Tinnitus - the perception of sound in the absence of an external source - continues to intrigue, perplex, and infuriate clinicians, researchers and sufferers. The authors here present an overview of the current approaches to tinnitus.
Whilst there are various therapeutic options for ameliorating the impact of tinnitus, there is no current approved treatment for attempting to eradicate, or even for reducing, the loudness of tinnitus. Various reasons have been suggested to try and explain why searching for a tinnitus cure has proved so unproductive [1]: the pathophysiology is incompletely understood; the size of the problem is unclear – prevalence estimates have varied from 5.1% to 42.7% of the population; there are multiple subtypes of tinnitus; animal models exist but research using these models often fails to translate to human tinnitus; there is no objective way of measuring tinnitus and no known biomarker for tinnitus; even the definition of tinnitus has come in for criticism. Modern research has clarified some of these areas but there are still many questions to be answered.
Tinnitus definitions
In an attempt to produce a robust tinnitus definition, an international working group has proposed that the word ‘tinnitus’ should refer to awareness of a noise with no corresponding external source and when this awareness is associated with emotional distress, that should be called ‘tinnitus disorder’ [2]. This suggestion has been welcomed by some but criticised by others and has not addressed some of the issues, such as how to exclude psychiatric hallucinations from the tinnitus definition.

Artist’s depiction of tinnitus.
Epidemiology and big data
The ability to collect, manipulate and analyse large quantities of data has improved enormously over the last quarter of the century, and these skills have been adopted by tinnitus researchers. Exploring the heterogeneity of tinnitus requires studying the characteristics of large numbers of tinnitus sufferers. Some work has been done using existing general biobanks, but tinnitus-relevant information is often lacking in these resources. Development of large-scale clinical databases and/or tinnitus-specific biobanks is urgently required. Use of big data is also helping to produce more accurate estimates of tinnitus prevalence and incidence, and is allowing us to better explore the association of tinnitus with other medical conditions [3].
SEE ALSO
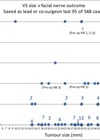
Positive causal associations were found for various hearing-related factors and several non-otological risk factors including temporo-mandibular joint disorder, depression, chronic obstructive pulmonary disease, and hyperlipidaemia. Negative, possibly protective, associations were found for diabetes and high alcohol consumption. No associations were found for low alcohol consumption, body mass index, head injury, heart failure, hypertension, leisure noise exposure, migraine, rheumatoid arthritis, sex, smoking, stroke, and whiplash.
Psychological management
Psychological therapies remain the treatment options with the best scientific evidence of efficacy. Cognitive behavioural therapy (CBT), mindfulness-based cognitive therapy (MBCT) and acceptance and commitment therapy (ACT) have all shown positive effects when investigated using randomised control trials. Unfortunately, there is a dearth of therapists who are both qualified to deliver these treatments and have the necessary tinnitus knowledge. Proof of concept studies have shown that CBT for tinnitus can be successfully delivered via the internet [4] and there are plans to introduce this into clinical practice in the UK as part of the Improving Access to Psychological Therapies (IAPT) programme. Psychological therapies continue to evolve, and it is likely that we will see other modalities used for tinnitus, particularly from the fourth wave of cognitive therapies.
A child’s drawing, depicting his tinnitus as ringing bells.
Drug treatments
For many in the tinnitus world, development of a tinnitus drug is the ultimate goal. Although such compounds remain elusive, there have been some drug trials that got tantalisingly close to a solution. Retigabine (or ezogabine in the USA) is a drug that was primarily developed for its anticonvulsant properties, acting on a subgroup of neuronal potassium channels called voltage-gated Kv7 channels. Research on rodents suggested efficacy against tinnitus and reports emerged on the internet that it was similarly effective for some human subjects, though this was never tested in a scientifically controlled trial. Unfortunately, retigabine had significant side effects and was withdrawn from clinical usage by the manufacturer in 2017.
"Psychological therapies remain the treatment options with the best scientific evidence of efficacy"
Another drug that was developed for use in epilepsy, selurampanel, is as an orally active, competitive AMPA glutamate receptor antagonist. This was investigated for tinnitus efficacy in a double-blind placebo-controlled randomised controlled trial, and measures of both tinnitus impact and tinnitus loudness improved during treatment. Short-term adverse effects were mostly mild but unfortunately long-term administration to mice resulted in the emergence of both benign and malignant tumours. Further development of the drug was therefore halted.
Bimodal neuromodulation
Bimodal neuromodulation is a technique that combines sound therapy with simultaneous stimulation of a non-auditory neural pathway [5]. Stimulation of the trigeminal, vagal, or upper cervical nerves have been investigated. A commercial device is now available that combines sound stimulation with gentle electrical stimulation of the anterior tongue. Initial results are optimistic but independent and more rigorously controlled studies are required.
Transcranial electromagnetic stimulation
Various forms of electromagnetic stimulation have been explored for use in tinnitus, with treatments directed at both peripheral and central auditory systems and associated areas of the wider central nervous system. The two most rigorously investigated modalities are repetitive transcranial magnetic stimulation (rTMS) and transcranial direct current stimulation (tDCS) [5]. A strong varying magnetic field is applied over the scalp in rTMS to induce electric currents in the superficial layers of underlying brain tissue. There is now a solid evidence base in support of rTMS in the management of treatment resistant depression, but it took large-scale multisite trials to work out which patients should be treated, and which stimulation protocols should be used. Tinnitus trials have used heterogenous study designs and have generally investigated small numbers of participants. Several editorials have highlighted this issue surrounding tinnitus research and have suggested that a large multicentre study is required. In contrast to inducing electrical activity in the brain using magnetic fields, tDCS applies low power electrical stimulation directly to the scalp. Evidence regarding tDCS is still emergent, but it does seem helpful for some people with depression and schizophrenia. There is conflicting evidence regarding its efficacy for tinnitus, and further research in this area is needed.
Conclusions
Understanding tinnitus and developing effective treatments has never been easy but there is now a more structured and collaborative research network trying to solve the puzzle.
References
1. McFerran DJ, Stockdale D, Holme R, et al. Why Is There No Cure for Tinnitus? Front Neurosci 2019;13:802.
2. De Ridder D, Schlee W, Vanneste S, et al. Tinnitus and tinnitus disorder: Theoretical and operational definitions (an international multidisciplinary proposal). Prog Brain Res 2021;260:1-25.
3. Biswas R, Genitsaridi E, Trpchevska N, et al. Low Evidence for Tinnitus Risk Factors: A Systematic Review and Meta-analysis. J Assoc Res Otolaryngol 2022;Epub ahead of print.
4. Beukes EW, Manchaiah V, Allen PM, et al. Internet-Based Interventions for Adults With Hearing Loss, Tinnitus, and Vestibular Disorders: A Systematic Review and Meta-Analysis. Trends Hear 2019;23:2331216519851749.
5. Langguth B. Non-Invasive Neuromodulation for Tinnitus. J Audiol Otol 2020;24(3):113-8.