Surgeons in Bangalore share how a novel robotic approach enables scar-sparing thyroid surgery for large nodules and cancer, while reshaping global training.
Can an 8 cm benign thyroid cystic nodule be removed without a big scar in the neck? Can a well differentiated thyroid cancer be removed completely by a minimal access thyroid surgery? Yes, it can be done and we at Krishna Institute of Medical Sciences-Minimal Access Cancer Surgery (KIMS-MACS) unit in Bangalore, India, would like to share our journey of minimal access thyroid surgery.
Led by Dr Sandeep Nayak, our group has pioneered minimally invasive cancer surgery for over a decade. Our work has consistently demonstrated that laparoscopic and robotic approaches can achieve uncompromised oncological outcomes while offering faster recovery, reduced hospital stay and improved quality of life [1–3]. Within this framework, we developed a novel technique of robotic thyroidectomy – a modification of the bilateral axillo-breast approach (BABA) – using four small ports to access the thyroid gland. Our initial feasibility study was published in the International Journal of Clinical Oncology, following which we have continued to refine the technique through meticulous audits and iterative improvements [4].
To date, we have performed 183 robotic thyroidectomies using this technique, which we call RABIT – robotic axillo-breast insufflation thyroidectomy. RABIT differs from other approaches in several significant aspects. It is a single-docking technique, unlike BABA, and both lobes of the thyroid gland can be accessed without changing camera or instrument position after the first docking is done. Unlike unilateral retroauricular approaches, specimen integrity is maintained [5]. In contrast to transoral techniques, which are used to remove small thyroid lesions in a craniocaudal direction, RABIT offers the surgeon the same perspective as obtained during open thyroidectomy, albeit using robotic instrumentation with all its inherent advantages.

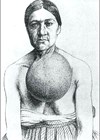
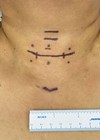
Left: Pre- and postoperative images.Right: Port sites after closure.

3D-printed silicon model for robotic simulation.
With increasing experience, we have expanded the indications to include thyroid malignancies, performing central compartment clearance and, when indicated, lateral neck dissections without compromising oncological principles. Over nine years, we have addressed enlarged thyroid glands up to 11 cm via this technique. We further combined this approach with robotic-assisted thoracoscopic surgery to excise thyroid tumours with mediastinal extension – procedures that would otherwise have required a sternotomy. We have used the same approach to address recurrent nodal disease or thyroid bed recurrence or to perform completion thyroidectomy. All thyroid operations are performed along with intraoperative nerve monitoring, with positive outcomes.
India, as a developing nation, exists in multiple timelines simultaneously. In our practice, we routinely perform both traditional open surgeries and advanced minimally invasive procedures to serve patients across diverse economic and social backgrounds. As early adopters of minimally invasive head and neck oncology in our country, we carry not only the responsibility of innovation but also the obligation to train future generations.

Robotic surgery is being increasingly adopted globally, yet standardised training remains available in only a few centres as part of super-specialty programmes. Our major training breakthrough came with the development of a 3D-printed silicone thyroid model mounted on a tracheolaryngeal framework, designed specifically for robotic training. This was made possible through collaboration with Dr Amjad Maniar, an anaesthetist, whose expertise in 3D printing brought this concept to life. The model was evaluated during a structured workshop in which 40 surgeons successfully simulated every step of robotic thyroidectomy using the RABIT technique. Silicone tubing was used to simulate blood vessels, and the pliable silicone thyroid closely mimicked tissue handling in real-life.
The model has since undergone multiple iterations, each improving its fidelity and educational value. I look forward to sharing the model for training, as I firmly believe that such cost-effective, reproducible and scalable models will play a meaningful role in democratising robotic surgical training worldwide.
Head and neck robotic surgery is a niche subspecialty with limited simulation models and highly variable training pathways influenced by local context. Model-based simulation training can bridge this gap by allowing repeated, structured practice in a safe environment. It also reduces the burden on trainers who must balance patient safety with the responsibility of teaching. Most importantly, it enables trainees to acquire procedural dexterity before operating on live patients.
I am grateful for the opportunity to present our work and look forward to your insights, suggestions and feedback.
Athira Ramakrishanan will present on this topic at BACO 2026 in Glasgow, UK, in July.
For further information visit: www.entuk.org/baco
References
1. Nayak SP, Jayaprasad K. Minimally Invasive Neck Dissection (MIND) Using Standard Laparoscopic Equipment: a Preliminary Report and Description of Technique. Indian J Surg Oncol 2017;8(2):217–21.
2. Nayak SP, Devaprasad M, Khan A. Minimally invasive neck dissection: A 3-year retrospective experience of 45 cases. J Minim Access Surg 2019;15(4):293–8.
3. Khan A, Reddy VS, Gangadhara B, et al. Robotic infraclavicular approach for minimally invasive neck dissection in head-neck cancers. J Minim Access Surg 2023;19(3):395–401.
4. Nayak SP, Sadhoo A, Gangadhara B, et al. Robotic-assisted breast-axillo insufflation thyroidectomy (RABIT): a retrospective case series of thyroid carcinoma. Int J Clin Oncol 2020;25(3):439–45.
5. Chang EHE, Kim HY, Koh YW, Chung WY. Overview of robotic thyroidectomy. Gland Surg 2017;6(3):218–28.
Declaration of competing interests: None declared.