As tonsillectomy rates for recurrent sore throats have declined, there has been increasing recognition of the importance of OSA in children. Not always diagnosed early – or in some cases at all – and with continuing debate as to how best to diagnose, investigate and treat it, OSA is now perhaps the single commonest condition to present in a children’s ORL clinic. This article outlines current thinking and imparts some sensible practical advice, much of it based on qualitative data from parents and clinicians.
“Well, it disturbed my sleep, so it had an effect on me because I was constantly watching her and making sure she was breathing.”
Parent of a child with obstructive sleep apnoea [1].
Obstructive sleep apnoea (OSA) and sleep-disordered breathing, which encompasses both OSA and primary snoring, are very common conditions in children, with a prevalence of 2% and 10% in the UK respectively. The problems have been recognised for a long time. ‘On Some Causes of Backwardness and Stupidity in Children’ was printed in the BMJ in 1889 and, despite the blunt title, featured a good description of obstructive sleep apnoea, its impact on quality of life and symptomatic improvement following adenoid surgery.
The number of adenotonsillectomies for obstruction is increasing. In the NHS there were 318,453 paediatric tonsillectomies between 2008 and 2019 and it is estimated that at least 35% of these were for airway obstruction - including a higher proportion in younger children [2]. But how well do we understand this condition and the best treatment strategies for it? As the quotation above from our qualitative study of OSA pathways demonstrates, this is important for patients and families [1].
"A history of habitual snoring with large tonsils and sleep disturbance has a high sensitivity for obstructive sleep apnoea, but the absence of apnoeas in the history has a low specificity"

Figure 1. One of the earliest papers to outline obstructive sleep apnoea symptoms.
It is rare for infants without comorbidity to develop symptoms of OSA. From the age of one to two, with an increasing exposure to infections and childcare settings, lymphoid hypertrophy of the tonsils and adenoids begins to have an impact on airflow through the post-nasal space and oropharynx. There is a dynamic element to the obstruction in addition to that caused by tonsil and adenoid size. The dynamic element relates mostly to the tone within the oropharynx and hypopharynx, which have a boundary of pharyngeal constrictor muscle. During the sleep cycle rapid eye movement (REM) sleep happens, which is associated with dreaming. During this phase muscles relax, including pharyngeal muscles. The combination of this with adenotonsillar hypertrophy results in snoring with partial or complete obstruction of the airway, worse during REM sleep.
The condition is not always recognised. It is likely that there are patients with undiagnosed sleep apnoea in the community, while others who have milder forms of the condition may be referred for treatment. The quotes from our pathway study demonstrate some of the issues for professionals and parents.
“She’s always made a bit of a noise when she was a baby. I just put it down to being normal because nobody told me. The health visitor witnessed her sleeping, and nobody really said, ‘Oh, that’s not normal.’ So, I didn’t really realise.”
Parent of a child with obstructive sleep apnoea.
“I’ve seen more for sleep-disordered breathing, rather than tonsillitis now… Fifteen years ago, it would have pretty much all been tonsillitis. The guidelines for not doing as many tonsillectomies for tonsillitis has certainly had an impact, I think.”
General practitioner.
A history of habitual snoring with large tonsils and sleep disturbance has a high sensitivity for obstructive sleep apnoea, but the absence of apnoeas in the history has a low specificity. This may reflect the fact that apnoeas occur with more frequency later in the sleep cycle (when REM sleep is more prevalent), and the parents are not observing the whole sleep pattern. Adding to the challenge is that in meta-analyses, symptoms correlate poorly with the results of sleep investigations. Even a recent study of smartphone video recordings has shown limited correlation with sleep study results, although less concerning videos were more likely to be correlated with milder degrees of OSA.
A pragmatic approach is currently required and widely applied. The presence of habitual snoring, witnessed apnoeas, sleep disturbance, daytime symptoms of tiredness combined with positive examination findings of deceased nasal airflow and large tonsils help build a clinical diagnosis. Much of these data can be captured formally in quality of life questionnaires, such as the OSA 18 or the T14.
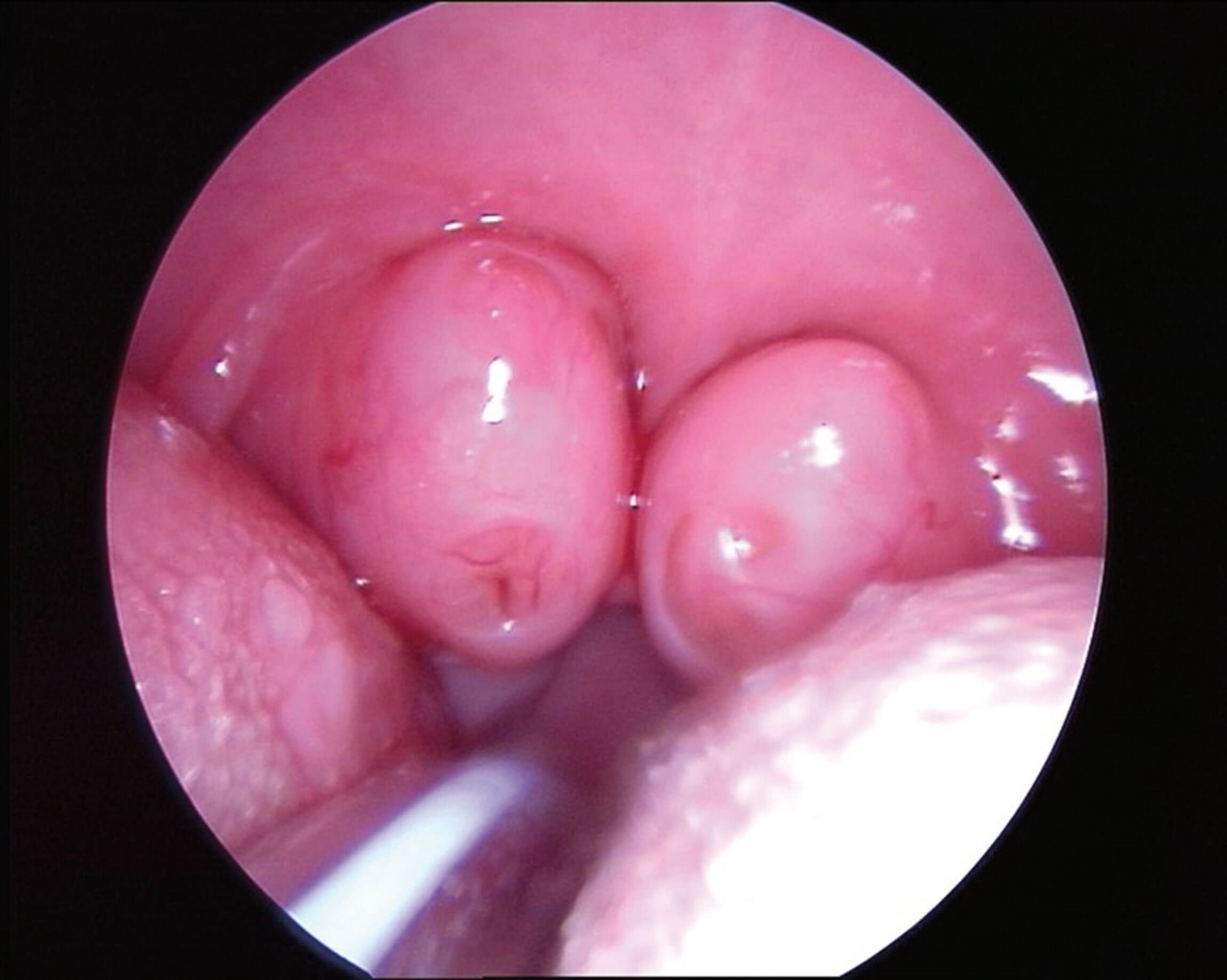
Figure 2. Tonsillar hypertrophy.
Sleep investigation has some benefits but also limitations. Pulse oximetry can demonstrate clusters of desaturation which can correlate with OSA. A ‘positive’ oximetry with clusters of desaturation combined with clinical features has a high positive predictive value for obstructive sleep apnoea, but a ‘negative’ oximetry without desaturation cannot exclude apnoea. This is due to the fact that milder degrees of apnoea may not result in desaturation. Polysomnography or sleep studies refer to a more detailed set of investigations which are most commonly undertaken overnight in hospital. This means that obstructive apnoeas can be differentiated from central apnoeas. Although there is use in defining the physiological characteristics of obstruction, the results often don’t correlate well with parental perception of quality of life before or after surgery. They are best reserved for complicated cases or where there is uncertainty about diagnosis, residual symptoms or comorbidity.
There have now been some major studies looking at adenotonsillectomy in the treatment of OSA. The Childhood Adenotonsillectomy Trial (CHAT) studied children aged five to nine years [3]. The primary neuro-behavioural outcome was not different between surgery versus watchful waiting, but quality of life and sleep study measures did improve. There was also a 46% improvement in sleep study results in the watchful waiting group, reflecting the older age group in this study where spontaneous improvement can be expected. Quality of life scores did not correlate well with the sleep study results.
The Preschool Obstructive Sleep Apnea Tonsillectomy and Adenoidectomy (POSTA) study enrolled younger children, aged three to five, to adenotonsillectomy or watchful waiting [4]. Similar to the CHAT study, cognitive improvement was not shown, but there were significant improvements in quality of life and sleep.
Quality of life and sleep are certainly areas which concern parents, many of whom may wish to consider adenotonsillectomy. Intracapsular coblation adenotonsillectomy has changed the safety outlook of surgery for patients with this condition. Our large cohort study demonstrated that, with intracapsular coblation, secondary haemorrhage is 1.2% and return to theatre just 0.2%. Regrowth requiring intervention is 2.2% at five years [5].
More work is needed in this area to define patients who are likely to benefit most from treatment and to streamline pathways. Currently a pragmatic approach to obstructive sleep apnoea, understanding the limitations of history and investigations, and the benefits of adenotonsillectomy can help facilitate significant improvement in quality of life for both children and families.
Hear more about the latest developments in paediatric obstructive sleep apnoea at ESPO Liverpool 2023.
References
1. Haighton C, Watson RM, Wilson JA, Powell S. Perspectives on paediatric sleep-disordered breathing in the UK: a qualitative study. J Laryngol Otol 2022;136(6):520-6.
2. Keltie K, Donne A, Daniel M, et al. Paediatric tonsillectomy in England: A cohort study of clinical practice and outcomes using Hospital Episode Statistics data (2008-2019). Clin Otolaryngol 2021;46(3):552-61.
3. Marcus CL, Moore RH, Rosen CL, et al. A randomized trial of adenotonsillectomy for childhood sleep apnea. N Engl J Med 2013;368(25):2366-76.
4. Waters KA, Chawla J, Harris MA, et al. Cognition After Early Tonsillectomy for Mild OSA. Pediatrics 2020;145(2).
5. Powell S, Tweedie DJ, Jonas NE, et al. Coblation intracapsular tonsillectomy: A cohort study of NHS practice in England using Hospital Episode Statistics. Clin Otolaryngol 2022;47(3):471-7.