Dysphagia profoundly impacts quality of life. Multidisciplinary research, like the POuCH study, aims to improve understanding, diagnosis and treatment.
We take for granted the simple joys of life – meeting over a cup of coffee, breaking bread with friends or sharing a meal with loved ones during holidays. Eating and drinking are so fundamental that their importance often escapes notice. Now imagine the discomfort of being unable to swallow or even belch. These are not trivial inconveniences; they strike at the heart of human connection and dignity.
The intersection of voice and swallow
The inevitable happens: we age. With ageing come assistive devices – wheelchairs, canes – and a growing list of diagnoses: cancer, stroke, cardiac disease. It should come as no surprise that swallowing is also affected. The challenge lies in recognising when compensatory strategies fail and dysphagia emerges.
We often detect illness through voice changes – throat clearing, weak or a wet voice. These are signals not only of dysphonia but also dysphagia. Glottic insufficiency – a leaky valve – contributes to breathy voice and aspiration risk, underscoring the interconnected nature of voice and swallowing.
Is swallowing just ‘plumbing’? We address the laryngeal valve, but the oesophagus has its own challenges. The upper and lower oesophageal sphincters must open and close appropriately. Failure may lead to regurgitation or choking; excessive tone may cause dysphagia or abelchia. Symptoms lead to disorganised referral pathways, sometimes starting with otolaryngologists, gastroenterologists, foregut surgeons, pulmonologists, neurologists, respiratory therapists or speech-language pathologists. However, disorders of the aerodigestive system require a multidisciplinary approach, and diverse perspectives strengthen our understanding of cricopharyngeal muscle dysfunction (CPMD) and the lens through which we treat patients.

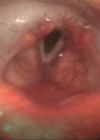
Patient undergoing simultaneous swallowing fluoroscopy with ultrasound and demonstrating a cricopharyngeal bar in order to diagnose cricopharyngeal muscle dysfunction (CPMD).
Defining cricopharyngeal muscle dysfunction (CPMD)
Using anatomic boundaries, dysphagia can be further characterised as oral (i.e. tongue), pharyngeal (i.e. hyolaryngeal complex), oesophageal (i.e. cricopharyngeus muscle, CPM) or a combination of the above (i.e. oropharyngeal or pharyngoesophageal dysphagia). The upper oesophageal sphincter (UOS) sits at the junction of the pharyngeal and oesophageal musculature where both neural input and elasticity of the CPM are protective of the larynx, especially at rest and during sleep. Afterall, the primary purpose of this high-pressure zone is to prevent backflow from the oesophagus. The opening of the UOS is thereby controlled by a variety of stimulus from the pharynx, oesophagus, larynx and central nervous system.
CPMD refers to impaired relaxation of the upper oesophageal sphincter (UOS). The cricopharyngeus muscle may exhibit hypertrophy, incomplete relaxation or failure to relax – detectable via fluoroscopy, high-resolution manometry or electromyography. The UOS regulates flow both ways – swallowing (‘north-to-south’) and reflux (‘south-to-north’). This sensorimotor complexity remains incompletely understood, yet it underscores how CPMD profoundly affects quality of life. Dysphagia evaluation focuses on both efficiency and safety. Efficiency can be trained, often by a speech language pathologist, with strengthening exercises such as the Masako manoeuvre. Safety, however, is a measure of aspiration risk, significantly impacting quality of life by dietary restrictions such as food thickener, or worse, alternative nutrition such as gastric feeding tubes (completely bypassing our sensory experience of taste and texture of food we consume).
To better understand patients with CPMD, a multicentre, international collaboration of dysphagia-focused clinicians was established in 2016 as the Prospective Outcomes in Cricopharyngeus Hypertonicity (POuCH) study. This longitudinal database includes demographic data, fluoroscopic imaging, laryngoscopy and patient-reported outcome measures (PROMs) from treated and observed patients across 15 sites worldwide.
CPMD with or without diverticula
Patients with untreated CPMD have stable symptom scores over time, unlike those with Zenker diverticulum who worsen without treatment [1]. Using validated dysphagia PROMs such as the Eating Assessment Tool (EAT-10), the POuCH working group revealed that isolated CPMD can be more symptomatic than CPMD associated with diverticula, most commonly Zenker diverticulum (ZD). Treatment for ZD is surgical. Historically, transcervical approaches such as diverticulectomy and diverticulopexy were preferred, until the 1980s when endoscopic technique was popularised. Today, endoscopic methods can be performed with a variety of instruments (e.g. laser, stapler or cautery) and techniques (e.g. flexible, rigid or submucosal resection). Moreover, the POuCH demonstrated that surgical intervention for Zenker – open or endoscopic – improved swallowing in 88% of patients by more than 50%, with two thirds achieving complete symptom resolution [2,3]. Although most patients undergo endoscopic surgery with pre- and postoperative EAT-10 assessment, open techniques demonstrate statistically significant superiority over endoscopic methods based on both raw EAT-10 scores and percent change. Importantly, symptom severity did not correlate with diverticulum size, and long-term follow-up (up to four years) affirms the reliability of surgical management [2].
What’s next?
CPMD is a confluence of both pharyngeal and oesophageal dysphagia related to both sensory feedback and motor response. Swallowing fluoroscopy is the most used diagnostic tool to confirm CPMD in patients with obstructive symptoms. However, the variability in imaging quality, number of swallows and frame rates yield poor reproducibility. Furthermore, availability of swallowing fluoroscopy limits patient access.
There is a need for novel diagnostics (and treatments) for CPMD. The Leuven Consensus has established normative metrics for pharyngeal high-resolution manometry, with promising greater diagnostic accuracy and biofeedback-driven interventions [4]. Complementary techniques – such as ultrasound-assisted tongue movement analysis – will further our understanding of swallowing physiology. Meanwhile, artificial intelligence and machine learning are poised to revolutionise assessment and lead to innovative interventions. With shared imaging data and global collaboration, the next decade could bring transformative advancements in dysphagia care.
A global call to action
The purpose of multicentre research, such as the POuCH, is to direct patient-centred care and support collaboration in order to innovate. CPMD is a poorly defined disorder that is likely underestimated worldwide. As otolaryngologists, we are uniquely positioned at the crossroads of voice and swallow to better diagnose and treat CPMD.
So, as we raise a glass to 2026, let’s commit to this: dysphagia matters. Let’s make sure our patients never lose the joy of sharing a meal.
Rebecca Howell will present on this topic at BACO 2026 in Glasgow, UK, in July.
For further information visit: www.entuk.org/baco
References
1. Randall DR, Chan R, Gomes D, Walker K. Natural History of Cricopharyngeus Muscle Dysfunction Symptomatology. Dysphagia 2022;37(4):937–45.
2. Howell R, Johnson C, Allen J, et al. Surgical Outcomes in Zenker Diverticula: A Multicenter, Prospective, Longitudinal Study. Laryngoscope 2024;134(1):97–102.
3. Schuman AD, McKeon M, Allen J, et al. Dysphagia Outcomes in Zenker Diverticulum: A Longitudinal POuCH Study. Laryngoscope 2026;136(2):683–7.
4. Omari TI, Maclean JCF, Cock C, et al. Defining Pharyngeal and Upper Esophageal Sphincter Disorders on High-Resolution Manometry-Impedance: The Leuven Consensus. Neurogastroenterol Motil 2025:e70042.
Further reading
1. Krekeler BN, Howell RJ. Cricopharyngeus muscle dysfunction: a poorly defined disorder from diagnosis to treatment. Eur Arch Otorhinolaryngol 2024;281(9):4519–27.
2. Kahrilas PJ, Dodds WJ, Hogan WJ. Dysfunction of the belch reflex. Gastroenterology 1987;93(4):818–22.
Declaration of competing interests: RJH has been reimbursed by Cook Medical and C2DX as a consultant and honorarium.