From lived experience to PhD research, Nic Wray explores how tinnitus and hyperacusis are understood in primary care, and why listening better could improve support.
My working life has taken many turns, but becoming a researcher was never part of the plan. I spent years in busy professional environments where productivity was measured in outputs, deadlines and deliverables; research felt like a world meant for other people.
And yet, today, I am a PhD student based at the NIHR Nottingham Biomedical Research Centre (BRC), University of Nottingham, investigating how people with tinnitus and hyperacusis experience care in primary settings.
Early experiences that stayed with me
My relationship with tinnitus began long before my research career. An ear infection left me with a sound that did not fade when the infection cleared. What stayed with me was not only the noise itself, but the absence of guidance that followed. The infection was treated competently; the aftermath was not. There was no discussion of emotional impact, or how to live with persistent internal noise. That early experience planted a seed that would resurface decades later.
Fourteen years at Tinnitus UK: understanding the impact
Around the turn of the millennium, my career settled into marketing and communications, and eventually I became a chartered PR practitioner. A defining chapter was 14 years at Tinnitus UK, where I worked closely with people affected by tinnitus and sound sensitivity conditions. Through the Tinnitus UK helpline and forum, the reports we produced, the campaigns we ran and countless conversations, I heard similar stories repeated: distress countered with vague reassurance, symptoms minimised or misunderstood and long waits for specialist care. I spoke with people who were anxious, angry, exhausted or depressed as an invisible condition took over their lives.
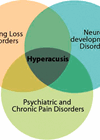
It was during this period that I came to understand hyperacusis (a reduced tolerance to everyday sounds) not only as a clinical term, but as a lived experience. Hyperacusis often co-exists with tinnitus and can be profoundly disabling. I recognised these patterns in the people I supported and, eventually, in myself. Having language for that experience fundamentally changed how I thought about sound, health and health literacy. It also became evident that there was even less support and understanding available for those living with hyperacusis.

Figure 1: The stages of my research.
These years also gave me the privilege of working alongside and learning from leading experts in the field – audiologists, clinicians, researchers and psychologists – helping to translate their knowledge into accessible information and practical support. This multidisciplinary environment exposed me to emerging research and thoughtful clinical debate, shaping how I communicated information and how I thought about care.
"Alongside standardised measures of tinnitus impact and sound sensitivity, open-ended questions allow people to describe in their own words what felt helpful, confusing or missing at that stage of care"
When reassurance is not enough
What struck me most consistently was not a lack of goodwill in healthcare, but a mismatch of expectations and understanding. General practitioners are often the first point of contact for people with tinnitus, yet training on these conditions is limited and consultation times are short. When symptoms have no clear test, cure or pharmaceutical solution, reassurance often becomes the default response. Whilst well-intentioned, and indeed part of the NICE tinnitus guidance [1], it can be experienced by patients as dismissal. Advice offered as information was received as rejection. This gap in communication frustrated me, intrigued me and ultimately pushed me toward research.
What research is trying to change
To try and change this narrative, in 2024 I stepped away from supporting people and into research, starting a PhD at NIHR Nottingham BRC, University of Nottingham. For my research project, I am exploring how GPs in the UK promote and support self-management for tinnitus and hyperacusis, how patients interpret that advice and how these interactions might be improved to support better outcomes. At its heart, this work is about listening: to patients trying to cope with life-altering symptoms and to clinicians constrained by time and resources. It is structured around four interconnected strands of work examining what happens in those early clinical encounters.
What my research project involves
The first stage of my research focuses on GPs. In a follow-up to a 2011 service evaluation [2], I am exploring how GPs currently assess and manage tinnitus and hyperacusis, their awareness and use of national guidance and referral pathways, and how they promote and support self-management strategies for the conditions via a UK-wide online survey. The survey combines structured questions with free-text responses, allowing both breadth and depth. The aim is not to judge practice, but to understand the constraints, uncertainties and competing pressures that shape care in short primary care consultations.
The next stages shift the focus to adults living with tinnitus and/or hyperacusis. I have started with an online survey asking participants to tell us about their experiences of GP consultations for tinnitus and hyperacusis, the self-management advice they received and how they understood and acted on it. Alongside standardised measures of tinnitus impact and sound sensitivity, open-ended questions allow people to describe in their own words what felt helpful, confusing or missing at that stage of care.
Following this, I will be interviewing adults living with tinnitus and hyperacusis to further explore in-depth how people make sense of their GP’s advice about self-management, how early interactions shape their journey with their conditions and how communication and support could be more effective. The theoretical framework I’ve chosen recognises that meaning is co-constructed between researcher and participant and is particularly well suited to understanding health advice, behaviour change and consultation dynamics.
Alongside these studies, I am also reviewing current literature on self-management in primary care, which provides theoretical context for the project. This review, referred to as a realist review, does not focus on whether self-management is effective – it examines how, why and for whom self-management works. It focuses on how context and mechanisms (such as time pressure, trust or validation) influence whether advice is taken up or rejected. Due to limited literature on tinnitus and hyperacusis, the review also draws upon other medically unexplained symptoms such as chronic fatigue and irritable bowel syndrome, to identify transferable insights relevant to tinnitus, hyperacusis and general practice.
Findings from the GP survey, patient survey and interviews and the realist review will be integrated using behavioural and health communication frameworks to develop an evidence-informed model of how tinnitus and hyperacusis self-management is promoted, perceived and supported in primary care.
Better research leads to better care
Ultimately, this stage of my professional journey, even with its uncertainties, endless reading lists and long days of writing and planning, feeds back into the same motivation that first drew me to the tinnitus community. Better research leads to better conversations, better understanding and better care. If we want people with tinnitus and hyperacusis to feel supported rather than dismissed, then the systems around them need careful, thoughtful scrutiny. Moving from the third sector into research has not taken me away from the real world; it has brought me closer to the point where meaningful change can begin.
The research is ongoing. If you or anyone you know is interested in more information about the different studies or would like to participate or be involved, please contact me.
References
1. National Institute for Health and Care Excellence. Tinnitus: assessment and management. NG155. 2020.
www.nice.org.uk/guidance/ng155
[Link last accessed April 2026]
2. El-Shunnar SK, Hoare DJ, Smith S, et al. Primary care for tinnitus: practice and opinion among GPs in England. J Eval Clin Pract 2011;17(4):684–92.
Declaration of competing interests: None declared.