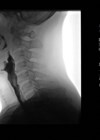
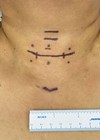
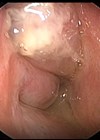
It is recognised that hearing loss and ear disease are far more common in less affluent parts of the world, and that those countries are often least able to provide treatment; so how can we prioritise care for these patients?
Low- and middle-income countries (LMIC) have a disproportionately high burden of ear diseases. Living conditions in these countries are a fertile ground for middle ear infections, especially in childhood. While most of these diseases are treatable, access to appropriate healthcare services is limited in LMIC. This leads to late detection and late intervention which then leads to complications and permanent hearing impairment and deafness, which would otherwise be prevented through timely and appropriate intervention.
Hearing impairment and deafness has now been identified as one of the leading causes of disability. Hearing loss is the most common sensory disorder in humans. Most of these cases of hearing impairment and deafness reside in LMIC. Rehabilitation of the hearing impaired has improved over the years due to the advances in technology: hearing assistive devices are now available to assist all forms and degrees of hearing impairment and deafness. The irony is that these devices are needed most in LMIC which have a high burden of disease and yet LMIC have the least ability to afford these essential devices.
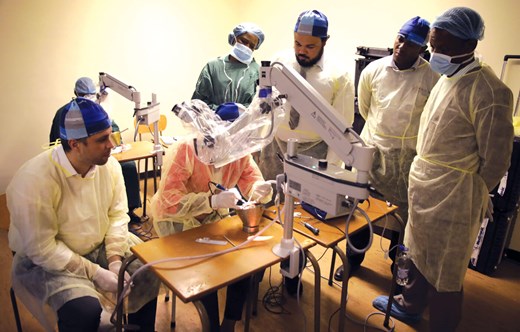
Otology training in Harare.
Competing needs for healthcare delivery in LMIC are a reality. Life-threatening infectious diseases remain rampant and endemic in LMIC. Lifestyle changes and changes in eating habits have seen an exponential rise in non-communicable diseases such as diabetes and hypertension. In addition, malignancies are also on the rise. All these life-threatening conditions mean that ear and hearing healthcare initiatives tend to take a back seat in LMIC. This calls for professionals in these fields to not only focus on service provision within their spaces but to also embark on effective advocacy to get a slice of the ever-constrained healthcare budgets.
“This calls for professionals in these fields to not only focus on service provision within their spaces but to also embark on effective advocacy to get a slice of the ever-constrained healthcare budgets”
The only effective way to reduce the incidence of hearing impairment and deafness in LMIC lies in prevention, early detection, treatment and rehabilitation of affected individuals. For such programmes to be effective, they rely on a well-trained and motivated human resource. This therefore calls for a focused approach to training, capacity development and retention of skilled manpower around otology, ear and hearing care initiatives.
Otology training, by nature, is capital and resource intensive. It is therefore not surprising that most governments in LMIC do not prioritise otology training. Once trained, ear and hearing care specialists are highly marketable globally. This poses an additional headache to LMIC governments who find themselves competing with richer nations for this precious and finite resource. In many cases, professionals do migrate to better remunerated environments with better working conditions. The result is a critical shortage of ear and hearing care specialists where they are needed most.
“Since 2016, Zimbabwe has embarked on high‑level otology training by fostering effective collaborations with leading institutions worldwide”
Is there a solution to this quagmire, one may wonder? High-level otology training in LMIC is possible through effective collaborations. Since 2016, Zimbabwe has embarked on high-level otology training by fostering effective collaborations with leading institutions worldwide. By sticking to a theme where the primary goal of our collaborative work is focused on training and capacity development, with service provision occurring as a by-product of our training activities, we have managed to upscale skills in otology in our region. There is no shortage of people of good will around the world whose focus is to reach out and make a difference to the lives of the needy. The key to providing effective, impactful, and sustainable otology training in LMIC lies in having clearly defined collaborative frameworks with like-minded individuals in LMIC and global leaders in otology.
One such model we have used effectively since 2016 is to run an annual Regional Temporal Bone Dissection Course in Harare. This course, which is fully supported by the International Federation of Otorhinolaryngological Societies (IFOS), has seen a great improvement of otological skills in our region. The course is attended by leaders in otology in our region and offers wet lab facilities for temporal bone dissection, didactic lectures on ear and hearing care, and live surgeries.
“Besides the upscaling of otology skills, which is the main focus of this regional activity, we have seen positive domino effects around ear and hearing care, which were unexpected”
Besides the upscaling of otology skills, which is the main focus of this regional activity, we have seen positive domino effects around ear and hearing care, which were unexpected. These positive domino effects include a general improvement of audiology services as well as speech and language services which have developed to support the high-end otology procedures taking place in the region.
Another positive outcome of the regular coming together of the thought leaders in otology, both at regional and international levels, has been the development of a robust regional Ear and Hearing Care Forum. Through this forum there is a free flow of information from international bodies like the World Health Organisation (WHO) and International Donor Organisation, as well as universities and training institutes in our region.
Otology training in LMIC is pivotal to meet the huge need of human resources. With smart thinking and effective collaborations, such training can be offered with great results.