Emma Watts, a West Midlands ENT Registrar and Digital Fellow, gives a witty and concise recollection of ENT training during COVID, and predicts how hybrid learning may be here to stay.
*A zorse is the offspring of a zebra stallion and a horse mare.
You’re muted. Nope, still can’t hear you. Can everyone see my slides?
This formed the soundtrack to a generation following the outbreak of COVID-19. Redeployment, virtual clinics and postponed elective operating stifled training opportunities [1]. In immediate response, Health Education West Midlands (HEWM) developed a new digital training platform to facilitate surgical education in the UK.
This postgraduate virtual learning environment (PGVLE) combined a learning management system (Moodle™) with an integrated virtual classroom (BigBlueButton), allowing surgical trainees to host and record training days and display key learning resources whilst collating and analysing feedback. As we transition to the new normal, we reflect on lessons learned and the new role of hybrid training.
Trainee experience
Feedback collated from regional training days demonstrate the platform was well received. Anonymous polling proved a popular function through encouraging interaction and providing opportunity for trainees and tutors to check understanding. All sessions were recorded and archived, allowing trainees to review content at their convenience. The PGVLE recognises trainees as busy adult learners, allowing control over their own education by facilitating access to expert-generated content available anytime and anywhere. Opportunities for personalisation allows learners to self-select or revisit relevant videos and proceed at their own pace.
This accessibility allowed our trainees to prioritise their surgical experience. As elective operating slowly returned, the age-old adage ‘see one, do one, teach one’ was no longer sustainable; now, every practical training opportunity needed to be maximalised. Recorded lectures have since become a cornerstone, allowing trainees to learn at their own pace and prioritise irreplicable surgical experience. Through the PGVLE, trainees have access to a fantastic online 3D anatomy resource to supplement their preoperative learning. Most ENT trainees are digitally native, raised alongside technology, with expectations that it should play increasingly meaningful roles throughout their learning. Arguably, COVID-19 has merely accelerated our assimilation of virtual technology.
Trainer perspective
Technology-enhanced learning must be accessible for both learner and resource developer, especially if they are clinicians. In my role as digital teaching fellow, I found creating learning resources to be an intuitive process. The opportunity to review archived training day programmes encouraged us to reflect on their content. Working collaboratively, we reviewed the new curriculum and divided it into manageable topics for each training day. These topics are set to rotate on a four-year cycle, preventing content repetition and encouraging outcome-based education through targeted learning objectives.Lecturers quickly grew confident in using the platform. Initial technical glitches have gradually been ironed out in subsequent updates.
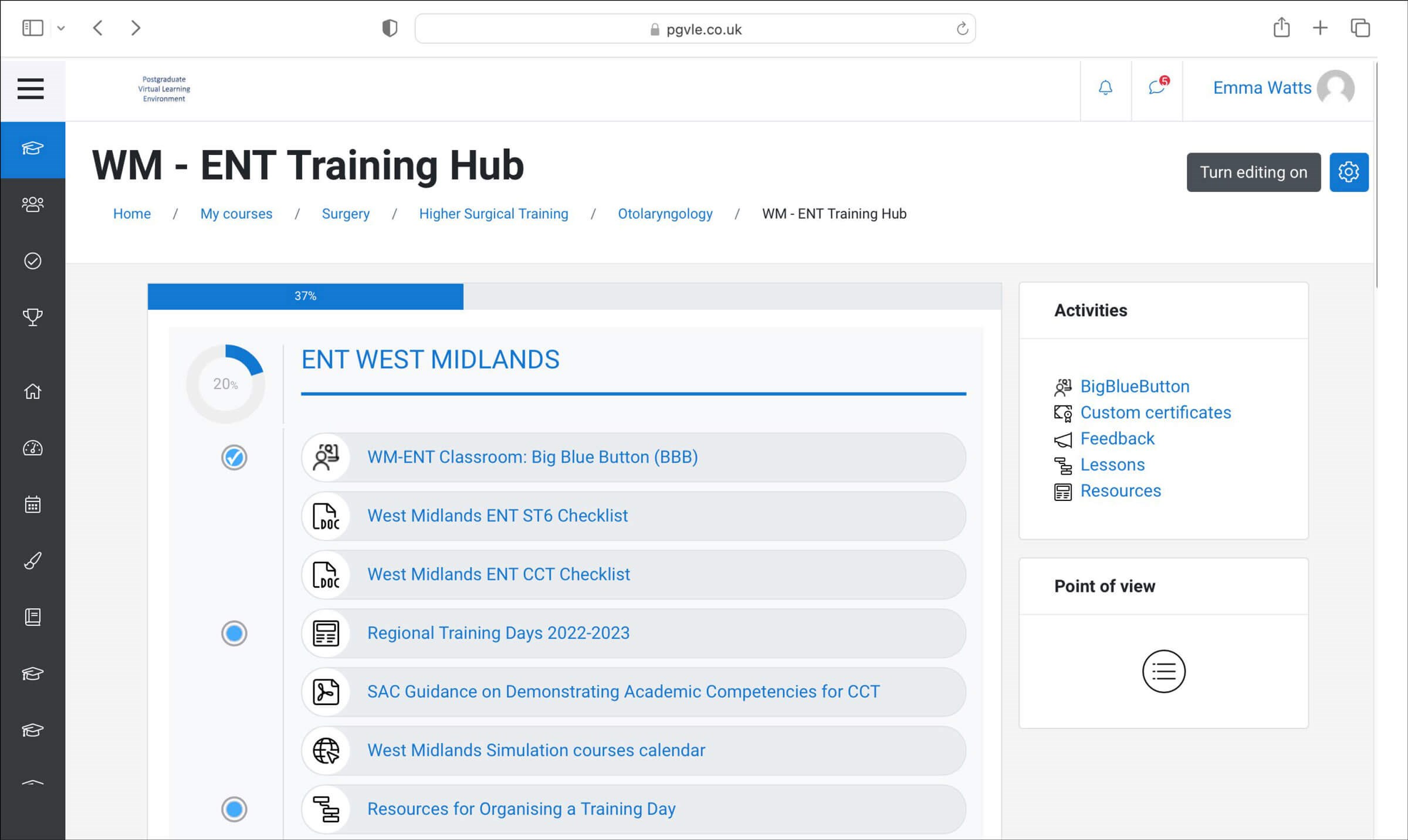
Lecturers are no longer confined to the hospital hosting the training day, as technology allows subspecialty experts to teach remotely. Reusable learning objects (RLOs) embrace recycling of existing digital resources to facilitate learning; this improves the quality of video content and limits work duplication. Thus, technology-enhanced learning provides both practical and financially astute solutions for increased accessibility [2].
"The PGVLE recognises trainees as busy adult learners, allowing control over their own education by facilitating access to expert-generated content available anytime and anywhere"
Some trainers found online teaching isolating. Previously vibrant trainees were replaced by a static sea of minimally responsive blank squares. Despite best efforts to engage trainees in active discussion using the ‘chat’ function, communication felt stilted and artificial. This limited networking opportunities, making it particularly difficult to get to know trainees entering the cohort.
Are face-to-face lectures integral to ENT training?
With social distancing measures lifted, surgical education approaches a crossroad. Should we return to tried and tested traditional teaching methods? Or embrace the learning toolset derived during the coronavirus pandemic?
Despite the excitement generated by emerging technologies, eLearning should not be considered a panacea for medical education. Although online learning offers greater flexibility, Vaona et al. report no difference in medical professionals’ behaviour or patient outcomes when comparing online and traditional teaching methods [3]. However, online learning can leave students drowning in too many resources, with tutors forced to transition to become ‘co-creators’.
Our deanery boasts incredible access to a simulation lab and multiple cadaveric dissection courses. Whilst eLearning can supplement training, it could never replace invaluable practical tuition. Our annual mock viva course utilises real patients and role models, allowing trainees to hone communication skills and examination technique. Small group activity endorses collaboration and fosters non-technical skills of leadership and cooperation. Although online ‘chat’ functions and discussion boards try to encourage collaborative learning, greater interactivity emerges from our face-to-face training days through fostering active discussion, networking and qualitative informal feedback.
Prediction for the future
eLearning carries pedagogical importance for modern surgical training and the PGVLE platform will prove pivotal for postgraduate training in the West Midlands. Gradually, we seek to accumulate a repository of lectures, add links to pre-existing resources and generate integrated MCQs to support self-directed revision. Our training cohort has discovered whilst online learning can supplement, it cannot replace face-to-face educational opportunities. Employing a flipped classroom approach [4] would allow trainees to capitalise on learning during cadaveric dissection or simulated temporal bone courses. Reviewing pre-course lecture material or instructional videos before the training session will enable a greater mastery of concepts for deeper learning engagement.
Surgical training follows an apprenticeship model, whereby skill correlates with experience. However, rare emergencies requiring time-critical responses mean experience may be impractical. For instance, ENT trainees may perform lateral canthotomy, evacuation of a neck haematoma or front of neck access with limited prior experience. Recorded demonstrations of critical emergencies could be simulated using models. Liaising with scrub teams to record the contents of ENT emergency trays could help familiarise trainees with equipment, improving communication during emergencies and enhancing interprofessional learning. Such resources require appropriate planning, evaluation and time for effective implementation. Finally, the arrival of augmented virtual reality could transform surgical education. New studies suggest it could reduce error rates and improve technical competency intraoperatively [5].
Conclusion
Adversity fosters change. Whilst the pandemic has threatened conventional training opportunities, it has also inspired transformation within medical education. Expanding upon lessons learned, we must create our own Zorse, through working towards a hybrid model of surgical education.
Hold on. Let me just check my connection.
This meeting has been ended by host.
References
1. Hope C, Reilly JJ, Griffiths G, et al. The impact of COVID-19 on surgical training: a systematic review. Tech Coloproctol 2021;25(5):505-20.
2. Ahmady S, Kallestrup P, Sadoughi MM, et al. Distance learning strategies in medical education during COVID-19: A systematic review. J Educ Health Promot 2021;10:421.
3. Vaona A, Banzi R, Kwag KH, et al. E-learning for health professionals. Cochrane Database Syst Rev 2018;1(1):CD011736.
4. Nouri J. The flipped classroom: for active, effective and increased learning – especially for low achievers. Int J Educ Technol High Educ 2016;13:33.
5. Piromchai P, Avery A, Laopaiboon M, et al. Virtual reality training for improving the skills needed for performing surgery of the ear, nose or throat. Cochrane Database Syst Rev 2015;9:CD010198.