing shared knowledge and understanding between the older adult with hearing loss, family member(s) and audiologist. Family participation in rehabilitation was also seen as a means to improve outcomes. Patients saw it as a way to verbalise family communication concerns, and use the audiologist as a sounding board and as someone who could verify these concerns. Patients and family members also emphasised the potential benefits of participating together in group rehabilitation programmes.
How are family currently involved in hearing rehabilitation?
Following this, the research team sought to investigate how family members are currently being involved in audiology appointments. Video-recorded initial audiology appointments with a family member in attendance were collected and the interaction was analysed in minute detail using a method called conversation analysis [3, 4].
The results from this study found that:
- Family members are not typically invited to join the conversation
- Despite not being invited to speak, family members displayed a strong interest in participating and sharing their experiences by attempting to enter the conversation. In particular, family members would self-select to speak by: – responding to questions from the audiologist that were directed to the patient – self-initiating expansions on patients’ turns – self-initiating questions to the audiologist
- Audiologists typically responded by shifting conversation back to the patient. In this way, the family member’s contribution to the interaction was typically brief, and they were often ‘shut out’ of the exchange between patient and audiologist.
These studies have demonstrated that while there is a desire for more family involvement in hearing rehabilitation, family members are not currently being involved in the rehabilitation process within appointments. There is thus a current gap between evidence and practice suggesting the importance of family-centred care.
How can audiologists implement family-centred care into their clinical practice?
Our findings show support for encouraging audiologists to further include family members within counselling in audiology practice. Family members can provide valuable information about the difficulties being experienced by the patient.
Further, when being actively involved in the process, family members may be more willing to engage in rehabilitative communication practices at home with the patient. While implementing family-centred care practices can be a challenge in the time-pressured clinical environment, there are effective and efficient ways that it can be achieved. Building on the results of the studies conducted to date, the research team is currently in the process of developing a family-centred care intervention to be implemented into clinical practice.
This intervention will include some useful strategies that audiologists can use to engage family members in the process. These include:
- Inviting family members to attend appointments
- Seeking and actively listening to family members’ contributions
- Responding openly and empathically to their contributions
- Using tools designed to engage family members, such as the Goal Sharing for Partners Strategy (GPS) [5] (Figure 2).
Goal Sharing for Partners Strategy

Figure 2: The Ida Institute ‘Goal Sharing for Partners Strategy’ (GPS).
(PHL: refers to person with hearing loss, CP: refers to communication partner).
These are some ways that audiologists can encourage further participation from family members during the appointment, and in doing so, include them in the patient’s ongoing hearing rehabilitation programme. Implementing a family-centred care approach is likely to improve the uptake of hearing rehabilitation and improve outcomes for people with hearing loss.
References
1. Scarinci N, Worrall L, Hickson L. Factors associated with third-party disability in spouses of older people with hearing impairment. Ear Hear 2012;33:698-708.
2. Scarinci N, Worrall L, Hickson L. The effect of hearing impairment in older people on the spouse. Int J Audiol 2008;47:141-51.
3. Ekberg K, Meyer C, Scarinci N, Grenness C, Hickson L. Family member involvement in audiology appointments with older people with hearing impairment. Int J Audiol 2015;54:70-6.
4. Ekberg K, Meyer C, Scarinci N, Grenness C, Hickson L. Disagreements between clients and family members regarding clients’ hearing and rehabilitation within audiology appointments for older adults. J Interactional Research in Communication Disorders 2014;5:217-44.
5. Preminger J, Lind C. Assisting communication partners in the setting of treatment goals: The development of the Goal-sharing for Partners Strategy. Seminars in Hearing 2012;33:53-64.
6. Department of Human Services and Department of Education and Early Childhood Development. Family-centred, person-centred organisations: a guide for managers and governance bodies to support whole-of-organisation approaches to family-centred practice. Melbourne, Australia; State Government of Victoria; 2011.
Declaration of Competing Interests: None declared.
ABOUT THE AUTHOR
Katie Ekberg is a Postdoctoral Research Fellow in the School of Health and Rehabilitation Sciences at The University of Queensland, Australia. Her research interests involve communication in client-clinician healthcare interactions, addressing psychosocial issues in healthcare consultations, patient-centred care and family-centred care. Her current research involves examining communication in audiology consultations with older clients with hearing impairment, and in paediatric hearing services.
SUMMARY
-
Family members are significantly affected by a patient’s hearing impairment.
-
Family member involvement has the potential to improve the uptake of hearing rehabilitation and improve outcomes for people with hearing loss.
-
While there is a desire for more family involvement in hearing rehabilitation, family members currently have minimal involvement within appointments.
-
There are some useful strategies audiologists can use to further engage family members in the rehabilitation process.
-
A family-centred care approach should be encouraged within audiology practice.




